What if there was a treatment strategy that did not involve medicines or surgeries to manage a wide range of medical conditions? Hyperbaric oxygen therapy has made it possible. It was first used in the U.S. in the early 1900s. Over the past 40 years, people have been utilizing this therapy to avoid the complications associated with other medical procedures.
What is Hyperbaric Oxygen Therapy?
Hyperbaric oxygen therapy (HBOT) is a treatment modality in which a person breathes 100% O2 while exposed to increased atmospheric pressure. It is an adjunctive therapy for acute traumatic and ischaemic injuries, such as crush injuries, compartment syndromes, situations of vascular compromise, decompression sickness, a hazard of scuba diving and carbon monoxide poisoning, clostridial infections. Our body possesses a remarkable capacity to heal itself after any severe injury, but chronic wounds take a little longer time to heal and sometimes complete healing also cannot be possible. Recent advances in treatment approaches have made a significant breakthrough in healthcare by developing an excellent mode of treatment that facilitates wound healing. By using the healing power of oxygen, scientists have developed hyperbaric oxygen therapy, which plays a vital role in complex wound healing. It enhances the body's natural healing process by keeping the patient in a pressurized chamber. It boosts the oxygen supply so that wounds can heal faster and efficiently.
How Does it Work?
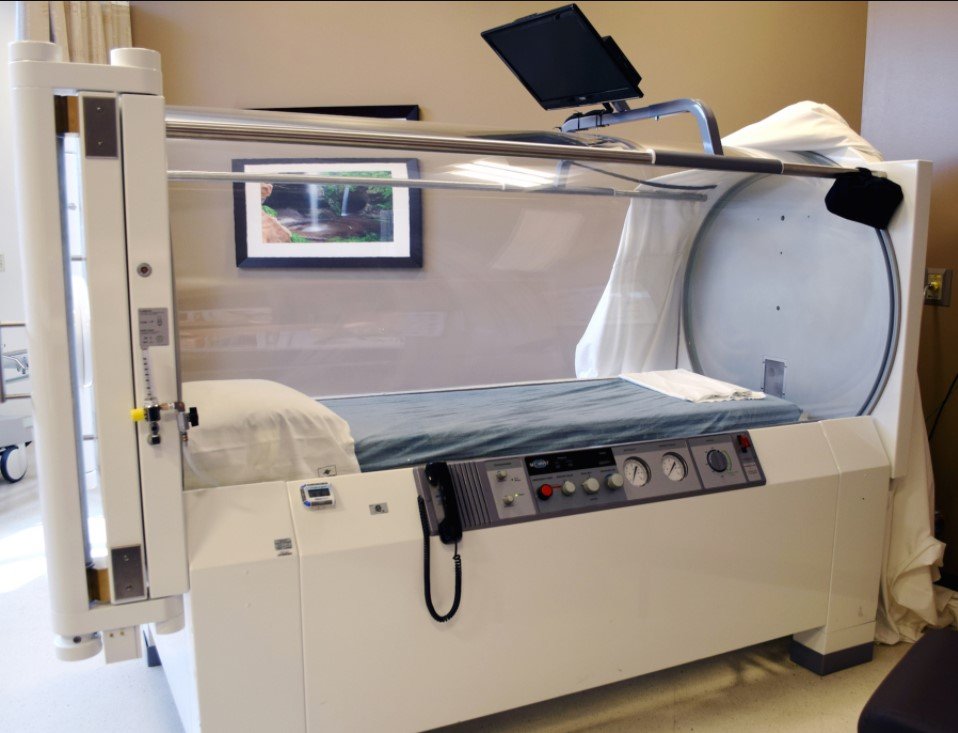
The tube-like HBOT chamber is made up of clear acrylic which is transparent and helps people see outside the chamber. During HBOT, as the pressure increases, the patient breathes the air inside the tube. The pressure inside the chamber usually is two to three times greater than outside air pressure, which means that the patient is inhaling 100% oxygen. The increased amount of oxygen rapidly gets delivered into the bloodstream of the patient and is absorbed into the tissues, plasma and major organs. Due to the improved circulation of oxygen in the body, the body jumpstarts its wound healing process.
What to Expect from this Therapy?
HBOT exerts significant physiological and pharmacological effects that improve cellular, tissue, and organ oxygenation and possesses anti-inflammatory, antibacterial effects.
i. Physiological Effects
The average human requires around 6 mL of O2/dL of blood to maintain metabolism. Therefore, HBOT provides sufficient plasma oxygen to drive cellular respiration. High levels of oxygen decrease local nitric oxide (NO) production by endothelial cells, thereby leading to vasoconstriction. This is especially important, related to cerebral blood flow as short-term hyperoxia causes cerebral vasoconstriction and reduced blood flow.
ii. Pharmacological Effects
Adjunctive HBOT speeds up the wound healing process. Increased arterial oxygen tension of HBOT promotes modulation of a number of growth factors, leading to enhanced healing. Oxygen also has antibacterial effects at wound sites. As soon as any injury occurs, neutrophils and macrophages arrive at the wound site and consume large amounts of oxygen to create hydrogen peroxide, superoxide anions, hydrochloric acid, and hydroxyl radicals. These reactive oxygen species (ROS) can then kill bacteria intracellularly and extracellularly through membrane disruption and protein denaturation through indirect and direct mechanisms. HBOT promotes neutrophil-mediated bacterial killing ability in hypoxic tissue. It also prevents the release of proteases and free radicals in specific injuries, thereby decreasing vasoconstriction, edema, and cellular damage.
Reversing the aging process is quite a fascinating idea and by achieving this, HBOT has drawn the attention of researchers worldwide. A recent study has revealed that hyperbaric oxygen therapy has the potential to reverse the aging process. As we grow older, our cells continue to divide and the telomeres gradually become shorter and can no longer divide. Shortening of telomeres results in aging in humans. HBOT reverses aging processes by preventing the shortening of telomere and decreases the number of senescent cells. Another important benefit of HBOT has been uncovered recently. It has the potential to reduce the ill effects of cytokine storm in COVID-19 patients. Though there is limited literature available on HBOT in COVID-19 patients, considering the present need for additional supportive therapy to improve oxygenation, HBOT has been proposed as a novel supportive treatment in COVID-19 patients.
Pros and Cons
HBOT has successfully treated many conditions such as stroke, severe anemia, decompression sickness, gangrene, burns, sudden deafness, cerebral palsy, head injuries and chronic fatigue. It increases the amount of oxygen in the patient's blood. This is called hyperoxia. The Food and Drug Administration (FDA) has approved HBOT treatment for 14 conditions, including non-healing wounds, stroke, carbon monoxide poisoning, burns, and ischemia, amongst many others.
Hyperbaric oxygen therapy has a role in modern medical practice. The therapy lasts for as little as 3 minutes to as long as 2 hours before the pressure becomes normalized in the chamber. Most people benefit from this therapy but like any other medical treatment, HBOT also carries few side effects. The therapy is not at all suitable for claustrophobic people. Due to the confined and enclosed nature of the hyperbaric chamber, some patients can develop a feeling of claustrophobia. Vision changes, finger numbness, oxygen poisoning, lung damage, barotrauma are possible side effects. Sometimes, hyperbaric oxygen therapy results in worsening myopia. It may cause cataracts to mature faster than usual.
Although hyperbaric chamber therapy is not yet thought of as a type of mainstream medical treatment, there is clinical research evidence that backs the efficacy and safety of this treatment for several conditions. Patients must consult doctors before undergoing HBOT to ensure safety and it should be performed under strict medical supervision. Although this therapy has unlocked the door of a novel treatment strategy, further definitive studies are required to conclusively prove its efficacy and safety.