Siliconoma a Diagnosing dilemma, A Case Report
A B S T R A C T
Silicone implants have been widely used for breast reconstruction and augmentation for years. One of the potential complications of these implants is rupture. Once rupture they start a granulomatous foreign body reaction in the surrounding tissue. The resulting mass formation poses diagnostic difficulties for the surgeons, as it mimics cancer. We report a case of 40 years female who underwent bilateral mastectomy and immediate reconstruction with implants, later presented with a mass. We suspect it local recurrence of tumor on initial presentation and radiology. Definitive diagnosis was only made after complete excision of the mass and histopathology report. No further treatment required and patient doing well.
Keywords
Siliconoma, mimics local recurrence, diagnostic dilemma
Introduction
Silicone prosthesis has been introduced in 1960s, since then they have been widely used for breast augmentation and reconstruction purpose. There are several forms of silicone in medical use: silicone oil, silicone gel and silicone elastomers. For breast mainly silicone gel is used. It is considered biologically inert, class III medical device of limited product life. These devices carry a potential complication of rupture, which can be due to damage during implantation, damage during other surgical procedures, and chemical degradation of the implant shell, trauma and mechanical pressure of mammographic examination. Once ruptured the silicone gel starts to migrate from the chest wall to other parts of body, most commonly to breast and armpit. It manifests as granulomas and axillary lymphadenopathy [1]. In some cases, it can be asymptomatic [2]. Silicone implant rupture can be evaluated using magnetic resonance imaging (MRI); from the long-term MRI data for single-lumen breast implants, the European literature about second-generation silicone-gel breast implants, reported silent device-rupture rates of 8-15% at 10 years post-implantation (15-30% patients) [3]. A Meta-analysis in 2011 reported that breast screening MRIs of asymptomatic women might overestimate the incidence of breast implant rupture [4]. Winer et al first described the histopathology of siliconoma as foreign body granulomatous inflammation with dense infiltrate consisting of plasma cells, lymphocytes and histiocytes. Siliconomas can occur locally or present at a distant site due to its high fat solubility. If left un-noticed it can form a firm to hard mass, can cause local tissue destruction, ulceration, scarring and nerve damage [2]. This mass can bring significant concern to the patient and also to the surgeon. Although they have characteristic diagnostic features on imaging, but their appearance can mimic a recurrence of underlying malignancy [5].
Case Presentation
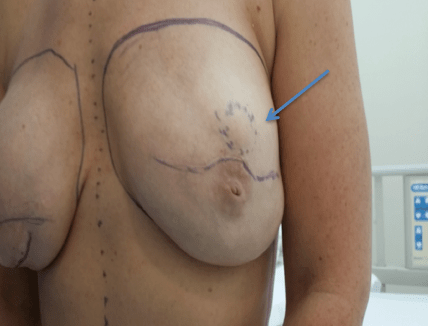
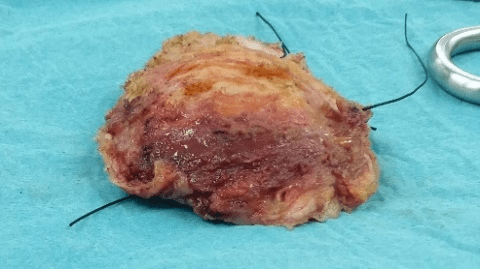
40 years female, nulliparous presented to the breast clinic with complain of recently felt a mass in her right breast on self-examination. Also noticed pulling sensation and heaviness. Clinically the right breast looks bigger than left, bilateral nipple inversion, 2-3cm hard, mobile mass at 9o’clock in the right breast. Plan to do ultrasound and core biopsy. Ultrasound showed irregular hypo echoic mass 2.5*1.5cm in the right breast, core biopsy with marker placement was done. Axilla showed few lymph nodes. Histopathology turned out as mucinous carcinoma, estrogen and progesterone receptor positive. Patient was counseled for right mastectomy and sentinel lymph node biopsy, also risk reducing left mastectomy. Procedure was done as planned, bilateral mastectomy, right sentinel lymph node biopsy, Latisimus dorsi flap and implants on both sides. All the wounds healed very well. Postoperative patient was started on tamoxifen. She was regular in her follow up and annual screening. After about 4 years patient developed a non-tender hard swelling of around 4*2cm on the left breast at 12o’clock (Figure 1). Clinical suspicion was of recurrence, as the mass was hard in consistency with irregular margins. Ultrasound was done that showed a cystic lesion but inconclusive. MRI was planned next and showed extra capsular rupture of the left implant, a mass of about 5.6*1.9cm in the upper quadrant, radiological features of this mass were inconclusive and enlarged axillary nodes. It was highly recommended by the radiologist that this mass to be biopsied. Enlarged axillary nodes were still of concern, hence excision of the mass was planned. The mass was excised, and bilateral change of implants was also done (Figure 2). Final histopathology of the mass came out to be a silicone granuloma. Which does not require any further treatment after complete excision.
Figure 1: Showing the mass.
Figure 2: The specimen after excision.
Discussion
Siliconomas develop as a result of implant rupture and can present as a mass resembling carcinoma or recurrence. They usually develop at around 4 weeks to 16 years after rupture. The most common presentation is a mass. Implant rupture may appear on mammogram however dynamic contrast-enhanced MRI is the optimal modality to assess for rupture and siliconoma formation. MRI findings include collapse of implant and free silicone particle outside the shell. The PET-CT can yield false positive results in patients [5]. Core biopsy does not always exclude malignancy from the mass in most of the cases; hence excision is required most of the time. Histopathology remains the gold standard for diagnosing siliconoma. A high index of suspicion is required while dealing with such patients. The swelling of siliconoma can be easily mistaken as a tumor, or a recurrence because of its appearance and consistency, as silicone droplets can travel to different body tissues and axillary lymph nodes. It can easily mislead a surgeon. Hence a complete background history is crucial. We present this case to emphasize that siliconoma can be difficult to diagnose on imaging and a complete surgical excision is required to reach a final diagnosis.
Article Info
Article Type
Case ReportPublication history
Received: Sat 05, Oct 2019Accepted: Thu 24, Oct 2019
Published: Thu 31, Oct 2019
Copyright
© 2023 Rabbia Khan. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited. Hosting by Science Repository.DOI: 10.31487/j.SCR.2019.05.11
Author Info
Annett Al Hamadi Faisel Ikram Rabbia Khan Yasser Khattab
Corresponding Author
Rabbia KhanMediclinic City Hospital, Dubai
Figures & Tables
References
- Katzin WE, Centeno JA, Feng LJ, Kiley M, Mullick FG (2005) Pathology of Lymph Nodes from Patients with Breast Implants: A Histologic and Spectroscopic Evaluation. Am J Surg Pathol 29: 506-511. [Crossref]
- Brown SL, Silverman BG, Berg WA (1977) Rupture of silicone-gel breast implants: causes, sequelae, and diagnosis. Lancet 350: 1531-1537 [Crossref]
- Hölmich LR1, Friis S, Fryzek JP, Vejborg IM, Conrad C et al. (2003) Incidence of Silicone Breast Implant Rupture. Arch Surg 138: 801-806. [Crossref]
- Song JW1, Kim HM, Bellfi LT, Chung KC (2011) The Effect of Study design Biases on the Diagnostic Accuracy of Magnetic Resonance Imaging for Detecting Silicone Breast Implant Ruptures: a Meta-analysis. Plast Reconstr Surg. 127: 1029-1044. [Crossref]
- Adejolu M, Huo L, Rohren E, Santiago L, Yang WT (2012) False-positive lesions mimicking breast cancer on FDG PET and PET/CT. AJR Am J Roentgenol 198: W304-W314. [Crossref]
