Sepsis Due to Port-Site Abscess in Laparoscopic Pelvic Lymphadenectomy: A Case Report
A B S T R A C T
Port-site infection is one of the most frequent complications in gynaecological laparoscopy. We present a rare case of port-site infection complicated by an abdominal wall abscess and sepsis. We conduct a literature review and discuss the difficulties of diagnosis and the management of this clinical situation.
Keywords
Laparoscopic surgery, port-site infection, sepsis, abscess
Introduction
Gynaecological laparoscopy is a frequent surgical procedure worldwide [1]. The advantages of minimal access surgery are well known: fewer postoperative complications, early postoperative recovery, less pain, and early return to work [2]. However, laparoscopy presents certain complications. One of the most frequent is port-site infection, with an incidence of around 8-11% depending on the procedure [3]. The most common location is the umbilical port [4]. We present a case of infection of the port-site in a patient after pelvic lymphadenectomy for endometrial cancer, complicated by an abdominal wall abscess and sepsis. We discuss the difficulty of diagnosis and management.
Case Report
A 46-year-old female was referred to our center for hypermenorrhea and suspicion of polyp or myoma. Hysteroscopy was performed, and a polypoid structure was excised. The histological analysis revealed endometrial carcinoma, and a magnetic resonance scan was performed to evaluate its extension. The patient underwent a laparoscopic hysterectomy with bilateral adnexectomy for endometrial carcinoma stage Ia G2. Postoperative evolution was satisfactory, and the patient was discharged on the second day of admission. The final histological result was endometrioid endometrial cancer stage IBG2, due to a myometrial infiltration superior to 50%. Laparoscopic pelvic lymphadenectomy was indicated to rule out lymphatic dissemination. The laparoscopic procedure was uneventful. Twenty-four hours after surgery, the patient presented fever of 38.9ºC and abdominal distension. A computed tomography (CT) scan was performed in order to rule out digestive injury (Figures 1-3), along with a blood test and culture. The CT revealed no pathological collections, and the blood test did not show leukocytosis, and so anti-thermic medication was administered, with a positive response. Urine infection was ruled out by examination of urine sediment.
Forty-eight hours after surgery, the patient once again presented fever of 38ºC, abdominal distension and pain in the surgical wound at the site of the right pelvic trocar, without erythema or signs of wound infection. A blood test revealed a leukocyte count of 18,700 with 26% of bands, C-reactive protein 390, procalcitonin 1.13ng/ml (n<0.5) and lactate 1.70mmol/L (n0.5-1.8). Treatment with piperacillin tazobactam was initiated. Another blood test 12 hours later revealed 16,700 leukocytes, C-reactive protein 420.2, procalcitonin 1.8ng/ml (n<0.5), lactate 1.9mmol/L (n0.5-1.8) and prothrombin time of 55%. The patient presented tachycardia (115pul/min), fever of 37.8ºC and hypotension (99/58). With the diagnosis of sepsis, she was transferred to the intensive care unit. A new CT revealed abdominal liquid and mild pneumoperitoneum, but no abdominal collections. The patient presented satisfactory evolution, the fever disappeared, and the blood infection parameters returned to normal. Six days after surgery the surgical wound of the right pelvic trocar presented erythema, the stitches were removed, and the abundant purulent liquid exiting the area was cultured. Washes of the surgical infected port-site wound were performed, and the blood and wound cultures were negative. The patient was discharged 12 days after the admission.
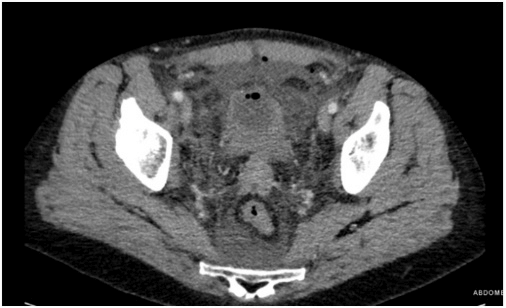
Figure 1: Axial CT. Free fluid in pelvis. Air bubble in urinary bladder. Pneumoperitoneum bubble.
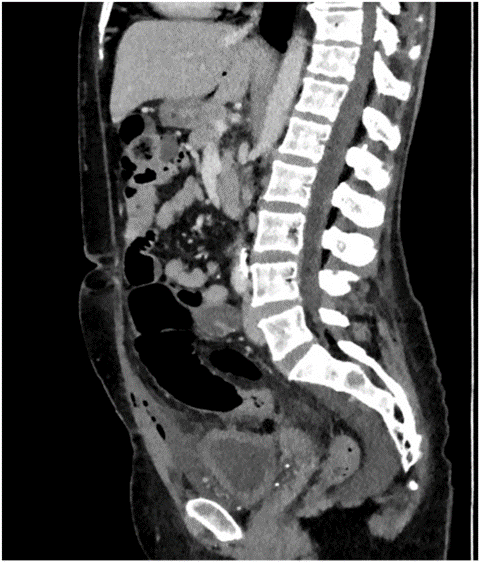
Figure 2: Sagittal reconstruction CT.
Figure 3: Coronal reconstruction CT.
Discussion
Among patients undergoing gynaecological laparoscopy surgical site infections are more common than might be expected; indeed, one recent study recorded a rate of 16.3% [1]. The port-site is one of the most frequent locations of infection (10.2% in the study just referenced) [1]. Nonetheless, surgical wound infection is significantly higher in open surgery than in laparoscopy [5]. Our exhaustive literature revision did not identify any cases of sepsis due to a port-site abscess. In our case, the diagnosis was made after ruling out digestive tract injury, which is the most frequent cause of fever and sepsis after laparoscopy. CT was not able to detect the port-site abscess, and the absence of signs of abdominal collections that might suggest digestive injury led us to apply conservative management with broad-spectrum antibiotic therapy. The definitive diagnosis was made six days after the procedure, when the port-site wound presented signs of infection and draining of purulent liquid after the opening of the wound. This case should alert surgeons to the possible importance of port-site infections in laparoscopic procedures.
Competing Interests
None.
Ethical Approval
The study was approved by the Research Ethics Committee of the Sant Joan de Déu Foundation.
Consent
Signed consent has been obtained from the patient.
Article Info
Article Type
Case ReportPublication history
Received: Tue 04, May 2021Accepted: Tue 18, May 2021
Published: Fri 04, Jun 2021
Copyright
© 2023 Eduardo Gonzalez Bosquet. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited. Hosting by Science Repository.DOI: 10.31487/j.SCR.2021.06.02
Author Info
Eduardo Gonzalez Bosquet Laia Grau Paulino Sousa Cacheiro
Corresponding Author
Eduardo Gonzalez BosquetObstetric and gynecology Department, Sant Joan de Déu Hospital, University of Barcelona, Spain
Figures & Tables

References
1. Dior UP,
Kathurusinghe S, Cheng C, Reddington C, Daley AJ et al. (2020) Effect of
Surgical Skin Antisepsis on Surgical Site Infections in Patients Undergoing
Gynecological Laparoscopic Surgery: A Double-Blind Randomized Clinical Trial. JAMA
Surg 155: 807-815. [Crossref]
2. Sasmal PK, Mishra
TS, Rath S, Meher S, Mohapatra D (2015) Port site infection in laparoscopic
surgery: A review of its management. World J Clin Cases 3: 864-871. [Crossref]
3. Hamzaoglu I, Baca
B, Böler DE, Polat E, Ozer Y (2004) Is umbilical flora responsible for wound
infection after laparoscopic surgery? Surg Laparosc Endosc Percutan Tech 14:
263-267. [Crossref]
4. Richards C, Edwards
J, Culver D, Emori TG, Tolson J et al. (2003) Does using a laparoscopic
approach to cholecystectomy decrease the risk of surgical site infection? Ann
Surg 237: 358-362. [Crossref]
5.
Li YS, Meng FC, Lin JK (2020) Procedural and
post-operative complications associated with laparoscopic versus open abdominal
surgery for right-sided colonic cancer resection: A systematic review and
meta-analysis. Medicine (Baltimore) 99: e22431. [Crossref]
