Resolution of Muscle Tension Dysphonia with Reinke’s Edema Following STRETTA Therapy in a Patient with GERD: A Case Report
A B S T R A C T
Muscle Tension Dysphonia (MTD) is a syndrome involving abnormal vocal cord behaviour due to increased tension of laryngeal musculature. It has a complex etiology, but gastroesophageal reflux disease (GERD) is implicated in up to half of cases. The authors present the first reported case of MTD being successfully treated using STRETTA, an endoscopic radio-frequency therapy, licenced for GERD. Since 2016, a 60-year-old female had symptoms of laryngo-pharyngeal reflux. These included dysphonia, cough, sore throat, and persistent throat clearing. She underwent flexible nasendoscopy demonstrating significant posterior laryngeal edema, and anterior-posterior constriction on phonation, suggestive of MTD. Despite anti-reflux medication, her symptoms persisted. Repeat flexible nasendoscopy demonstrated bilateral Reinke's edema. Her symptoms failed to improve despite incision and drainage of the Reinke’s edema. An EGD demonstrated reflux esophagitis, and a blunt angle of His. She underwent STRETTA and reports significant improvement of symptoms. Repeat nasoendoscopy showed convalescence of the Reinke’s edema. Existing evidence suggests that management of MTD with proton pump inhibitor (PPI) improves reflux symptoms such as chronic cough and heartburn but has a limited effect on measures of voice such as voice range profile, perceptual evaluation, and acoustic analysis. Given that the present patient found subjective improvement in voice quality, it is possible STRETTA may be preferable to PPI in treating MTD with regard to voice, but further assessment of voice quality pre- and post-STRETTA is needed. In LPR refractory to PPI, there is evidence that Laparoscopic Nissen Fundoplication (LNF) is successful; however, the cost-effectiveness of endoscopic anti-reflux procedures such as STRETTA is superior to operative management such as LNF. Therefore, STRETTA may well be more beneficial than both PPI and LNF in the treatment of MTD with LPR.
Keywords
STRETTA, endoscopy, muscle tension dysphonia
Background
Muscle Tension Dysphonia (MTD) is a syndrome with a variety of etiologies leading to abnormal vocal fold behaviour as a result of increased tension of laryngeal musculature [1]. It is subdivided into primary and secondary, the latter whereby the cause is related to structural or neurogenic abnormality. Primary causes are often multifactorial relating to functional disorders, allergy, and gastro-intestinal reflux, with gastroesophageal reflux disease (GERD) a predominant co-morbidity (40-49% of cases) [2, 3].
Laryngopharyngeal reflux (LPR) is the backflow of gastric contents into the larynx, pharynx, and upper aerodigestive tract [4]. LPR is very common, representing around half of laryngeal complaints presenting to ear, nose, and throat (ENT) services [5]. LPR is one of the etiological factors in the development of MTD [1].
LPR is managed with proton pump inhibitors (PPI); however, it is accepted that PPI is less effective for LPR than for typical GERD symptoms [6]. In addition, anti-GERD lifestyle modifications are recommended; these include avoidance of trigger foods, weight loss, reduction of portion size, cessation of alcohol and smoking, avoiding eating immediately before going to bed, and raising the bed head.
Treatment techniques for MTD such as injection laryngoplasty and transcutaneous electrical nerve stimulation, often in combination with vocal therapy, are widely accepted as the gold standard treatment [7-9]. These treatments can result in a positive outcome, though rarely result in complete symptom resolution [7].
STRETTA is a novel endoscopic anti-reflux therapy that uses radio-frequency to stimulate hypertrophy at the gastroesophageal junction (GEJ), augmenting the GEJ to prevent reflux of gastric contents into the esophagus [10]. It has excellent outcomes in patients with GERD [11, 12]. STRETTA is the only radiofrequency anti-reflux therapy approved by NICE for use in the UK [10]. Here, we report the first case of MTD successfully treated with STRETTA therapy.
Case Report
A 60-year-old female had been under follow up from both the ENT and gastroenterology team at James Cook University Hospital since 2016. She had a past medical history of Raynaud’s disease. Since 2016, she had symptoms of LPR. These included dysphonia, cough, sore throat, and persistent throat clearing. In early 2017, she underwent flexible nasendoscopy, which demonstrated significant posterior laryngeal edema, and anterior-posterior constriction on phonation, suggestive of MTD. In light of these findings, she was initiated on PPI and Gaviscon Advance.
Despite anti-reflux medication, her symptoms persisted. Repeated flexible nasendoscopy in 2019 demonstrated persistent MTD and bilateral Reinke's edema secondary to reflux. She underwent incision and drainage of Reinke’s edema on her left vocal cord in April 2019. Unfortunately, despite this, her symptoms persisted.
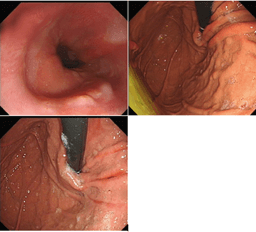
Figure 1: EGD findings pre-STRETTA.
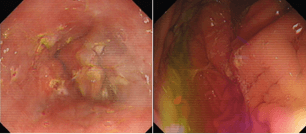
In November 2019, she was referred to the upper GI surgical team for further assessment. A repeat Esophagogastroduodenoscopy (EGD) demonstrated a lax GEJ with retrograde prolapse of gastric mucosa, evidence of reflux oesophagitis, and a blunt angle of His (Figure 1). She also underwent barium swallow, which demonstrated evidence of esophageal dysmotility, there were subtle uncoordinated, non-peristaltic contractions of her esophagus with slow transit on prone swallow, but her esophagus eventually cleared when in an erect position. Her DeMeester score was equivocal. Her 24 hr pH study result was equivocal, and manometry showed preserved peristalsis with a relaxing lower esophageal sphincter (LES) zone. She underwent STRETTA therapy in January 2020, under conscious sedation. Forty-nine out of a total of 56 radiofrequency thermal treatment points were successfully delivered (Figure 2).
Figure 2: Endoscopic images at-STRETTA.
Due to the COVID-19 pandemic, her post-procedure follow-up was via the telephone 4 months after treatment. She reported, feeling much better with improvement in her GERD HRQL scores. Specifically, she reports less acid taste in her mouth along with improvement in her voice, that was normal on the phone, and the patient states her voice has improved. She had a repeat nasendoscopy under ENT, which showed convalescence of the Reinke’s edema. She no longer takes a PPI but does continue to take Gaviscon Advance as and when required, after meals and before bed.
Discussion
Although STRETTA has been documented to reduce hoarseness and voice changes associated with GERD, based upon current published literature, we believe this case to be the first report of the use of STRETTA to successfully treat MTD with LPR [13].
In patients presenting with otolaryngeal symptoms, silent gastroesophageal reflux is often present. Where a patient has a normal pH profile and no reflux symptoms, PPI is of no benefit [14]. On the other hand, where patients have abnormal pH and/or reflux symptoms, PPI improves reflux symptoms such as dysphonia, dysphagia, globus, chronic cough and heartburn [14]. However, PPI has a limited effect on measures of voice such as voice range profile, perceptual evaluation, and acoustic analysis [14, 15]. Given that the present patient found subjective improvement in voice quality, it is possible STRETTA may be preferable to PPI in treating MTD with regard to voice, but a further assessment of voice quality pre- and post-STRETTA is needed. This patient had GERD symptoms persisting despite PPI therapy; this has been shown to occur in 15% of patients with LPR [15]. Given the prevalence of LPR, there are a substantial number of patients with refractory LPR despite PPI that could benefit from STRETTA.
In LPR refractory to PPI, there is evidence that Laparoscopic Nissen Fundoplication (LNF) is successful, with 61% reporting no or only mild laryngitis and 69% had an improved voice quality following surgery [16]. The cost-effectiveness of endoscopic anti-reflux procedures such as STRETTA is superior to operative management such as LNF and becomes more favourable compared with PPI when high doses and long-term therapy is needed [17, 18]. Patients with LPR often require prolonged courses of high dose PPI, and unfortunately, many suffer relapse upon stopping therapy [19]. Therefore, in cases of LPR, STRETTA may be more cost-effective and confer a more durable benefit when compared to life-long high dose PPI, or more invasive surgical procedures with the higher potential risk profile.
To our knowledge, this is the first documented case of muscle tension dysphonia successfully treated with STRETTA therapy. This has resulted in symptom resolution and reduced the patient’s medication burden. Further work is needed to confirm if STRETTA should be used routinely in patients with muscle tension dysphonia.
Abbreviations
MTD: Muscle Tension Dysphonia
GERD: Gastroesophageal Reflux Disease
LPR: Laryngopharyngeal Reflux
ENT: Ear, Nose and Throat
PPI: Proton Pump Inhibitor
GEJ: Gastroesophageal Junction
NICE: National Institute for Health and Care Excellence
EGD: Esophagogastroduodenoscopy
LES: Lower Esophageal Sphincter
LNF: Laparoscopic Nissen Fundoplication
Conflicts of Interest
None.
Author Contributions
Dr J E Dixon: Writing original draft, writing review, editing, ORCID: 0000-0001-7860-710X; Mr E J Nevins: Conceptualisation, writing review, editing, ORCID: 0000-0002-4172-3729; Dr M John: Writing original draft, ORCID: 0000-0003-0994-4019; Prof YKS Viswanath: Conceptualisation, supervision, editing, ORCID: 0000-0003-3880-1172.
Ethical Approval
None.
Consent
The patient consented to the use and publication of her case for research.
Article Info
Article Type
Case ReportPublication history
Received: Tue 22, Dec 2020Accepted: Sat 09, Jan 2021
Published: Tue 19, Jan 2021
Copyright
© 2023 Viswanath YKS. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited. Hosting by Science Repository.DOI: 10.31487/j.SCR.2021.01.10
Author Info
James E Dixon Edward J Nevins Michael John Viswanath YKS
Corresponding Author
Viswanath YKSJames Cook University Hospital, Middlesbrough, Cleveland, UK
Figures & Tables
References
- Van Houtte E, Van Lierde K, Claeys S (2011) Pathophysiology and treatment of muscle tension dysphonia: a review of the current knowledge. J Voice 25: 202-207. [Crossref]
- Cohen SM, Pitman MJ, Noordzij JP, Courey M (2012) Management of dysphonic patients by otolaryngologists. Otolaryngol Head Neck Surg 147: 289-294. [Crossref]
- Altman KW, Atkinson C, Lazarus C (2005) Current and emerging concepts in muscle tension dysphonia: a 30-month review. J Voice 19: 261-267. [Crossref]
- Oguz H, Tarhan E, Korkmaz M, Yilmaz U, Safak MA et al. (2007) Acoustic analysis findings in objective laryngopharyngeal reflux patients. J Voice 21: 203-210. [Crossref]
- Koufman JA, Amin MR, Panetti M (2000) Prevalence of reflux in 113 consecutive patients with laryngeal and voice disorders. Otolaryngol Head Neck Surg 123: 385-388. [Crossref]
- Vaezi MF (2010) Benefit of acid-suppressive therapy in chronic laryngitis: the devil is in the details. Clin Gastroenterol Hepatol 8: 741-742. [Crossref]
- Novakovic D, Nguyen DD, Chacon A, Madill C (2020) Injection laryngoplasty as adjunct treatment method for muscle tension dysphonia: Preliminary findings. Laryngoscope 130: 980-985. [Crossref]
- Mansuri B, Torabinejhad F, Jamshidi AA, Dabirmoghaddam P, Vasaghi Gharamaleki B et al. (2020) Transcutaneous Electrical Nerve Stimulation Combined With Voice Therapy in Women With Muscle Tension Dysphonia. J Voice 34: 490.e11-490.e21. [Crossref]
- Mansuri B, Torabinezhad F, Jamshidi AA, Dabirmoghadam P, Vasaghi Gharamaleki B et al. (2019) Application of High-Frequency Transcutaneous Electrical Nerve Stimulation in Muscle Tension Dysphonia Patients With the Pain Complaint: The Immediate Effect. J Voice 8: 657-666. [Crossref]
- NICE (2016) Stretta System for gastro-oesophageal reflux disease.
- Auyang ED, Carter P, Rauth T, Fanelli RD, SAGES Guidelines Committee (2013) SAGES clinical spotlight review: Endoluminal treatments for gastroesophageal reflux disease (GERD). Surg Endosc 27: 2658-2672. [Crossref]
- Viswanath Y, Maguire N, Obuobi RB, Dhar A, Punnoose S (2019) Endoscopic day case antireflux radiofrequency (Stretta) therapy improves quality of life and reduce proton pump inhibitor (PPI) dependency in patients with gastro-oesophageal reflux disease: a prospective study from a UK tertiary centre. Frontline Gastroenterol 10: 113-119. [Crossref]
- McClusky DA, Khaitan L, Swafford VA, Smith CD (2007) Radiofrequency energy delivery to the lower esophageal sphincter (Stretta procedure) in patients with recurrent reflux after antireflux surgery: can surgery be avoided? Surg Endosc 21: 1207-1211. [Crossref]
- Willems Bloemer LH, Vreeburg GC, Brummer R (2000) Treatment of reflux-related and non-reflux-related dysphonia with profound gastric acid inhibition. Folia Phoniatr Logop 52: 289-294. [Crossref]
- Shaw GY, Searl JP, Young JL, Miner PB (1996) Subjective, laryngoscopic, and acoustic measurements of laryngeal reflux before and after treatment with omeprazole. J Voice 10: 410-418. [Crossref]
- Salminen P, Karvonen J, Ovaska J (2010) Long-term outcomes after laparoscopic Nissen fundoplication for reflux laryngitis. Dig Surg 27: 509-514. [Crossref]
- Gregory D, Scotti DJ, Buck D, Triadafilopoulos G (2016) Budget Impact Analysis to Estimate the Cost Dynamics of Treating Refractory Gastroesophageal Reflux Disease With Radiofrequency Energy: a Payer Perspective. Manag Care 25: 42-50. [Crossref]
- Funk L, Zhang JY, Drosdeck JM, Melvin WS, Walker JP et al. (2015) Long-term cost-effectiveness of medical, endoscopic and surgical management of gastroesophageal reflux disease. Surgery 157: 126-136. [Crossref]
- Hanson DG, Kamel PL, Kahrilas PJ (1995) Outcomes of antireflux therapy for the treatment of chronic laryngitis. Ann Otol Rhinol Laryngol 104: 550-555. [Crossref]
