Opening Wedge Tibial Osteotomy in Medial Osteoarthritis of Varus Knee: Is it Necessary to Graft?
A B S T R A C T
Background: Opening wedge high tibial osteotomy (OWHTO) is accepted and commonly used procedure in selected patients with medial osteoathrosis in the varus knee. The aim of this study is to demonstrate that OWHTO can be performed without graft interposition to filling the osteotomy defect and we evaluate bone union, its complications (delayed or nonunion), and functional results.
Materials and Methods: This is a continuous retrospective study of patients treated by OWHTO from July 2008 to August 2018. OWHTO was performed using a 4 holes wedges-plate of Puddu without interposition of graft. HKA angle was assessed preoperatively and postoperatively and at 3 months. Clinical and radiological follow-up at 6 weeks, 3 months and 6 months assessed consolidation in terms of filing the defect of the osteotomy according to the method recommended by Brosset.
Results: Mean age was 53.2 years. Mean body mass index was 24, 8 and 30% of patients had BMI >30. The average varus was 171° (165°-177°); postoperatively, the HKA angle was 182° (176°-186°). Radiological union occurred on average after 3.5 months, with a minimum of 2 months and a maximum of 5. The time to union was 3.7 months for opening wedges of more than 10° and 3.4 months for opening wedges of 10° or less. 9 patients showed delayed union; in all these cases the lateral cortex was broken initially (stage II Takeuchi) with large correction>10°, 4 of them had BMI>30.
The IKS knee score increased from 69 to 90 and the functional score increased 84 to 95 with 95% of patients scoring between 92 and 97.
Conclusion: OWHTO without graft interposition using a wedges plate can be considered an alternative in the treatment of medial osteoarthritis of the varus knee, enabling the correction of the deformity and improvement of the clinical picture. Precautions must be taken event of large correction>10° and unstable lateral cortex fracture (stage II Takeuchi).
Keywords
Opening wedge high tibial osteotomy, wedges plate, graft interposition, bone union
Introduction
Opening wedge high tibial osteotomy (OWHTO) is accepted and commonly used as conservative surgical treatment for medial unicompartmental osteoathrosis of the knee. Indications are well defined and efficiency has been demonstrated in the short-, medium- and long term [1-13]. Many materials are available to fill the osteotomy defect (bone substitute, allograft or autograft, acrylic cement, ceramic spacer) but each has its disadvantages: foreign body reaction, degree of resorption, degree of re-population, and donor site complications for the autograft [14-18]. With The advent of new implant that can provide stable fixation, some authors have begun to achieve opening wedge high tibial osteotomy without filling the defect, letting the replacement of the lost bone material naturally while a stiff plate with wedges protects osteotomy [19-21]. In this retrospective study, we demonstrate that OWHTO can be performed without materiel interposition to fill the defect and we evaluate bone union, its complications (delayed union, nonunion) and functional results with this method.
Materials and Methods
This is a continuous retrospective study of patients admitted in our department from July 2008 to August 2018. We adopted the following inclusion criteria: medial compartment osteoarthritis with genu varum deformity (HKA angle less than 180°) with functional limitations in terms of pain and walking distance; absence of advanced patellofemoral osteoarthritis, intact lateral compartment, the absence of laxity and the same surgical technique with proximal tibia medial opening wedge osteotomy using plates with wedges. The osteotomy defect was unfilled.
Surgical Technique
The procedure was performed with a tourniquet at the root of the limb. A 5 cm longitudinal incision was performed between the anterior tibial tuberosity and the posteromedial border of tibia beginning 1cm from the joint line. The medial collateral ligament was removed from the tibial cortex with a bone rasp and then a Hohmann retractor was inserted. Under fluoroscopic control, A Kirschner wire is introduced upward from medial to lateral up to the tibiofibular joint. This is obliquely oriented starting approximately 4 cm below the medial joint line and directed across the superior aspect of the tibial tubercle to a point 1 cm below the lateral joint line. This step is repeated as necessary until guide pin placement is optimal. A second pin was placed more horizontally. The tip of the fibular head is a helpful reference when aiming the guide pin.
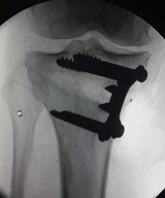
The osteotomy was performed with an oscillating saw along the K-wire guide. Stop 1 cm short of the lateral cortex. Continuous or frequent imaging helps prevent violation of the lateral cortex and/or misdirection of the osteotome (Figure 1). Once the tibial cut was finished, the osteotomy was completed with a first osteotome. Then, this cut bone was distracted using a second and a third osteotome. The last osteotome was introduced between the two osteotomes and slowly advanced until the osteotomy has been opened to provide the appropriate alignment. Distraction was maintained with a distractor of Meary according to the preoperative planification. The objective is to obtain 3° to 6° of valgus.
Figure 1: Postoperative radiological control after OWHTO using the alpha plate with wedges without materiel interposition.
With the leg held in extension, internal fixation was performed using a 4 holes Puddu plate with wedges corresponding to desired correction. Proximally the plate was fixed with two 6.5 mm cancellous screws parallel to the osteotomy line. Distally, the plate is secured with two 4.5 mm cortical screws. The immobilization was kept for 4 weeks, but patients were encouraged to do passive exercises starting immediately. Partial weight bearing started at 4 weeks and total weight-bearing at the 8-weeks and depending on the bone union. All patients were monitored radiologically after surgery at 3month, 6 month and one year (Figure 2).
Figure 2: Radiological index to measure filling of the osteotomy according to the method of Brosset with five identified zones.
Results
69 patients were included in this study, 48 women and 21 men, with an average age of 53.2 year (range 22-64). The average Body mass index was 24.8. 30 % of patients were overweight or obese in both genders. Bone union was assessed on A/P and lateral radiographs. A radiological index to measure filling of the osteotomy was used according to the method recommended by Brosset (Figure 2) [21]. We draw a triangle on A/P radiographs, with the sides of the triangle being along the borders and corner of the osteotomy. This triangular surface was then divided into five zones of the same surface area on the pre and postoperative radiographs. These areas were numbered 1 to 5, starting from the lateral cortex. Each area corresponded to 20% of the osteotomy being filled. The amount of filling (disappearance then increase in density of the osteotomy) and its progression were assessed at each radiological session. The osteotomy was considered as being stable if the site was 40 to 60% filled (area 3) and if the patient no longer had pain over the tibial osteotomy site while weight-bearing on the operated leg.
Preoperatively, the average varus was 171° (165°-177°); postoperatively the HKA angle was 182° (176°-186°). The tibial slope significantly changes: 9° before the surgery and 11.4° after the surgery. However, the patella was slightly lower: the Caton-Deschamps index went from 0.84 before the surgery to 0.79 on average at the last follow-up (Table 1).
Table 1: Radiological preoperative and postoperative assessment.
|
|
Preoperative |
Postoperative |
|
HKA angle |
171° (165°-177°) |
182° (176°-186°) |
|
Tibial slope |
9° |
11.4° |
|
Caton-Deschamps index |
0.84 |
0.79 |
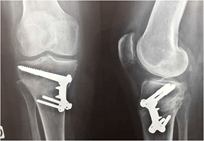
Functional evaluation was made by using the IKS scoring system. From the preoperative assessment to follow-up, the IKS knee score increased from 69 (25 to 96) to 90 (66 to 98) and the functional score increased 84 (50 to 100) to 95 (50 to 100) with 95% of patients scoring between 92 and 97. The average overall IKS score went from 154 (104 to 196) to 185 (144 to 198). Table 2 shows the clinical results before and after surgery. Radiological union occurred on average after 3.5 months, with a minimum of 2 months and a maximum of 5. The time to union was 3.7 months for opening wedges of more than 10° and 3.4 months for opening wedges of 10° or less (Figure 3).
Table 2: Clinical results before and after surgery.
|
|
Preoperative |
Postoperative |
|
IKS knee score |
69 (25 to 96) |
90 (66 to 98) |
|
Functional score |
84 (50 to 100) |
95 (50 to 100) |
|
Overall IKS score |
154 (104 to 196) |
185 (144 to 198) |
Figure 3: Progression of union at 2 months after OWHTO without filing the defect.
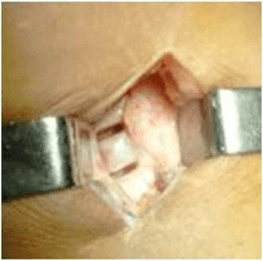
Full weight-bearing without assistance was possible after 3 months on average. 95% Patients were fully weight-bearing after 2 months. No loss in the knee range of motion was detected in any of the patients, in comparison with the preoperative period. As complication, we had 8 cases of intraoperative lateral cortical hinge fractures, 5 with stage I according to Takeuchi classification and 3 patients with stage II [22]. Delayed union problems were encountered in 5 patients. All patients with delayed union had more than 10° correction with BMI> 30 and 3 of them had lateral cortical hinge fractures stage II. At the last follow up, we don’t have any loss of correction. The (Figure 4) shows the macroscopical aspect of the regeneration after plate removal.
Figure 4: Macroscopical aspect of the regenerate after plate removal.
Discussion
When planned correction is > 10° some authors recommend grafting the osteotomy site to avoid loss of correction, delayed or nonunion. Brosset performed 51 OWTHO without grafting in 57% of which opening was>10° and reported no influence on degree of correction on consolidation [21]. Factors of delayed or no union have not been studied in the recent literature for OWTHO without graft interposition. Our retrospective study demonstrated that an opening wedge high tibial osteotomy can be performed without graft interposition using 4 holes Puddu plate with wedges and that our outcomes are similar to the recent literature data in terms of functional results. The majority of our patients were satisfied or very satisfied with the procedure. This method provides a precise correction of the alignment and maintenance of the correction over time. We confirm that the defect can be completely filled with this procedure without grafting.
Bone union occurred in all patients in an average time of 3.5 months. Our technique, without filing the osteotomy defect and without introducing an additional foreign body allows for union and filling of 4/5 of the osteotomy site in 97% of cases before the end of the first year, similar to results reported by Brosset [21]. This period of bone union is perhaps not so important in comparison with the results obtained in other series using various materiel interposition. The absence of material interposition eliminates some specific disadvantages. The use of an autologous graft bone is associated with earlier expense of iliac crest, morbidity such as severe pain after surgery in the donor site, lesion of the femoral cutaneous nerve if the incision is too low, bruises. The use of bone substitutes, acrylic cement, ceramic spacer also represents various drawbacks with their delayed union, degree of resorption and re-population, foreign body reaction and their high cost. In (Table 3), we demonstrate the period of union in other study using different materiel of interposition after OWHTO.
Table 3: Period of union with different materiel of interposition.
|
Author |
Materiel of interposition |
Period of union |
|
Goutallier [14] |
Cement spacer |
>3 months |
|
Dehoux [15] |
tricalcium phosphate substitute |
3 months |
|
Bonnevialle [16] |
Tricalcium phosphate macro-porous substitute |
> 3 months |
|
Koshino [17] |
Porous hydroxyapatite non resorbable ceramic substance |
4 months with continuous network of bone |
|
Bove [18] |
porous inert alumina ceramic spacer |
3 months with radiolucent margin around spacer |
The assessment of the consolidation is essentially made by a radiographic viewpoint without special method analysis of the consolidation of the osteotomy and no correlation with the clinic. The two-dimensional analysis of a three-dimensional phenomenon is always delicate. The index of consolidation adopted by Brosset is used as a reference and can be adapted to each radiograph [21]. Its use is not facilitated by the osseous superposition. This is directly related to the geometry of tibia that is roughly triangular and inclined relative to the x-ray osteotomy. The interpretation of the progression of bone callus finds weakened.
Indeed, at the end of the consolidation process, we get the formation of a true medial cortex. This neo-cortical has physical fastness properties which should be close to the cortical native. When osteotomy is filled with another materiel, the bone around consolidates the hold without recreating cortical and no real mechanical stability. In our series, radiological union occurred on average after 3.5 months, with a minimum of 2 months and a maximum of 5. There is no significant difference between the time to union for opening wedges of more than 10° (3.7 months) and opening wedges of 10° or less (3.4 months). El-Assal et al. find in their study an average time of union at 3.1 months, and they support OWHTO up to 14 mm without bone graft or bone substitutes, which shortens the operative time and avoids unnecessary morbidity [19].
In a comparative study Zorzi et al. concluded that time to bone union was not statically (p= 0.13) different between the group with bone graft (3.1 months) and the group without graft (3.4 months); and demonstrate that the use of autologous bone graft in OWHTO using plate with spacer less than 12.5 mm is unnecessary [20]. In our work we were able to obtain bone union more than 16 mm without filing the defect. In the literature the relation between elevated BMI and consolidation are discordant. Van houten found no relation, which is the opposite for Meidinger [23, 24]. In our series due to the low rate of delayed union this did not emerge as a risk factor.
Concerning lateral cortex fracture (LCF), Takeuchi et al. proposed a classification for lateral hinge fracture: unstable lateral hinge fracture (Type II) correlated with correction loss and delayed consolidation by rotational destabilization that the plate might fail to control [22]. Saragaglia reported 100% consolidation despite 5 cases of LCF [25]. In our series we found 8 cases of intraoperative lateral cortical fractures, 5 cases were stage I and 3 cases stage II without nonunion. Delayed union problems were encountered only in 5 patients. All patients had a large correction of more than 10° with elevated BMI and only 3 of them had lateral cortical hinge fractures stage II. As Takeuchi et al., we advised against authorizing full weight-bearing in case of lateral tibial cortex fracture until a callus has formed in the osteotomy [22].
However, SIBONI found that lateral cortex fracture was associated with delayed consolidation and non-union [26]. In this study, the authors concluded that Obesity and initial lateral cortex fracture appeared as risk factors for non-consolidation of OWHTO with large correction. Systematic bone or bone-substitute grafting may therefore be considered in this population in case of >10° correction. Biomechanically, the implantation of a stable fixation should help to avoid complications as loss of correction, delayed or nonunion. The internal fixation should guarantee a high primary stability and a maximal stiffness. Spahn found that conventional plates without wedges have lower stability [27]. By using a spacer or wedges, the primary stiffness is significantly increased. The wedges alone do not prevent the lateral cortex fracture, but the stable angle design can prevent this. The mechanical characteristics of the plate, with two components and millimeter- precision adjustment, enable the deformity to be corrected with greater precision. This plate has two parallel wedges, one proximal and the other distal, with a beveled surface which comes into contact with the bone. We believe that due to its greater wedge surface, it provides better support for the opening of the osteotomy, while the beveled surface of the wedges causes them to adhere more firmly to the bone.
The results described in our study that the use of the plate with wedges reproduces the satisfactory results reported in the literature with the use of similar plates with wedges, in terms of the correction of the deformity with a correct mechanical axis between 3 and 6° valgus. In terms of functional results, the majority of our patients were satisfied or very satisfied with this procedure. The scores knee and function contained in the global score of the IKS (International Knee Society) are clearly increased. We did not find statistical relation between the obtained scores and the level of satisfaction of the patients. The comparison of these results with the data of the literature is delicate. Indeed, the scores used in each of the studies about OWHTO are different. Nevertheless, some criteria can be compared as the pains, the perimeter of walking, and the resumption of the activities. On the other hand, in the revision, the average IKS knee was 90 and IKS knee function was 95. For knees having undergone a morphological modification of their slope and their patellar height we were not able to find a relation between these modifications and the functional results.
Conclusion
OWHTO without graft interposition using a 4 holes Puddu plate with wedges can be considered an alternative in the treatment of medial osteoarthrosis of the varus knee, enabling the correction of the deformity and improvement of the clinical picture. Precautions must be taken event of large correction>10° and unstable lateral cortex fracture (stage II Takeuchi). More studies with this procedure are necessary, after these encouraging results to finding risk factors of delayed or nonunion.
Competing Interests
None.
Author Contributions
All authors designed the study, accumulated data, analysed data, drafted manuscript. All authors read and approved the final manuscript.
Article Info
Article Type
Research ArticlePublication history
Received: Sat 06, Mar 2021Accepted: Fri 19, Mar 2021
Published: Fri 02, Apr 2021
Copyright
© 2023 El Ibrahimi Abdelhalim. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited. Hosting by Science Repository.DOI: 10.31487/j.SCR.2021.04.02
Author Info
El Ibrahimi Abdelhalim Hatim Abid Mohammed El Idrissi Abdelmajid Elmrini
Corresponding Author
El Ibrahimi AbdelhalimDepartment of Orthopedic Surgery B4, UH Hassan II of Fez, Morocco
Figures & Tables
Table 1: Radiological preoperative and postoperative assessment.
|
|
Preoperative |
Postoperative |
|
HKA angle |
171° (165°-177°) |
182° (176°-186°) |
|
Tibial slope |
9° |
11.4° |
|
Caton-Deschamps index |
0.84 |
0.79 |
Table 2: Clinical results before and after surgery.
|
|
Preoperative |
Postoperative |
|
IKS knee score |
69 (25 to 96) |
90 (66 to 98) |
|
Functional score |
84 (50 to 100) |
95 (50 to 100) |
|
Overall IKS score |
154 (104 to 196) |
185 (144 to 198) |
Table 3: Period of union with different materiel of interposition.
|
Author |
Materiel of interposition |
Period of union |
|
Goutallier [14] |
Cement spacer |
>3 months |
|
Dehoux [15] |
tricalcium phosphate substitute |
3 months |
|
Bonnevialle [16] |
Tricalcium phosphate macro-porous substitute |
> 3 months |
|
Koshino [17] |
Porous hydroxyapatite non resorbable ceramic substance |
4 months with continuous network of bone |
|
Bove [18] |
porous inert alumina ceramic spacer |
3 months with radiolucent margin around spacer |

References
1. Klinger HM, Lorenz F, Harer T (2001) Open wedge tibial osteotomy by hemicallotasis for medial compartment osteoarthritis. Arch Orthop Trauma Surg 121: 245-247. [Crossref]
2. Franco V, Cerullo G, Cipolla M, Gianni E, Puddu G (2002) Open wedge high tibial osteotomy. Tech Knee Surg 1: 43-53.
3. Hernigou P, Medevielle D, Debeyre J, Goutallier D (1987) Proximal tibial osteotomy for osteoarthritis with varus deformity. A ten to thirteen-year follow-up study. J Bone Joint Surg Am 69: 332-354. [Crossref]
4. Lobenhoffer P, Agneskirchner JD (2003) Improvements in surgical technique of valgus high tibial osteotomy. Knee Surg Sports Traumatol Arthrosc 11: 132-138. [Crossref]
5. Nakhostine M, Friedrich NF, Muller W, Kentsch A (1993) A special high tibial osteotomy technique for treatment of unicompartmental osteoarthritis of the knee. Orthopedics 16: 1255-1258. [Crossref]
6. Paccola CA, Fogagnolo F (2005) Open-wedge high tibial osteotomy: a technical trick to avoid loss of reduction of the opposite cortex. Knee Surg Sports Traumatol Arthrosc 13: 19-22. [Crossref]
7. Weale AE, Lee AS, MacEachern AG (2001) High tibial osteotomy using a dynamic axial external fixator. Clin Orthop Relat Res 382: 154-167. [Crossref]
8. Sangwan SS, Siwach RC, Singh Z, Duhan S (2000) Unicompartmental osteoarthritis of the knee: an innovative osteotomy. Int Orthop 24: 148-150. [Crossref]
9. Magyar G, Ahl TL, Vibe P, Toksvig Larsen S, Lindstrand A (1999) Open-wedge osteotomy by hemicallotasis or the closedwedge technique for osteoarthritis of the knee. A randomised study of 50 operations. J Bone Joint Surg 81: 444-448. [Crossref]
10. Miller BS, Sterett WI (2003) High tibial osteotomy utilizing distraction osteogenesis. Tech Knee Surg 2: 184-189.
11. Murphy SB (1994) Tibial osteotomy for genu varum. Indications, preoperative planning, and technique. Orthop Clin North Am 25: 477-482. [Crossref]
12. Naudie D, Bourne RB, Rorabeck CH, Bourne TJ (1999) The Install Award. Survivorship of the high tibial valgus osteotomy. A 10- to -22-year followup study. Clin Orthop Relat Res 367: 18-27. [Crossref]
13. Hernigou P (1996) A 20-year follow-up study of internal gonarthrosis after tibial valgus osteotomy. Single versus repeated osteotomy. Rev Chir Orthop 82: 241-250. [Crossref]
14. Goutallier D, Julieron A, Hernigou P (1992) Cement wedge replacing iliac graft in tibial wedge osteotomy. Rev Chir Orthop Reparatrice Appar Mot 78: 138-144. [Crossref]
15. Dehoux E, Madi K, Fourati E, Mensa C, Segal P (2005) High tibial open-wedge osteotomy using a tricalcium phosphate substitute: 70 cases with 18 months mean follow-up. Rev Chir Orthop Reparatrice Appar Mot 91: 143-148. [Crossref]
16. Bonnevialle P, Abid A, Mansat P, Verhaeghe L, Clement D et al. (2002) Tibial valgus osteotomy using a tricalcium phosphate medial wedge: a minimally invasive technique. Rev Chir Orthop 88: 486-492. [Crossref]
17. Koshino T, Murase T Saito T (2003) Medial opening wedge high tibia osteotomy with use of porous hydroxyapatite to treat medial compartment osteoarthritis of the knee. J Bone Joint Surg 85: 78-85. [Crossref]
18. Bove JC (2002) Utilization of a porous alumina ceramic spacer in tibial valgus open-wedge osteotomy: 50 cases at 16 months mean follow-up. Rev Chir Orthop 88: 480-485. [Crossref]
19. El Assal MA, Khalifa YE, Abdel Hamid MM, Said HG, Bakr HM (2010) Opening-wedge high tibial osteotomy without bone graft. Knee Surg Sports Traumatol Arthrosc 18: 961-966. [Crossref]
20. Zorzi AR, da Silva HG, Muszkat C, Marques LC, Cliquet A Jr et al. (2011) Opening-wedge high tibial osteotomy with and without bone graft. Artif Organs 35: 301-307. [Crossref]
21. Brosset T, Pasquier G, Migaud H, Gougeon F (2011) Opening wedge high tibial osteotomy performed without filling the defect but with locking plate fixation (TomoFixTM) and early weight-bearing: Prospective evaluation of bone union, precision and maintenance of correction in 51 cases Gougeond. Orthopaed Traumatol Surg Res 97: 705-711. [Crossref]
22. Takeuchi R, Ishikawa H, Kumagai K, Yamaguchi Y, Chiba N (2012) Fractures around the lateral cortical hinge after a medial opening-wedge high tibial osteotomy: a new classification of lateral hinge fracture. Arthroscopy 28: 85-94. [Crossref]
23. Van Houten AH, Heesterbeek PJ, van Heerwaarden RJ, van Tienen TG, Wymenga AB (2014) Medial open wedge high tibial osteotomy: can delayed or nonunion be predicted? Clin Orthop Relat Res 472: 1217-1224. [Crossref]
24. Meidinger G, Imhoff AB, Paul J, Kirchhoff C, Sauerschnig M et al. (2011) May smokers and overweight patients be treated with a medial openwedge HTO? Risk factors for non-union. Knee Surg Sports Traumatol Arthrosc 19: 333-339. [Crossref]
25. Saragaglia D, Blaysat M, Inman D, Mercier N (2011) Outcome of opening wedge high tibial osteotomy augmented with a Biosorb® wedge and fixed with a plate and screws in 124 patients with a mean of ten years follow-up. Int Orthop 35: 1151-1156. [Crossref]
26. Siboni R, Beaufils P, Boisrenoult P, Steltzlen C, Pujol N (2018) Opening-wedge high tibial osteotomy without bone grafting in severe varus osteoarthritic knee. Rate and risk factors of non-union in 41 cases. Orthop Traumatol Surg Res 104: 473-476. [Crossref]
27. Spahn G, Mückley T, Kahl E, Hofmann GO (2006) Biomechanical investigation of different internal fixations in medial opening-wedge high tibial osteotomy. Clin Biomech 21: 272-278. [Crossref]
