How to Confirm and Document Adequate Lumbar Spine Discectomy Intraoperatively?
A B S T R A C T
Lumbar discectomy is a common procedure for acute disc prolapse, especially in patients with neurological deficit [1]. The literature describes using fluoroscopy intraoperatively to avoid wrong level and side [2]. However, there is no method to confirm/document adequate discectomy apart from a postoperative MRI. The authors' technique involves taking clinical photos of the removed disc material. This technique provides accurate, low-cost documentation, and the patient can review it post-operatively. This could be of significant value in large disc prolapse and cauda equina syndrome surgery.
Keywords
Lumbar discectomy, cauda equina, recurrent disc, residual disc, diagnosis
Background
Posterior lumbar discectomy is a common procedure for acute disc prolapse, especially in patients with neurological deficit. The recurrence rate varies 5-18% [3]. This could be due to inadequate removal of disc material with residual disc or wrong level/side. On the other hand, it could be a true recurrence [4]. From 2002 to 2010, wrong level surgery and CES surgical failures constituted 9.9% each, of spinal surgery NHS Litigations with a cost of 12,000,000 GBP [5].
Aim
This study describes the authors’ technique to confirm and document adequate correct level discectomy.
Technique
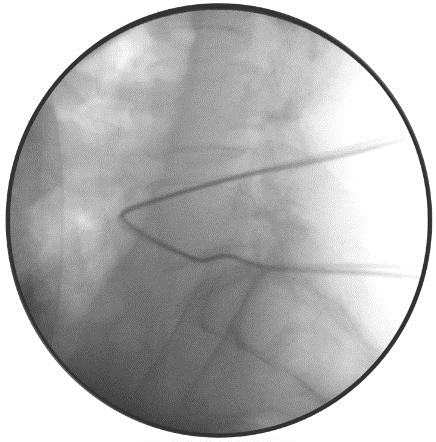
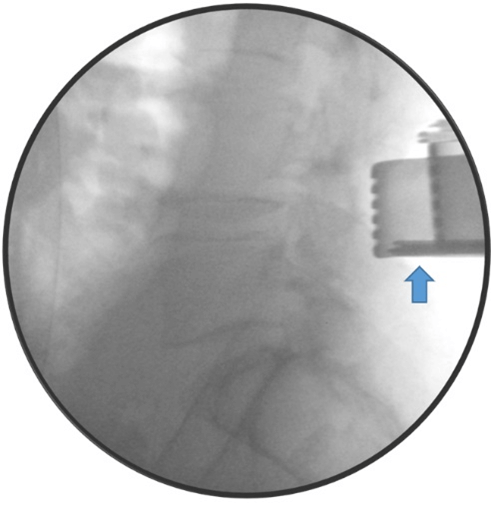
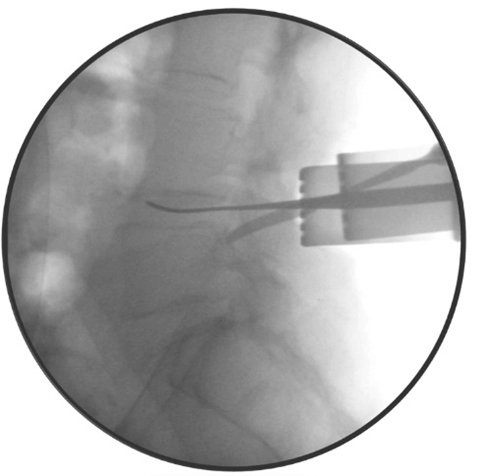
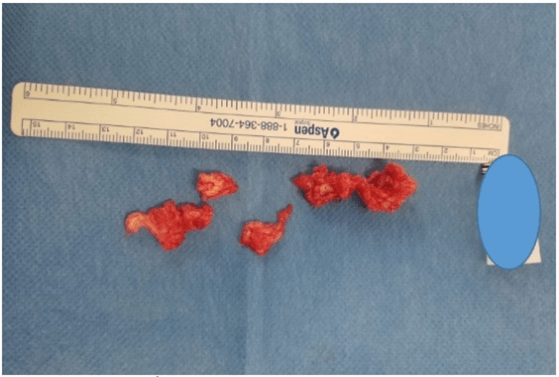
Pre-incision fluoroscopy was undertaken to confirm the level and side (Figure 1). Further fluoroscopy was undertaken before breaching ligamentum flavum (Figure 2). Central decompression/micro-discectomy was performed according to surgeon’s preference and the size of the disc. Once discectomy was completed, probes are placed in the disc space and nerve foreman to fluoroscopically document the extent of decompression (Figure 3). The removed disc fragments were collected and kept aside. Following surgery, a photo of the disc material (with scale and patient’s label) was taken and included in the patient records (Figure 4).
Figure 1: Identification of the correct level (L4/5) before prepping and draping.
Figure 2: Confirmation of correct level and side at ligamentum flavum level.
Figure 3: Watson Cheyne in the correct disc level (L4/5) and probe in the foramen (L5 exiting root) under the image screen.
Figure 4: Photo of herniated disc materials with scale and patient label to be added in the patient notes.
Discussion
The use of intraoperative fluoroscopy to confirm the correct level and side in lumbar discectomy is recommended by the British association of spine surgery (BASS). This technique is useful for the first point avoiding residual disc (wrong level) [2]. Nevertheless, adequate discectomy cannot be confirmed apart from postoperative MRI. Hence, the use of photos showing the excised disc fragments’ volume could form a robust low-cost documentation of adequate surgery. This could be undertaken in all discectomy surgeries without any extra cost or patient inconvenience. This provides substantial medicolegal evidence of adequate discectomy especially in CES surgery.
Conclusion
Authors recommend using intraoperative photos of the excised disc material to be taken in all lumbar discectomy surgeries.
Conflicts of Interest
None.
Funding
None.
Article Info
Article Type
Case ReportPublication history
Received: Wed 18, Nov 2020Accepted: Thu 10, Dec 2020
Published: Tue 22, Dec 2020
Copyright
© 2023 Joseph Gamal Boktor. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited. Hosting by Science Repository.DOI: 10.31487/j.SCR.2020.12.20
Author Info
Joseph Gamal Boktor Miriam Nakanda Kakaire Ashish Khurana Devi Prakash Tokala
Corresponding Author
Joseph Gamal BoktorST3 Trauma and Orthopaedics, Royal Gwent Hospital, Newport, Wales, United Kingdom
Figures & Tables
References
- Peul WC, van Houwelingen HC, van den Hout WB, Brand R, Eekhof JAH et al. (2007) Surgery versus prolonged conservative treatment for sciatica. N Engl J Med 356: 2245-2256. [Crossref]
- Irace C, Corona C (2010) How to Avoid Wrong-Level and Wrong-Side Errors in Lumbar Microdiscectomy. J Neurosurg Spine 12: 660-665. [Crossref]
- Hlubek RJ, Mundis GM (2017) Treatment for Recurrent Lumbar Disc Herniation. Curr Rev Musculoskelet Med 10: 517-520. [Crossref]
- Lurie JD, Moses RA, Tosteson AN, Tosteson TD, Carragee EJ et al. (2013) Magnetic Resonance Imaging Predictors of Surgical Outcome in Patients with Lumbar Intervertebral Disc Herniation. Spine 38: 1216-1225. [Crossref]
- Cross CE, Kapoor V, Todd B, Bhutta MA (2018) The Litigation Burden to The NHS From Spinal Injuries and Surgery: Analysis Of 236 Consecutive Closed Claims. Orthop Proc 94B.
