Descending Necrotizing Mediastinitis in Covid- 19 Time
Descending Necrotizing Mediastinitis in Covid- 19 Time
A B S T R A C T
Introduction: Descending Necrotizing Mediastinitis (DNM) is the fatal form of mediastinitis and mostly develops as a complication of peritonsillar abscesses or dental- odontogenic infections. The aim of this study is to evaluate clinical and surgical feature of the patients with DNM who were managed in our Department during the period of general lockdown in Greece, between March 2020 and June 2020, because of the Covid-19.
Patients and Methods: During the period of general lockdown in Greece, 4 patients, mean age 46, 25 years (range 39-59), with DNM treated to our Department of General Thoracic Surgery. Primary odontogenic abscess occurred to 2 patients and peritonsillar abscess to other 2 of them. Diagnosis was confirmed by computed tomography (CT) of the neck and chest. All patients underwent surgical drainage of abscesses of the involved cervical region and mediastinum by lateral cervicotomy and left thoracotomy in three of them and cervicotomy, and bilateral thoracotomy in one patient.
Results: The delay between the occurrence of thoracic symptoms and mediastinal drainage varied from 1 to 3 days. The side of the thoracotomy depended on the involved mediastinal compartments and side of pleural effusion. The duration of mediastinal drainage varied from 12 to 20 days (mean: 17 days). One patient died of multiorgan failure related to post-op septic shock.
Conclusion: Between January 2000 and January 2020, 21 patients with DNM were treated at our Department, whilst during the four - month of lockdown, four patients were treated. We concluded that the patients delay for dentistry recourse because of covid-19, result in the increased number of patients with DNM in the above period. Delayed diagnosis and inadequate drainage are the main causes of the high mortality rate of DNM. If one realistically hopes to avoid the high mortality rate, aggressive surgical drainage and debridement of the neck and drainage of the mediastinum via a posterolateral thoracotomy by a multidisciplinary team of surgeons is a must.
Keywords
Descending necrotizing mediastinitis, mediastinitis, necrotizing fasciitis, Covid-19
Introduction
Descending Necrotizing Mediastinitis (DNM) is the fatal form of mediastinitis and usually develops as a complication of peritonsillar abscesses or dental - odontogenic infections. The delay in the treatment of a infection that starts in the pharynx, the tonsillar or tooth, leads to the spread of the suppurative infection through the deep and superficial cervical fascial planes to the mediastinum [1]. DNM was first described by Estrera et al. the beginning of 1980s.
They described the diagnostic criteria in the following four titles :1) Clinical manifestation of severe oropharyngeal infection; 2) Demonstration of characteristic roentgenographic features of mediastinitis; 3) Documentation of necrotizing mediastinal infection at operation or postmortem examination or both; and 4) Establishment of relationship between oropharyngeal infection and development of necrotizing mediastinal process [2]. Even with the use of CT scanning, aggressive drainage, and modern antibiotic treatment, the mortality rate of DNM remains high. Surgical management, and particularly the optimal form of mediastinal drainage, remains controversial with support ranging from cervical drainage alone, to cervical drainage and routine thoracotomy [3]. We report our experience with four patients affected by DNM, in the period of lockdown in Greece because of the pandemic of coronavirus and stress the importance of early and large surgical mediastinal drainage.
Patients and Methods
During the lockdown period between 3/2020-6/2020, because of Covid-19, four patients with DNM treated at the Department of General Thoracic Surgery at the General Hospital of Attica KAT, Athens, Greece. In all cases, the diagnostic criteria of DNM as defined by Estrera et al. were fulfilled. The patients included 3 men and 1 woman, with ages ranging from 39 to 59 years (mean: 46, 25 years). First, two of these patients were hospitalized at Oral and Maxillofacial Surgical Department of our Hospital and the other two patients were referred to our Department from other hospitals of Athens. All the patients because of lockdown and the fear of Covid-19, delayed receiving dental therapy. The primary oropharyngeal infection was a peritonsillar abscess in 2 patients and an odontogenic abscess in the other 2 patients. One of the patients was alcoholic, three were referred as long-term smokers, one was affected by diabetes and two were affected by psychotic disturbances.
Symptoms at admission included cervical pain (n=4, 100%), odynophagia (n=2 , 50%), cervical swelling (n=3, 75%), hoarseness (n=2, 50%), and dyspnea ( n= 2, 50% ). Stridor, swelling of the face and thoracic pain, were reported in one patient. The main clinical findings were fever and swelling/ redness of the pharynx / larynx in all patients. Diagnosis was made by preoperative cervicothoracic computed tomography - (CT) scan in all patients. Follow-up CT scan was performed to assess the adequacy of therapy. All patients had radiological signs of posterior mediastinal involvement and 3 of them pleural effusion (monolateral in two and bilateral in one case). Empirical, broad spectrum, intravenous antibiotics were initiated as soon as diagnosis was suspected. The surgical management was as follows.
First, all patients were treated by cervical drainage. Prior of this, the odontogenic and peritonsillar abscesses were drained by an oral and maxillofacial surgeon - 2 in our hospital and 2 in the referred hospitals. The neck is usually approached through an incision anterior to the sternocleidomastoid muscle. The involved cervical spaces were opened, drained, and debrided of necrotic tissue and the cervical wound was left open. Thoracic procedure included radical surgical debridement of the mediastinum and pleura through a posterolateral thoracotomy with complete excision of tissue necrosis, decortication, and placement of chest tubes for adequate mediastino-pleural drainage. The duration of drainage was dependent on clinical progress, return to normal CT scanning aspects, and results of the cultures of fluids aspirated from the mediastinal tubes.
Results
Bacteriologic results from materials obtained from the neck, pleura, and blood revealed in all cases a polymicrobial infection with mixed aerobic and anaerobic organisms. The most common isolated aerobic bacteria were Streptococcus species including pyogenes (n=1), epidermis (n=2), milleri (n=1). In two patients anaerobic bacteria (Prevotella melaninogenica, Peptostreptococcus anaerobius) were present. In one patient Acinetobacter baumani and Staphylococcus epidermidis were isolated in blood cultures whereas Klebsiella pneumoniae, Candida and Acinetobacter baumani were isolated in bronchial secretions in two patients. The delay between the occurrence of thoracic symptoms and mediastinal drainage varied from 1 to 3 days. Chest radiography showed a widening of the mediastinal shadow (3 patients), pneumomediastinum (1 patient), and pleural effusion (3 patients).
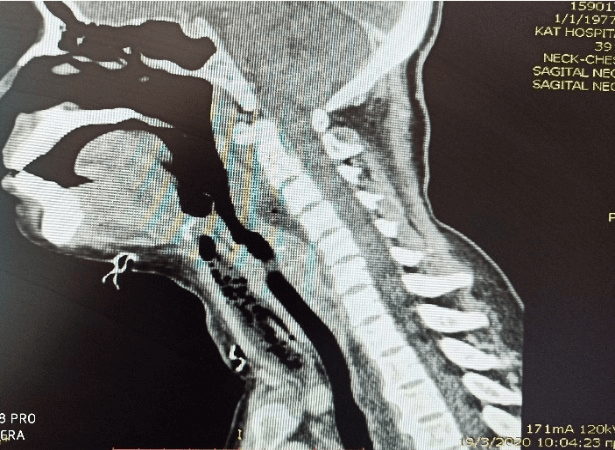
Figure 1: CT - Scan of the neck with prevertebral abscess.
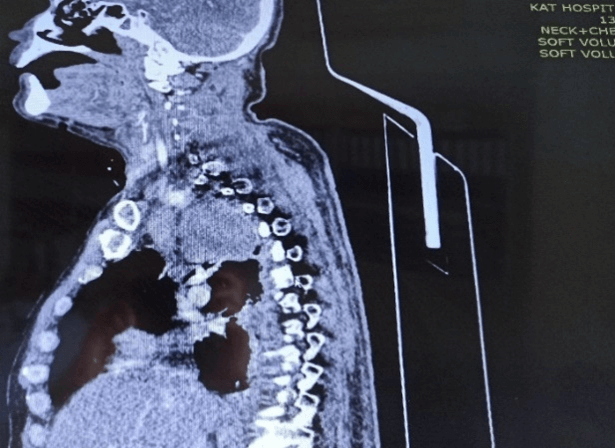
Figure 2: Cervical abscess and cervical cellulitis with emphysema associated with diffuse mediastinitis and mediastinal collections.
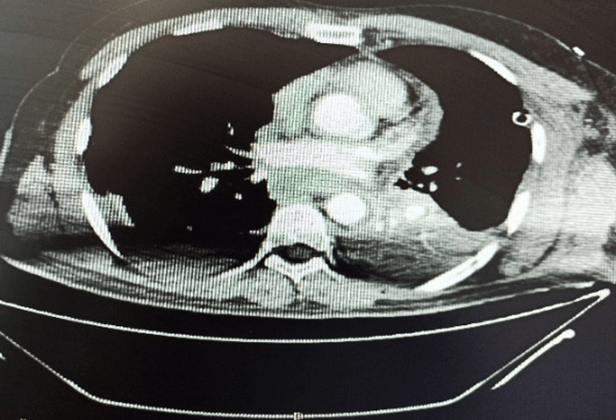
Figure 3: Thoracic empyema.
Each patient was promptly submitted to CT scan of the neck (Figure 1) and thorax which confirmed the diagnosis of Descending Necrotizing Mediastinitis, displaying cervical abscess or cervical cellulitis with emphysema associated with diffuse mediastinitis or mediastinal collections and complicated by empyema (3 patients) (Figures 2 & 3). The side of thoracotomy depended on the involved mediastinal compartments and side of pleural effusion on CT scan. Operative findings and surgical procedure are reported in (Table 1). Tracheostomy was indicated in all patients. The duration of mediastinal drainage varied from 12 to 20 days (mean: 17 days).
Table 1: Summary of 4 patients with Descending Necrotizing Mediastinitis.
|
Case |
Age (years) |
Male |
Initial site of infection |
Diffusion of infection |
Surgical Drainage |
Hospital stay (days) |
Outcome |
|
1 |
47 |
F |
Peritonsillar abscess |
Monolateral cervical abscess, posterior mediastinitis, |
Monolateral cervicitomy, Right thoracotomy, |
15 |
Died |
|
2 |
39 |
M |
Peritonsillar abscess |
Monolateral cervical abscess, posterior mediastinitis, Left empyema |
Monolateral cervicotomy, Left thoracotomy |
26 |
Discharge |
|
3 |
40 |
M |
Odontogenic abscess |
Cervical abscess on both sides, posterior mediastinitis, Pleural effusion on both sides. |
Cervicotomy- Thoracotomy on both sides |
35 |
Discharge |
|
4 |
59 |
M |
Odontogenic abscess |
Monolateral cervical abscess, posterior mediastinitis, Left empyema |
Monolateral cervicitomy, Left thoracotomy |
28 |
Discharge |
The outcome was favorable in 3 patients. All the patients had mediastinal drainage through a thoracotomy. One patient - a man of 40-year-old - out of four, was needed two re-operations. The female patient experienced early postoperative onset of septic shock and died because of multiorgan failure 12 days after the operation in the I.C.U. Control thoracic CT scan done before discharge displayed normal aspect with return to water density of the mediastinal fat or persistence of increased soft tissue attenuation in the mediastinal fat planes, but without widening of the mediastinum. The mean hospital stay for patients was 29, 6 days (range: 26 - 35 days). No intraoperative mortality occurred.
Discussion
DNM diagnosis implies that the relationship between mediastinitis and oropharyngeal infection is clearly established. Infections originating in the fascial planes of the head and neck spread downward into the mediastinum along the cervical fascias, facilitated by the gravity, breathing, and negative intrathoracic pressure. Knowledge of the cervical fascial planes is essential in understanding the propagation pathways, symptoms and thoracic complications of cervical infections [4, 5]. It has been estimated that 8% of mediastinitis cases originating in the neck spread through the pretracheal space: greater than 70% of spread occurs through the retrovisceral and “danger space”. Delay of diagnosis is one of the primary reasons for the high mortality in DNM and this is the reason of high rate of DNM during the lockdown period.
Immunosuppression should come to mind in many DNM patients. The comorbidities most commonly associated with DNM are type II Diabetes Mellitus, inadequate nutrition, and poor hygiene, advanced age, chronic liver- renal failure and malignancy [6]. However, there are a certain number of DNM patients without any comorbidities. The clinicians should also be prepared for laryngeal oedema and airway obstruction due to the nature of the disease. Tracheostomy is also proposed for secretion cleaning and the prevention risk of aspiration. Adult Respiratory Distress Syndrome (ARDS) can be developed primarily when diagnosis is delayed [7].
CT scan immediately confirms the mediastinitis diagnosis with high accuracy. Contiguous 1 cm cervicothoracic scan demonstrated the continuity of the infectious process between the neck and thorax, establishing the relationship between neck infection and mediastinitis. Moreover, follow-up CT scanning postoperatively is also recommended, because the initial surgical drainage is not always sufficient, and a need for redrainage is not uncommon [8, 9]. Intravenous broad-spectrum antibiotic therapy alone in not efficient without adequate surgical drainage of the cervical and mediastinal collections, extensive debridement, excision of necrotic tissue, and wide mediastinal and pleural irrigation. Aggressive surgical drainage recommended as the preferred treatment of DNM.
All four patients underwent surgical procedures for drainage of the neck and posterolateral thoracotomy for drainage and debridement of the thorax and mediastinum after the diagnosis of DNM. These procedures were performed by a team of thoracic surgeon and an oral and maxillofacial surgeon because an odontogenic disease was encountered. We applied the posterolateral thoracotomy because provides the broadest exposure of the prevertebral and paraoesophageal planes without the risk of sternal osteomyelitis encountered with medial sternotomy or clamshell incision. Furthermore, posterolateral thoracotomy is generally tolerated even by acutely ill patients [10]. We surveyed our patients with CT scan of the neck and chest during the 3rd and 7th postoperative day. The CT scan signs allowed to identify incomplete drainage and progression of the septic spread in the mediastinum and prompted urgent reoperation. During the period of lockdown in Greece, because of the Covid-19, we noticed an increase of DNM at our Thoracic Department.
The increased rate of DNM these two months was due to the fear of the patients because of Covid-19 visiting a dentist for further treatment. As a result, the delay of diagnosis and treatment of the abscesses led to the lethal condition, called DNM. In summary, DNM remains a life-threatening infection. Delayed diagnosis and inadequate drainage are the main causes of the high mortality rate of DNM. Routine use of the CT scan is highly recommended in patients with a deep cervical infection for early detection of mediastinitis at a time when the chest roentgenogram is still normal. If one realistically hopes to avoid the high mortality rate, aggressive surgical drainage and debridement of the neck and drainage of the mediastinum via a posterolateral thoracotomy by a multidisciplinary team of surgeons is a must.
In conclusion, we will agree with Esteva [11]. “We learned from experience to be as aggressive as the disease is, even if the patient seems to be in good condition. Dental resection, wide open drainage of the oral and cervical process, and thoracotomy are needed in cases of DNM”.
Article Info
Article Type
Research ArticlePublication history
Received: Mon 28, Sep 2020Accepted: Fri 09, Oct 2020
Published: Wed 28, Oct 2020
Copyright
© 2023 Michos Thrasyvoulos. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited. Hosting by Science Repository.DOI: 10.31487/j.SCR.2020.10.10
Author Info
Michos Thrasyvoulos Stamatelopoulos Athanasios Roumpaki Anastasia Vakouftsi Alexia- Christina Chatziantoniou Christos Gakidis Ioannis Michos Petros
Corresponding Author
Michos ThrasyvoulosGeneral Thoracic Department, of General Hospital of Attica “KAT”, Athens, Greece
Figures & Tables
Table 1: Summary of 4 patients with Descending Necrotizing Mediastinitis.
|
Case |
Age (years) |
Male |
Initial site of infection |
Diffusion of infection |
Surgical Drainage |
Hospital stay (days) |
Outcome |
|
1 |
47 |
F |
Peritonsillar abscess |
Monolateral cervical abscess, posterior mediastinitis, |
Monolateral cervicitomy, Right thoracotomy, |
15 |
Died |
|
2 |
39 |
M |
Peritonsillar abscess |
Monolateral cervical abscess, posterior mediastinitis, Left empyema |
Monolateral cervicotomy, Left thoracotomy |
26 |
Discharge |
|
3 |
40 |
M |
Odontogenic abscess |
Cervical abscess on both sides, posterior mediastinitis, Pleural effusion on both sides. |
Cervicotomy- Thoracotomy on both sides |
35 |
Discharge |
|
4 |
59 |
M |
Odontogenic abscess |
Monolateral cervical abscess, posterior mediastinitis, Left empyema |
Monolateral cervicitomy, Left thoracotomy |
28 |
Discharge |
References
- Mihos P, Potaris K, Gakidis I, Papadakis D, Rallis G (2004) Management of Descending Necrotizing Mediastinitis. J Oral Maxillofac Surg 62: 966-972. [Crossref]
- Estrera AS, Landay MJ, Grisham JM, Sinn DP, Platt MR (1983) Descending necrotizing mediastinitis. Surg Gynecol Obstet 157: 545-552. [Crossref]
- Mihos PT, Gakidis I, Potaris K, Stathopoulou S (2006) Tonsillitis, descending necrotizing mediastinitis, and a different neck drainage. Am J Otolaryngol 27: 341-343. [Crossref]
- Levitt MGW (1970) Cervical fascias and deep neck infections. Laryngoscope 80: 409-435. [Crossref]
- Zachariades N, Mezitis M, Stavrinidis P, Konsolaki Agouridaki E (1988) Mediastinitis, Thoracic empyema, and Pericarditis as Complications of a Dental Abscess: Report of a Case. J Oral Maxillofac Surg 46: 493-495. [Crossref]
- Sumi Y (2015) Descending necrotizing mediastinitis: 5 years of published data in Japan. Acute Med Surg 2: 1-12. [Crossref]
- Sancho LM, Minamoto H, Fernandez A, Sennes LU, Jateme FB (1999) Descending necrotizing mediastinitis: A retrospective surgical experience. Eur J Cardiothoracic Surg 16: 200-205. [Crossref]
- Marty Ané CH, Berthet JP, Alric P, Pegis JD, Rouviére Ph et al. (1999) Management of Descending necrotizing mediastinitis: An aggressive treatment for an aggressive disease. Ann Thorac Surg 68: 212-217. [Crossref]
- Marty Ané CH, Alauzen M, Alric P, Cousine OS, Mary H (1994) Descending necrotizing mediastinitis: Advantage of mediastinal drainage with thoracotomy. J Thorac Cardiovasc Surg 107: 55-61. [Crossref]
- Brunelli A, Sabatini A, Catalini G, Fianchini A (1996) Descending necrotizing mediastinitis: Cervicotomy or thoracotomy? J Thorac Cardiovasc Surg 111: 485-486. [Crossref]
- Esteva H (1997) To the Editor: Descending Necrotizing Mediastinitis. Chest 111: 529. [Crossref]
