Critical Heart Rate Dependent LBBB: Need Caution!
A B S T R A C T
Right bundle branch block (RBBB) and left bundle branch block (LBBB) are commonly seen in geriatric cases posted for surgeries. LBBB usually results from conduction system degeneration or myocardial pathology. LBBB is often associated with hypertension, myocarditis, coronary heart disease, aortic valve disease, cardiomyopathy etc. We report a case of diagnosed LBBB preoperatively posted for emergency spinal decompression. After induction of anaesthesia, the heart rate settled below 77 beats per minute (bpm) and led to reversion of LBBB to normal sinus rhythm. LBBB is a red flag diagnosis to the anaesthesiologist. But the knowledge of critical heart rate is important; below which the rhythm may revert back to normal sinus rhythm. The knowledge to differentiate between myocardial ischaemia and LBBB is the need of the hour.
Keywords
Left bundle branch block, heart arrhythmias, peri operative arrhythmias
Purpose of Article
The purpose of this article is to expand the knowledge regarding intra operative Left bundle branch block and critical heart rate. A doctor should be able to distinguish between LBBB and more dangerous Myocardial infarction.
Introduction
Any cardiac abnormality in peri operative period is detrimental and raises a red flag to the anaesthesiologist. Peri operative rhythm disturbances, myocardial infarction are dreaded complications which are often faced by the medical team. Right bundle branch block (RBBB) and left bundle branch block (LBBB) are commonly seen in geriatric cases posted for surgeries. Geriatric population now undergoes various procedures everyday around the world. LBBB usually results from conduction system degeneration or myocardial pathology [1, 2]. New onset of arrhythmias can occur due to innumerable causes, but remission of LBBB under general anaesthesia is rarely documented. The anaesthesiologist is expected to distinguish between the more critical myocardial ischaemia (MI) intra-operatively from the LBBB.
We report a case of preoperative left bundle branch block that reverted to normal conduction after a decrease in heart rate during surgery under general anaesthesia and which resurged intermittently and was dependent on heart rate in the immediate postoperative period.
Case Presentation
A 62-year-old male patient diagnosed as cauda equina syndrome was posted for emergency spinal cord decompression. Pre-anaesthetic evaluation revealed a medical history of hypertension for 6 years (for which he was prescribed tab amlodipine 5 mg by the physician). Physical examination revealed acute onset of back pain associated with loss of bladder and bowel control for past 2 days. Laboratory investigations were within normal limits. Preoperative electrocardiograph (ECG) showed sinus rhythm with pattern compatible with LBBB. The patient didn’t give any history of chest pains, palpitations or decreased effort tolerance. Hemodynamically, patient was stable throughout the preoperative period. Urgent cardiac consultation was sought, and a preoperative 2 D Echocardiography was conducted which documented a paradoxical motion of septum, concentric left ventricular hypertrophy (LVH), diastolic dysfunction and a mildly reduced left ventricular systolic function with ejection fraction of 45-50%. Cardiac markers were sent which were negative. Due to the urgent nature of the surgery and the hemodynamic stability, it was decided not to postpone the surgical procedure for further study of electrocardiographic alterations.
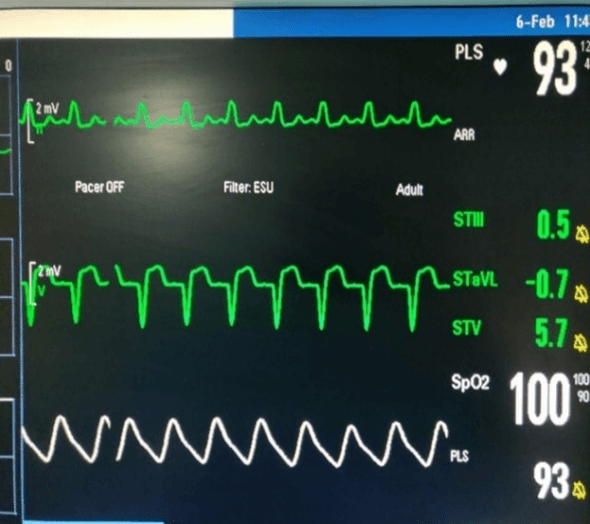
Figure 1: Preoperative monitor readings (before induction).
On arrival to the pre anaesthesia room, the monitors as per American society of Anaesthesia (ASA) standards were attached and the heart rate of 97 bpm with blood pressure of 136/97 mm Hg and Oxygen saturation of 98% (Figure 1). ECG showed persistent LBBB. The patient underwent the surgical procedure as per the institutional protocol. Intraoperatively, the heart rate settled down to 77 bpm after which the LBBB reverted to sinus rhythm (Figure 2). Although T wave inversion was seen which may be due to lead placement on the back, patient remained hemodynamically stable throughout the intraoperative period. After the surgery, neuromuscular blockade was reversed, and the trachea was extubated uneventfully. The post operative period showed LBBB pattern as in preoperative period when the heart rate exceeded 80 bpm. Patient was observed in the Intensive care unit and with cardiologist consultation, no active management was advised. Peri operative period was uneventful for the patient. Written informed consent was taken from the patient to share his data and images for publication reason.
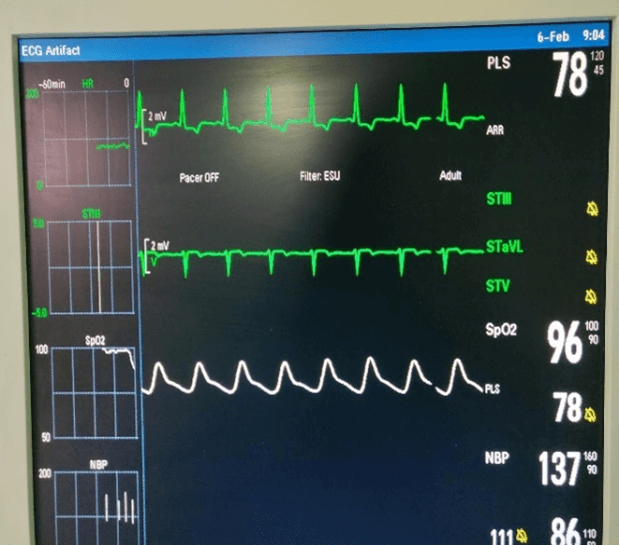
Figure 2: Intraoperative monitor readings (after intubation where heart rate settled below 77bpm).
Discussion
Electrical conduction originating from Sino atrial (SA) node travel through the pathways dividing into left and right bundle after the bundle of His. Any electrical disturbance can manifest as delayed transmission, erratic rhythm or irregular conduction. RBBB or LBBB results from delayed transmission through the Bundle of His [3].
LBBB is often associated with hypertension, myocarditis, coronary heart disease, aortic valve disease, cardiomyopathy etc. [4, 5]. It may be transient, intermittent or permanent where transient block can be due to phase 3 block, a phase 4 block, or a concealed conduction. Even a minor change in heart rate of 1 bpm can cause a BBB to appear or disappear. This has been coined as critical heart rate by Constantini [6]. The etiology can be attributed to aberration in conduction phase 3. As the heart rate increases above the critical point, it leads to manifestation of the block. Under general anaesthesia, when the heart rate dips below it, the block gets reverted back to sinus rhythm. Although literature documents few cases of reversion back to sinus rhythm and critical heart rate, the features which distinguish between more critical intra operative MI and other rhythm disturbances needs to be re explored. When to act is the need of the hour. Time is of essence in such scenarios.
LBBB always make the anaesthesiologist to be cautious during the peri operative period as any of the above causes may be present. Although benign but sometimes serious issues like acute MI may be masked under this and poses a significant challenge. Various scoring system have been published but Sgarbossa score is a validated score for diagnosis in patients of acute MI with LBBB [7]. A positive result is considered if 3 points are scored on the scale:
ST-segment elevation of at least 1 mm in a lead with QRS complex and T-wave concordant (5 points);
ST-segment depression of at least 1 mm in lead V1, V2, or V3 (3 points);
ST-segment elevation of at least 5 mm in a lead with a QRS complex and T-wave discordant (2 points).
Smith’s modification of Sgarbossa scale is also used clinically but it is time consuming [8]. Intraoperative LBBB diagnosis can be made by various modalities which alter the heart rate (valsalva, carotid massage, administration of atropine, neostigmine, esmolol or propranolol) but it should be done under controlled settings only [9]. Such maneuvers can be more detrimental in patients with cerebrovascular diseases. Holter monitoring is the gold standard for these patients and can shed more light to the etiology.
The mechanism for such aberration is not clear whether it is anatomical due to ventricular enlargement or neurogenic or pathological due to underlying disturbances. Rate dependent LBBB occurs due to prolonged refractory periods, the impulse is not transmitted further in Bundle of His hence manifesting as bundle branch block. When heart rate decreases, the impulse is conducted after the refractory period, hence completing the electrical circuit [10]. Rate dependent left bundle branch block may be associated with atypical chest pain, possibly related to the paradoxical cardiac movement occurring at onset of left bundle branch block, and not due to myocardial ischaemia [11]. This patient also did not have any symptoms related to LBBB and had good effort tolerance. No positive history for any stress related or otherwise events could be elucidated.
Another finding in this patient was paradoxical motion of septum, also known as septal bounce. During a 2D echocardiograph, the inter ventricular septum moves away from the placed transducer after the depolarization. It is followed by short trembling movement which coincides with T wave. Afterwards, the septum returns towards the transducer. This is seen normally but sometimes a paradoxical movement of the IVS is seen which has been coined as septal bounce [12]. Septal bounce is attributed to various causes: LBBB is one of them. Others are post cardiac surgeries, mitral stenosis, cardiac tamponade, pulmonary embolism and right atrial overload. In LBBB, there is discordance in electrical conduction and ventricular contraction resulting in dyssynchrony. Right ventricle is contracting earlier than the left, and the septum is displaced posteriorly in early systole. This has been termed as septal beaking by Dillon et al., the main cause behind it is reversal of transeptal pressure gradient [13]. Walmsley et al. has coined the same movement as ‘septal flash’ and noticed it larger the longer the delay between the right ventricle free wall and septal conduction although felt it occurred irrespective of the pressure gradient between the right and left ventricles [14].
Conclusion
In this case report, preoperatively the heart rate was higher than the critical heart rate which when settled under general anaesthesia, led to remission of LBBB to sinus rhythm. The patient remained asymptomatic throughout and had an uneventful peri operative period. Such cases may benefit from Holter monitoring later on to accurately know the etiology. Although it remained uneventful, due caution should always be used as an underlying acute MI may be missed. Sgarbossa scoring criteria shall be used and risk assessment shall be a multidisciplinary approach. Underlying MI must be differentiated from other rhythm disturbances so that the patient does not land up in a critical situation.
Presentation(s) or Awards at a Meeting
None.
Acknowledgement
None.
Funding
None.
Conflicts of Interest
None.
Author Contributions
Conceptualization, Data curation, Formal Analysis, Investigation, Methodology, Resources, Software, Supervision, Validation, Visualization, Writing – original draft, Writing – review and editing: RK; Funding acquisition: NIL.
Consent to Participate
The patient has given written informed consent to publish his data for scientific reasons provided his anonymity is maintained.
Ethical Approval
Not applicable.
Article Info
Article Type
Case ReportPublication history
Received: Thu 04, Aug 2022Accepted: Tue 16, Aug 2022
Published: Tue 20, Sep 2022
Copyright
© 2023 Ravneet Kaur Gill. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited. Hosting by Science Repository.DOI: 10.31487/j.SCR.2022.09.03
Author Info
Ravneet Kaur Gill Ashwani Mudgal
Corresponding Author
Ravneet Kaur GillAssistant Professor, Department of Anaesthesia, Dr B R Ambedkar State Institute of Medical sciences, Mohali, India
Figures & Tables
References
1. Tan NY, Witt CM, Oh
JK, Cha YM (2020) Left Bundle Branch Block: Current and Future
Perspectives. Circ Arrhythm
Electrophysiol 13: e008239. [Crossref]
2. Saad SM, Polani FS,
Lelorier P (2021) A Case of Intermittent Left Bundle Branch Block. Cureus
13: e15851. [Crossref]
3. Breithardt G,
Breithardt OA (2012) Left bundle branch block, an old-new entity. J Cardiovasc Transl Res 5: 107-116. [Crossref]
4. Bazoukis G, Tsimos
K, Korantzopoulos P (2016) Episodic Left Bundle Branch Block-A Comprehensive
Review of the Literature. Ann
Noninvasive Electrocardiol 21: 117-125. [Crossref]
5. Laney J, Tran T,
Motamed A (2020) Critical heart rate and left bundle-branch block resolution in
anesthesia. J Anaesthesiol Clin
Pharmacol 36: 282-285. [Crossref]
6. Costantini M (2014)
Intermittent bundle branch block: a clinical model for the study of
electrophysiological phenomena. G
Ital Cardiol (Rome) 15: 25-36. [Crossref]
7. Sgarbossa EB (1996)
Recent advances in the electrocardiographic diagnosis of myocardial infarction:
left bundle branch block and pacing. Pacing
Clin Electrophysiol 19: 1370-1379. [Crossref]
8. Smith SW, Dodd KW,
Henry TD, Dvorak DM, Pearce LA (2012) Diagnosis of ST-elevation myocardial
infarction in the presence of left bundle branch block with the ST-elevation to
S-wave ratio in a modified Sgarbossa rule. Ann Emerg Med 60: 766-776. [Crossref]
9. Silva AMOCD, Silva
EAGLD (2017) Intermittent left bundle branch block - reversal to normal
conduction during general anesthesia. Rev
Bras Anestesiol 67: 430-434. [Crossref]
10. Tyagi A, Sethi AK,
Agarwal V, Mohta M (2004) Rate-dependent left bundle branch block during
anaesthesia. Anaesth Intensive Care
32: 715-718. [Crossref]
11. Hertzeanu H, Aron
L, Shiner RJ, Kellerman J (1992) Exercise dependent complete left bundle branch
block, Eur Heart J 13: 1447-1451. [Crossref]
12. Clancy DJ, Mclean
A, Slama M, Orde SR (2018) Paradoxical septal motion: A diagnostic approach and
clinical relevance. Australas J
Ultrasound Med 21: 79-86. [Crossref]
13. Dillon JC, Chang S, Feigenbaum H (1974) Echocardiographic manifestations of left bundle branch block. Circulation 49: 876-880. [Crossref]
14. Walmsley J, Huntjens PR, Prinzen FW, Delhaas T, Lumens J (2016) Septal flash and septal rebound stretch have different underlying mechanisms. Am J Physiol Heart Circ Physiol 310: H394-H403. [Crossref]
