Clinical Impact of Biliary Candidiasis in Pancreatoduodenectomy: A Series of Cases
A B S T R A C T
Infectious complications play a prominent role in postoperative outcome of pancreatoduodenectomy. The analysis of the microorganisms responsible for these complications has focused on bacteria, and there is little documentation regarding the role of fungi. We present a case series with 8 patients who underwent pancreatoduodenectomy with positive bile cultures for Candida spp., in order to analyse the postoperative outcome.
Keywords
Candidiasis, pancreatectomy, postoperative complications, antifungal agents
Introduction
Infectious complications play a prominent role in postoperative outcome of pancreatoduodenectomy. Surgical site infection (SSI) and sepsis are some of the most frequent complications and have important clinical repercussions. Among the factors related to its occurrence, the existence of microorganisms in bile at the time of the surgery is of particular importance, a circumstance favoured by the performance of endoscopic retrograde cholangiopancreatography (ERCP) [1-3]. Thus far, the analysis of the microorganisms responsible for these complications has focused on bacteria, and there is little documentation regarding the role of fungi [2]. Although there are publications suggesting their association with the development of SSI and even pancreatic fistula, their impact on postoperative complications of pancreatoduodenectomy is not yet well understood [4, 5].
Case Series
In this case series we report patients who underwent pancreatoduodenectomy with positive bile cultures for Candida spp. The patients were treated in a third-level hospital between 2015 and 2018. Microbiological sampling was performed by puncturing the common hepatic duct with a subcutaneous needle before sectioning the same. Once the culture result was obtained, targeted treatment was administered according to the findings. If biliary candidiasis was detected, antifungal treatment was initiated even in the absence of symptoms. Of the total number of patients who underwent pancreatoduodenectomy (60), biliary candidiasis was detected in 13.3% (8 cases). All of them had a history of preoperative biliary drainage (PBD), 87.5% (7 cases) by ERCP and 12.5% (1 case) by cholecystostomy.
Table 1 shows the demographic variables, as well as the most relevant medical history of each patient. Median and mean age were 66 years. It is noteworthy that 75% of the patients (6 cases) had received prolonged antibiotic treatment (more than 7 days) in the weeks prior to the surgery. It is also worth highlighting the history of neoadjuvant treatment and admission to the intensive care unit, both of which appeared in 12.5% (1 case) of the patients. All patients underwent surgery for malignant disease, with pancreatic adenocarcinoma in 87.5% (7 cases) and distal cholangiocarcinoma in 12.5% (1 case). Median time from PBD to surgery was 45 days and mean time was 32 days. The antibiotic therapy and the antifungal treatment administered in each case according to the microbiological culture are also recorded.
Table 1: Descriptive table.
|
CASE |
1 |
2 |
3 |
4 |
5 |
6 |
7 |
8 |
|
Age (years) |
55 |
75 |
77 |
67 |
65 |
60 |
61 |
74 |
|
Sex |
Female |
Female |
Female |
Male |
Male |
Female |
Female |
Male |
|
ATB>7 days |
Yes |
Yes |
Yes |
Yes |
Yes |
Yes |
No |
Yes |
|
ICU admission previous weeks |
Yes |
No |
No |
No |
No |
No |
No |
No |
|
Neoadjuvant |
No |
No |
Yes |
No |
No |
No |
No |
No |
|
Tumor |
Pancreatic
adenocarcinoma |
Pancreatic
adenocarcinoma |
Pancreatic
adenocarcinoma |
Distal
cholangiocarcinoma |
Pancreatic
adenocarcinoma |
Pancreatic
adenocarcinoma |
Pancreatic
adenocarcinoma |
Pancreatic
adenocarcinoma |
|
PBD |
ERCP |
ERCP |
ERCP |
ERCP |
ERCP |
Cholecystostomy |
ERCP |
ERCP |
|
PBD to surgery (days) |
90 |
32 |
100 |
13 |
21 |
14 |
18 |
42 |
|
Surgical technique |
Cephalic
pancreato-duodenectomy |
Cephalic
pancreato-duodenectomy |
Total
pancreato-duodenectomy |
Cephalic
pancreato-duodenectomy |
Cephalic
pancreato-duodenectomy |
Cephalic
pancreato-duodenectomy |
Cephalic
pancreato-duodenectomy |
Cephalic
pancreato-duodenectomy |
|
Pancreatic anastomosis |
Pancreatico-gastrostomy |
Pancreatico-jejunostomy |
No |
Pancreatico-jejunostomy |
Pancreatico-
jejunostomy |
Pancreatico-gastrostomy |
Pancreatico-
jejunostomy |
Pancreatico-
jejunostomy |
|
Antibiotherapy |
Piperacillin
–Tazobactam, Linezolid |
Piperacillin-Tazobactam |
Piperacillin-Tazobactam,
Linezolid |
Piperacillin-Tazobactam |
Piperacillin- Tazobactam |
Vancomycin |
Piperacillin-Tazobactam |
Piperacillin-Tazobactam,
Linezolid |
|
Antifungal treatment |
Fluconazole |
Fluconazole |
Fluconazole |
Fluconazole |
Fluconazole |
Fluconazole |
Fluconazole |
Itraconazole |
*ATB: Antibiotherapy
*ICU: Intensive Care Unit
*PBD: Preoperative Biliary Drainage
*ERCP: Endoscopic Retrograde Cholangiopancreatography
Table 2: Postoperative morbility.
|
CASE |
1 |
2 |
3 |
4 |
5 |
6 |
7 |
8 |
|
Superficial incisional SSI |
No |
No |
No |
No |
No |
No |
No |
No |
|
Deep incisional SSI |
No |
No |
No |
No |
No |
No |
No |
No |
|
Organ /space SSI |
No |
No |
No |
No |
No |
No |
No |
No |
|
Sepsis |
No |
No |
No |
No |
No |
No |
No |
No |
|
Septic shock |
No |
No |
No |
No |
No |
No |
No |
No |
|
Pancreatic fistula |
No |
No |
No |
No |
No |
No |
No |
No |
|
Bile leak |
No |
No |
No |
No |
No |
No |
No |
No |
|
Hemorrhagic complications |
No |
No |
No |
Upper digestive bleeding |
No |
Bleeding from hepatic artery pseudoaneurysm |
No |
No |
|
Need for re-laparotomy |
No |
No |
No |
No |
No |
Yes |
No |
No |
|
Hospital readmission |
No |
No |
No |
Yes |
No |
Yes |
No |
No |
|
Hospital stay |
6 |
6 |
7 |
17 |
9 |
35 |
5 |
17 |
|
Mortality |
No |
No |
No |
No |
No |
No |
No |
No |
*SSI: Surgical Site
Infection
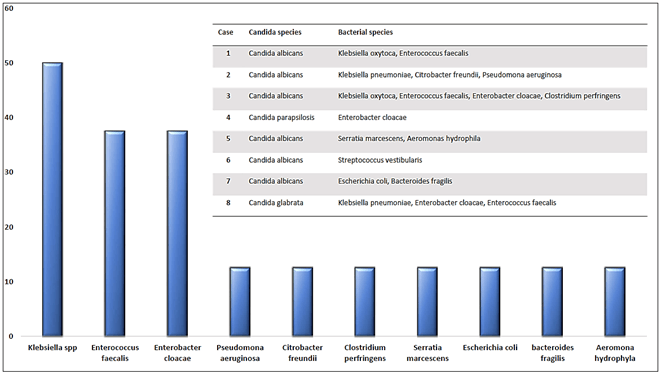
Table 2 shows the postoperative complications for each patient. The absence of infectious complications and postoperative mortality in our series is noteworthy. Regarding other complications, 25% (2 cases) of the patients presented postoperative hemorrhagic events. One patient had self-limited upper gastrointestinal hemorrhage. The other case presented intra-abdominal hemorrhage secondary to a hepatic artery pseudoaneurysm. It required urgent surgery with vascular reconstruction, showing good clinical evolution. Median hospital stay was 12.7 days and mean hospital stay was 8 days. A figure illustrating the bacterial species detected in bile fluid cultures along with Candida species is attached hereto (Figure 1).
Figure 1: Bacterial species isolated with Candida spp.
Discussion
Candida infections are of increasing interest due to their role in the development of nosocomial infections, mainly in intensive care units. Similarly, although documentation of biliary candidiasis in literature has been scarce in previous years, an increasing number of articles address the subject [6-8]. Since different fungal species are part of the microbiota of different regions of the body, one of the most important aspects is how to differentiate infection from colonisation. It is well known that various Candida species are part of the microbiota of the oral cavity and digestive tract, acting as commensal bacteria [7]. However, the biliary tract is a sterile compartment and the presence of Candida at this level should be considered as a pathological finding [7-9]. These microorganisms can infect the bile upstream from the intestinal tract, particularly in cases with a history of preoperative endoscopic biliary drainage [10-12]. In fact, ERCP has been recognised as an independent risk factor for the development of biliary candidiasis [6]. Also, a high correlation between Candida spp. detected in bile fluid and those present in the intestinal tract has been documented [7].
In addition to the upstream, there is a possibility of infection via the haematogenous route in cases of fungaemia and sepsis [7]. Other possible risk factors for the development of biliary candidiasis are prolonged antibiotherapy (more than 7 days) in the weeks prior to surgery, immunosuppression and advanced age [6, 7]. In accordance with these findings, 87.5% of the cases in our series had a history of ERCP and had received long-term antibiotic treatment in the weeks prior to surgery. The clinical impact of ERCP in the postoperative period following pancreatoduodenectomy, mainly in relation to the development of infectious complications, has been analysed in several articles [2, 13]. The alteration of the sphincteric mechanism of the bile duct caused by ERCP leads to the passage of enteric microorganisms, including Enterococcus spp., Klebsiella spp., Escherichia coli and Enterobacter spp. [2, 14-17]. Their presence in bile at the time of surgery is considered a risk factor for the development of postoperative infectious complications [1-3].
One of the findings in favour of this statement is the correlation between the micro-organisms present in bile and those detected in wound cultures upon the emergence of SSI [2, 18]. Although bacteria have been well analysed, so far there are not a large number of studies assessing the role of fungi in postoperative infectious morbidity in pancreatoduodenectomy. In this regard, Kato et al. reported that the presence of biliary candidiasis was significantly linked to the occurrence of SSI, is noteworthy [4, 5]. One characteristic of Candida spp. to consider is their ability to support bacterial growth. Candida spp. infection causes tissue damage that facilitates co-infection by bacteria. In addition, it can directly stimulate the growth of Staphylococcus aureus, Serratia marcescens and Streptococcus faecalis [19]. This may be linked to the high incidence of SSI in cases of biliary candidiasis [5].
In view of the foregoing, it is considered that biliary candidiasis should be treated whenever it is detected, even in cases without apparent symptoms [4]. In our clinical practice, we start antibiotic and antifungal treatment as soon as the bile culture result is available. To the best of our knowledge, it helps to avoid postoperative infectious complications. This is particularly important in immunocompromised patients, where early diagnosis and initiation of antifungal treatment is crucial [20].
In conclusion, although more studies are needed to provide further evidence, biliary candidiasis is an issue to be considered in patients undergoing pancreatoduodenectomy, especially in cases with ERCP or prolonged antibiotic therapy. Although it is just a case series, we believe that, given its possible relationship with the development of infectious complications, antifungal treatment should be considered whenever detected.
Conflicts of Interest
None.
Funding
None.
Article Info
Article Type
Case SeriesPublication history
Received: Fri 07, May 2021Accepted: Sat 22, May 2021
Published: Tue 08, Jun 2021
Copyright
© 2023 Miguel Ángel Suárez-Muñoz. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited. Hosting by Science Repository.DOI: 10.31487/j.SCR.2021.06.04
Author Info
Hinojosa-Arco LC Roldan-Rua JF Carranque Chaves GA Eslava-Cea Y Miguel Ángel Suárez-Muñoz
Corresponding Author
Miguel Ángel Suárez-MuñozLiver Transplant Unit, University Hospital Regional, Malaga, Spain
Figures & Tables
Table 1: Descriptive table.
|
CASE |
1 |
2 |
3 |
4 |
5 |
6 |
7 |
8 |
|
Age (years) |
55 |
75 |
77 |
67 |
65 |
60 |
61 |
74 |
|
Sex |
Female |
Female |
Female |
Male |
Male |
Female |
Female |
Male |
|
ATB>7 days |
Yes |
Yes |
Yes |
Yes |
Yes |
Yes |
No |
Yes |
|
ICU admission previous weeks |
Yes |
No |
No |
No |
No |
No |
No |
No |
|
Neoadjuvant |
No |
No |
Yes |
No |
No |
No |
No |
No |
|
Tumor |
Pancreatic
adenocarcinoma |
Pancreatic
adenocarcinoma |
Pancreatic
adenocarcinoma |
Distal
cholangiocarcinoma |
Pancreatic
adenocarcinoma |
Pancreatic
adenocarcinoma |
Pancreatic
adenocarcinoma |
Pancreatic
adenocarcinoma |
|
PBD |
ERCP |
ERCP |
ERCP |
ERCP |
ERCP |
Cholecystostomy |
ERCP |
ERCP |
|
PBD to surgery (days) |
90 |
32 |
100 |
13 |
21 |
14 |
18 |
42 |
|
Surgical technique |
Cephalic
pancreato-duodenectomy |
Cephalic
pancreato-duodenectomy |
Total
pancreato-duodenectomy |
Cephalic
pancreato-duodenectomy |
Cephalic
pancreato-duodenectomy |
Cephalic
pancreato-duodenectomy |
Cephalic
pancreato-duodenectomy |
Cephalic
pancreato-duodenectomy |
|
Pancreatic anastomosis |
Pancreatico-gastrostomy |
Pancreatico-jejunostomy |
No |
Pancreatico-jejunostomy |
Pancreatico-
jejunostomy |
Pancreatico-gastrostomy |
Pancreatico-
jejunostomy |
Pancreatico-
jejunostomy |
|
Antibiotherapy |
Piperacillin
–Tazobactam, Linezolid |
Piperacillin-Tazobactam |
Piperacillin-Tazobactam,
Linezolid |
Piperacillin-Tazobactam |
Piperacillin- Tazobactam |
Vancomycin |
Piperacillin-Tazobactam |
Piperacillin-Tazobactam,
Linezolid |
|
Antifungal treatment |
Fluconazole |
Fluconazole |
Fluconazole |
Fluconazole |
Fluconazole |
Fluconazole |
Fluconazole |
Itraconazole |
*ATB: Antibiotherapy
*ICU: Intensive Care Unit
*PBD: Preoperative Biliary Drainage
*ERCP: Endoscopic Retrograde Cholangiopancreatography
Table 2: Postoperative morbility.
|
CASE |
1 |
2 |
3 |
4 |
5 |
6 |
7 |
8 |
|
Superficial incisional SSI |
No |
No |
No |
No |
No |
No |
No |
No |
|
Deep incisional SSI |
No |
No |
No |
No |
No |
No |
No |
No |
|
Organ /space SSI |
No |
No |
No |
No |
No |
No |
No |
No |
|
Sepsis |
No |
No |
No |
No |
No |
No |
No |
No |
|
Septic shock |
No |
No |
No |
No |
No |
No |
No |
No |
|
Pancreatic fistula |
No |
No |
No |
No |
No |
No |
No |
No |
|
Bile leak |
No |
No |
No |
No |
No |
No |
No |
No |
|
Hemorrhagic complications |
No |
No |
No |
Upper digestive bleeding |
No |
Bleeding from hepatic artery pseudoaneurysm |
No |
No |
|
Need for re-laparotomy |
No |
No |
No |
No |
No |
Yes |
No |
No |
|
Hospital readmission |
No |
No |
No |
Yes |
No |
Yes |
No |
No |
|
Hospital stay |
6 |
6 |
7 |
17 |
9 |
35 |
5 |
17 |
|
Mortality |
No |
No |
No |
No |
No |
No |
No |
No |
*SSI: Surgical Site
Infection
References
1.
Okano K, Hirao T,
Unno M, Fujii T, Yoshitomi H et al. (2015) Postoperative infectious
complications after pancreatic resection. Br J Surg 102: 1551-1560. [Crossref]
2.
Herzog T, Belyaev
O, Akkuzu R, Hölling J, Uhl W et al. (2015) The Impact of Bile Duct Cultures on
Surgical Site Infections in Pancreatic Surgery. Surg Infect (Larchmt)
16: 443-449. [Crossref]
3.
Sugiura T, Mizuno
T, Okamura Y, Ito T, Yamamoto Y et al. (2015) Impact of bacterial contamination
of the abdominal cavity during pancreaticoduodenectomy on surgical-site
infection. Br J Surg 102: 1561-1566. [Crossref]
4.
Kato H, Iizawa Y, Kishiwada M, Usui M, Nakamura A et al. (2016) Negative Impact of Biliary Candidiasis on Early
and Late Postoperative Complications After Pancreatoduodenectomy Usefulness of
the CHROMagar Candida Plate for Identification. Pancreas 45: e45-e47. [Crossref]
5.
Kato H, Iizawa Y,
Nakamura K, Gyoten K, Hayasaki A et al. (2018) The Critical Role of Biliary
Candidiasis in Development of Surgical Site Infections after Pancreatoduodenectomy:
Results of Prospective Study Using a Selective Culture Medium for Candida
Species. Biomed Res Int 2018: 5939724. [Crossref]
6.
Lenz P,
Eckelskemper F, Erichsen T, Lankisch T, Dechêne A et al. (2014) Prospective
observational multicenter study to define a diagnostic algorithm for biliary
candidiasis. World J Gastroenterol 20: 12260-12268. [Crossref]
7.
Lenz P, Conrad B,
Kucharzik T, Hilker E, Fegeler W et al. (2009) Prevalence, associations, and
trends of biliary-tract candidiasis: a prospective observational study. Gastrointest
Endosc 70: 480-487. [Crossref]
8.
Domagk D, Fegeler
W, Conrad B, Menzel J, Domschke W et al. (2006) Biliary tract candidiasis:
diagnostic and therapeutic approaches in a case series. Am J Gastroenterol
101: 2530-2536. [Crossref]
9.
Ascioglu S, Rex
JH, de Pauw B, Bennett JE, Bille J et al. (2002) Defining opportunistic
invasive fungal infections in immunocompromised patients with cancer and
hematopoietic stem cell transplants: an international consensus. Clin Infect
Dis 34: 7-14. [Crossref]
10. Krüger CM, Adam U, Adam T, Kramer A, Heidecke CD et
al. (2019) Bacterobilia in pancreatic surgery-conclusions for perioperative
antibiotic prophylaxis. World J Gastroenterol 25: 6238-6247. [Crossref]
11. Scheufele F, Aichinger L, Jäger C, Demir IE, Schorn S
et al. (2017) Effect of preoperative biliary drainage on bacterial flora in
bile of patients with periampullary cancer. Br J Surg 104: e182- e188. [Crossref]
12. Scheufele F, Schorn S, Demir IE, Sargut M, Tieftrunk E
et al. (2017) Preoperative biliary stenting versus operation first in jaundiced
patients due to malignant lesions in the pancreatic head: A meta-analysis of
current literature. Surgery 161: 939-950. [Crossref]
13. Limongelli P, Pai M,
Bansi D, Thiallinagram A, Tait P et al. (2007)
Correlation between preoperative biliary drainage, bile duct contamination, and
postoperative outcomes for pancreatic surgery. Surgery 142: 313-318. [Crossref]
14. Windisch O, Frossard JL, Schiffer E, Harbarth S, Morel
P et al. (2019) Microbiologic Changes Induced by Biliary Drainage Require
Adapted Antibiotic Prophylaxis during Duodenopancreatectomy. Surg Infect
(Larchmt) 20: 677-682. [Crossref]
15. Stecca T, Nistri C,
Pauletti B, Greco A, Di Giacomo A et al. (2020)
Bacteriobilia resistance to antibiotic prophylaxis increases morbidity after
pancreaticoduodenectomy: a monocentric retrospective study of 128 patients. Updates
Surg 72: 1073-1080. [Crossref]
16. Fong ZV, McMillan MT,
Marchegiani G, Sahora K, Malleo G et al. (2016)
Discordance Between Perioperative Antibiotic Prophylaxis and Wound Infection
Cultures in Patients Undergoing Pancreaticoduodenectomy. JAMA Surg 151:
432-439. [Crossref]
17. Gavazzi F, Ridolfi C, Capretti
G, Angiolini MR, Morelli P et al. (2016)
Role of preoperative biliary stents, bile contamination and antibiotic
prophylaxis in surgical site infections after pancreaticoduodenectomy. BMC
Gastroenterol 16: 43. [Crossref]
18. Fathi AH, Jackson T, Barati M, Eghbalieh B, Siegel KA
et al. (2016) Extended Perioperative Antibiotic Coverage in Conjunction with
Intraoperative Bile Cultures Decreases Infectious Complications after
Pancreaticoduodenectomy. HPB Surg 2016: 3031749. [Crossref]
19. Carlson E (1983) Enhancement by Candida albicans of
Staphylococcus aureus, Serratia marcescens, and Streptococcus faecalis in the
establishment of infection in mice. Infect Immun 39: 193-197. [Crossref]
20. Pacholczyk M,
Lagiewska B, Lisik W, Wasiak D, Chmura A (2011) Invasive fungal infections
following liver transplantation - risk factors, incidence and outcome. Ann
Transplant 16: 14-16. [Crossref]
