Breast MRI Analysis for Surgeons Using Virtual Reality: Real-life Applications, Clinical Case Reports
A B S T R A C T
Breast cancer (BC) is the leading cause of cancer and cancer mortality among women worldwide. Surgery is the primary therapeutic strategy of BC in most of the cases. Efficient carcinologic and aesthetic resection requires breast surgeons to accurately understand medical images. Virtual reality (VR) is a promising avenue to improve surgical diagnosis and planning by producing high-precision images. Hereafter we report three cases of patients for which using AVATAR medical device for 3D visualization with VR would have helped to decide surgical strategy and adapt surgical procedure. The three cases are real-life examples of using the VR-AVATAR medical device for breast cancer surgery treatment: evaluation of the tumor response to neoadjuvant chemotherapy, decision for breast conservative or radical treatment, decision for loco-regional treatment in metastatic setting. Through these three real-life cases, we describe the potential impact of VR-AVATAR medical device use in clinical daily practice in breast cancer surgery. It seems like a useful tool, easy to use, providing high-quality images, helping with surgery planning and decisions.
Keywords
Breast cancer, breast surgery, breast MRI, virtual reality, oncoplastic surgery, innovation
Introduction
Breast cancer (BC) is the leading cause of cancer and cancer mortality among women worldwide. Surgery is the primary therapeutic strategy of BC in most of the cases. Efficient carcinologic and aesthetic resection requires breast surgeons to carry out mental projections of planar two-dimensional (2D) radiological images into three-dimensional (3D) surgical procedures and techniques. This 3D representation can be difficult to apprehend initially when analysing two-dimensional magnetic resonance image (MRI) scans. It has been reported that only 12% of surgeon medical faculty and 1% of surgery residents have followed a radiology curriculum in the US [1]. The surgeon is hence often limited in the exploitation of the medical images which, for oncology, contains among the most valuable clinical information.
As a mean of visualizing 3D structures through 2D medical imaging, virtual reality (VR) is a promising avenue to improve surgical diagnosis and planning [2-4]. VR is a natural vehicle through which 3D data can be easily understood [5]. Some visualization tools based on VR have been developed and AVATAR medical is one of them. Its usefulness for analysing breast MRI in the context of BC has been recently assessed [6].
Hereafter we report three cases of patients for which using AVATAR medical device for 3D visualization with VR would have helped to decide surgical strategy and adapt surgical procedure.
Case 1: Breast Conservative Treatment After Neoadjuvant Treatment with Axillary Lymph Node Dissection Using Virtual Reality
I Summary
In breast cancer, adapting the surgical procedure to residual disease in breast and axilla can be sometimes challenging after a neoadjuvant treatment. A precise dissection of pathologic axillary lymph nodes, tailored to initial disease and thus providing less long-term complications, remains a therapeutic challenge. In this case report, we report the ability to confirm an indication for breast conservative treatment and to somehow guide the lymph nodes dissection using 3D-VR MRI analysis.
II Introduction
This case is about a 62-year-old patient, treated for right breast cancer. The initial breast MRI showed a multi lobulated tumor measuring 41×25 mm in the Lower External Quadrant of the right breast with spicules up to the chest wall without invading it. At least six retro pectoral and internal mammary lymph nodes were visualized. The microbiopsy revealed an infiltrating ductal carcinoma of grade EE III, ER-positive, PR-negative, Her2-negative, Ki 67 40%, with positive axillary cytology.
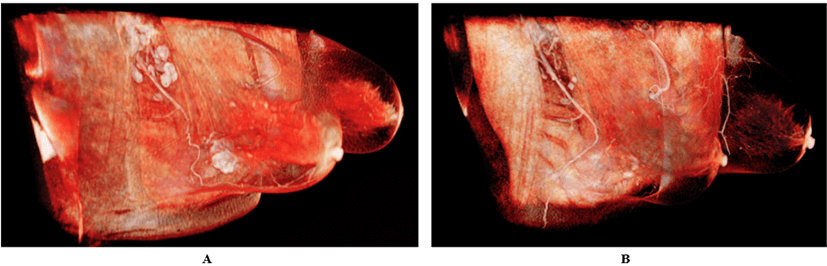
A neoadjuvant treatment was then proposed and performed, according to local and national treatment guidelines. The post neoadjuvant chemotherapy reevaluation MRI showed a partial tumor response in the Lower External Quadrant (-70%) and a normalization of axillary lymph nodes. Based on this treatment response, a breast conservative treatment was decided, and the patient underwent a partial mastectomy surgery, with axillary lymph node dissection. Both MRIs that had been done before (Figure 1A) and after (Figure 1B) neoadjuvant treatment have been secondarily visualized in AVATAR medical to assess whether the surgical therapeutic decision would have been confirmed.
Figure 1: A) pre-treatment MRI; B) post-treatment MRI.
III Methods
Both T1-weighted Gadolinium enhanced Dynamic Subtracted MRI of the chest that had been done before and after the neoadjuvant treatment have been uploaded into AVATAR medical to be visualized in 3D and then in virtual reality. In this study, we used an Oculus Rift S on a DELL G5 computer.
IV Findings
i Tumor Response to Neoadjuvant Treatment
By comparing both MRIs, we noticed that the tumor reduction was concentric, conversely to sometimes observed fragmented treatment response. It confirmed that a partial mastectomy could safely be performed.
ii Anatomy of Pathologic Lymph Nodes
On the initial MRI, VR was of great precision and helped to assess the anatomical features of the initial axillary disease. It helped determine the exact location of the pathologic lymph nodes along the right external mammary vein.
V Conclusion
AVATAR medical would have confirmed the decision for a partial mastectomy surgery. Complete axillary lymph node dissection would have been performed according to local and national guidelines. Nonetheless, the quality of VR images could help in tailoring the axillary lymph node dissection, focusing on initial pathologic lymph nodes. We think it could, in some selected cases, avoid large surgical axillary dissection and then reduce the long-term complications incidence.
Case 2: Conservative Breast Treatment for Multicentric Breast Tumor Using Virtual Reality
I Summary
In breast cancer surgery, the surgical strategy can sometimes be challenging due to multicentric lesions. Using a VR software as AVATAR medical allows the precise visualization of tumors and breast volumes based entirely on the patient’s MRI, strictly reproducing patient’s anatomical features. Here we report the ability to rapidly confirm and secure an indication for partial mastectomy for a multifocal and multicentric lesion in a metastatic 37-year-old patient.
II Introduction
The patient was a 37-year-old patient without previous medical history. She was diagnosed with a relatively large luminal B tumor type on the right breast with synchronous liver metastasis. The mammography with ultrasound showed a peri areolar mass of 32 mm, with two axillary adenomegalies. The MRI showed a retro areolar mass classified as American College of Radiology (ACR) category 5 on the right breast, and two lower internal and external masses with axillary lymph nodes involvement. The left breast was classified as an ACR2. The right mammary microbiopsy showed an infiltrating ductal carcinoma of grade EE III, Ki67 85% - ER-positive, PR-negative, HER2-negative. The microbiopsy of the lymph nodes showed a metastatic involvement.
In this metastatic setting, a first-line systemic treatment was initiated by hormone therapy and cycle inhibitors according to a national study protocol in which the patient was included. Due to the satisfying response of the metastatic disease after 6 months of the first-line treatment, a loco-regional treatment was considered and recommended by a multidisciplinary team. Due to the initial multicentric tumor feature, a radical breast surgery would have been recommended. A breast MRI was performed to adapt the surgical strategy and consider if a radical mastectomy could be avoided in this metastatic young patient.
Although the response was complete on the liver, the ultrasound, MRI and PET showed only partial response of the peri areolar tumor (-50% on the Ultrasound and -35% the MRI) and a remaining axillary involvement. Breast lesions were considered to be possibly removed by conservative breast surgery. Given the metastatic nature, the age of the patient and the potential impact of a radical treatment on quality of life, it was decided to perform a partial mastectomy with oncoplasty. The MRI was then visualized in AVATAR medical to assess whether this decision would have been confirmed.
III Methods
We selected the T1 weighted Gadolinium enhanced Dynamic Subtracted MRI of the chest that had been done for reevaluation. The image was then uploaded into AVATAR medical to be visualized in 3D and then in virtual reality. In this study, we used an Oculus Rift S on a DELL G5 computer.
IV Findings
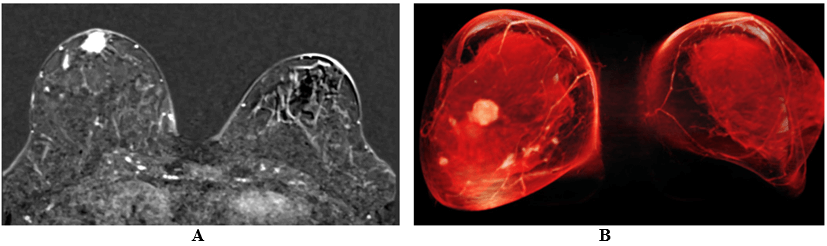
Analysing the breast MRI in virtual reality using AVATAR, the surgeon could assess and visualize the exact localization of the lesions (Figure 2A): two were in the lower quadrants and the third one at the union of all quadrants, which was not so evident in 2D-analysis (Figure 2B). MRI analysis using VR with AVATAR device would have helped to quickly confirm the surgical strategy consisting of a conservative breast treatment with no areolar complex conservation using Thorek's technique.
Figure 2: A) 2D visualization of breast MRI; B) VR visualization of Breast MRI.
V Conclusion
AVATAR medical helped to confirm the decision of a conservative breast surgery and would have been a useful tool to choose the best adapted oncoplastic technique.
Case 3: Breast Conservative Surgery for Peri-Areolar Breast Tumor Using Virtual Reality
I Summary
Oncoplastic surgery enlarges indications for conservative breast cancer treatments. However, uncertainty as to whether it can be safely performed remains in certain situations, even when the breast volume can accommodate it. With the aid of a virtual reality software, AVATAR medical, allowing a precise visualization of tumors and breast volumes based entirely on the patient’s MRI, we report the ability to rapidly confirm and secure an indication for breast conservative surgery of a large lesion in a 57-year-old patient. With the described approach, the patient did not have to suffer significant aesthetic issues from oncologic breast surgery without compromising safety.
II Introduction
A 57-year-old patient with a 48C cup size was admitted for a left breast cancer. The diagnosis began with an auto palpation of a left breast mass. Clinical breast exam revealed a 60 mm mass starting behind the areolar complex on its outer side and overflowing on the upper quadrants. The mammography with ultrasound of the left breast showed a unifocal peri areolar mass of 23×40×20 mm in the Superior External Quadrant, at 1 o’clock radius 2 cm from the nipple. An MRI was performed, confirming a peri areolar architectural distortion of 25×35×20 mm less than 2 cm from areolar complex. It was classified as American College of Radiology (ACR) category 5 on the left breast. The right breast was classified as ACR2.
The microbiopsy found an infiltrating ductal carcinoma of grade EE II, ER-positive, PR-positive, HER2-negative, Ki67: 10%. Given the clinical examination, a total mastectomy was first deemed necessary. But due to the size of the lesion and the mammary size, the surgical team decided to first perform a breast conservative surgery with a large external oncoplasty with a sentinel node. The MRI was then visualized in AVATAR medical to assess whether this decision would have been confirmed.
III Methods
The radiologist selected the T1 weighted Gadolinium enhanced Dynamic Subtracted MRI of the chest that had been done for diagnostic purposes. The image was then uploaded into AVATAR medical to be visualized in 3D and then in virtual reality. In this study, we used an Oculus Rift S on a DELL G5 computer.
IV Findings
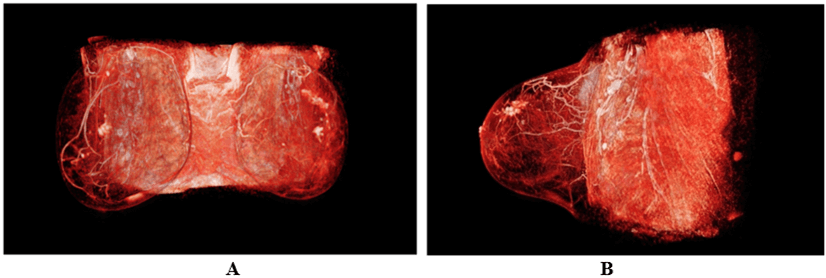
Reading the breast MRI in virtual reality using AVATAR (Figures 3A & 3B), we could easily confirm that the localization of the tumor was limited enough and sufficiently superficial to be accessible to a breast conservative treatment by large oncoplasty.
Figure 3: A) frontal view of 3D breast MRI; B) lateral view of 3D breast MRI.
V Conclusion
AVATAR medical confirmed the decision of breast conservative treatment. This 3D/VR visualization also helped the discussion between junior and senior surgeons (and also with radiologists) during multidisciplinary team meetings.
Conclusion
Through these three clinical cases, we describe the potential impact of AVATAR medical in simple clinical daily practice in breast cancer surgery. Here are selected cases but there are unlimited potential applications that could appear with the use of VR visualization. We think that, if daily used, it could accelerate surgical decisions in some situations, make surgeons better at medical imaging interpretation and surgical procedure preparation. It could also help teaching and communication over specialties and generations.
Article Info
Article Type
Case ReportPublication history
Received: Mon 05, Sep 2022Accepted: Sat 24, Sep 2022
Published: Tue 18, Oct 2022
Copyright
© 2023 Noemie Girard. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited. Hosting by Science Repository.DOI: 10.31487/j.SCR.2022.10.01
Author Info
Noemie Girard Thomas Gaillard Lauren Darrigues Lea Pauly Elodie Gauroy Enora Laas Jean Guillaume Feron Fabien Reyal
Corresponding Author
Noemie GirardGynecologic Cancer & Reconstructive Surgery Unit, Department of Surgery, Institut Curie, Paris, France
Figures & Tables
References
1. Butler KL, Chang Y,
DeMoya M, Feinstein A, Ferrada P et al. (2016) Needs assessment for a focused
radiology curriculum in surgical residency: a multicenter study. Am J Surg
211: 279-287. [Crossref]
2. Sadeghi AH, Taverne
YJHJ, Bogers AJJC, Mahtab EAF (2020) Immersive virtual reality surgical
planning of minimally invasive coronary artery bypass for Kawasaki disease. Eur
Heart J 41: 3279. [Crossref]
3. Cao C, Cerfolio RJ
(2019) Virtual or Augmented Reality to Enhance Surgical Education and Surgical
Planning. Thorac Surg Clin 29: 329-337. [Crossref]
4. Alsofy SZ,
Sakellaropoulou I, Stroop R (2020) Evaluation of Surgical Approaches for Tumor
Resection in the Deep Infratentorial Region and Impact of Virtual Reality
Technique for the Surgical Planning and Strategy. J Craniofac Surg 31:
1865-1869. [Crossref]
5. El Beheiry M, Doutreligne S, Caporal C, Ostertag C, Dahan M et al. (2019) Virtual Reality: Beyond Visualization. J Mol Biol 431: 1315-1321. [Crossref]
6. El Beheiry M, Gaillard T, Girard N, Darrigues L, Osdoit M et al. (2021) Breast Magnetic Resonance Image Analysis for Surgeons Using Virtual Reality: A Comparative Study. JCO Clin Cancer Inform 5: 1127-1133. [Crossref]
