A Rare Case of Primary B Cell Lymphoma of the Spine
A B S T R A C T
Spinal non-Hodgkin’s lymphomas are rare and often present late when the disease is in an advanced stage. We describe a case of primary B cell lymphoma diagnosed in a 74-year-old male, who presented with worsening back pain and unilateral leg weakness. Radiological imaging identified an abnormality within the T6 vertebral body, but analysis of initial vertebral body biopsies showed no clear evidence of malignancy. The diagnosis of high-grade B-cell lymphoma was only made following repeated bone biopsies and subsequent histopathological analysis. The patient’s care has since been transferred to Haematology and is currently undergoing intensive chemotherapy.
Keywords
Non-Hodgkin’s lymphoma, spinal Colour tumor, surgery, biopsy
Introduction
Spinal non-Hodgkin’s lymphomas (NHLs) are a rare form (1-2%) of extranodal lymphomas, which constitute 10-20% of all lymphomas [1, 2]. Back pain, neurological dysfunction and spinal instability are often a late presentation of systemic disease [3]. They may present as epidural lesions or intramedullary lesions, which mimic inflammatory lesions and primary spinal cord tumors [4]. In addition, epidural lymphomas, accounting for 9% of spinal epidural tumors, mainly involve the thoracic spine, whilst inconsistent evidence is available on lower incidence in the lumbar and cervical spine [2-4]. The diagnosis of primary lymphoma is dependent upon the identification of no involvement of other locations at the time of diagnosis, whereas secondary spinal disease may arise from haematogenous, venous via Batson’s plexus or lymphatic spread or drop metastasis from brain involvement [4-6].
Primary central nervous system (CNS) NHL mainly targets the brain parenchyma and leptomeninges, whilst the spinal cord is primarily affected by epidural primary or secondary deposits of NHL [7]. Spinal lymphomas are intriguing disorders, often discovered in association with distinctive clinicopathologic features, such as immunodeficiency, autoimmune disease, infection or other immunologic conditions. The past four decades have seen an increase in the diagnosis of NHL thanks to better understanding of its pathogenesis, improved diagnostic modalities and efficacious antineoplastic agents [8]. This paper presents the case of an adult male with primary spinal lymphoma who presented with back pain and a literature review of current advances in clinical management of this occurrence.
Case Report
A 74-year-old gentleman presented to the emergency department (ED) with sudden-onset left leg weakness following a fall from the bed. Prior to this, he had a 6-week history of progressively worsening central back pain, radiating to his left chest, for which he had presented to ED on two separate occasions within the previous 4 weeks. His past medical history included hypertension, atrial fibrillation, angina, non-insulin dependent type 2 diabetes mellitus and cholestasis. There was no history of malignancy.
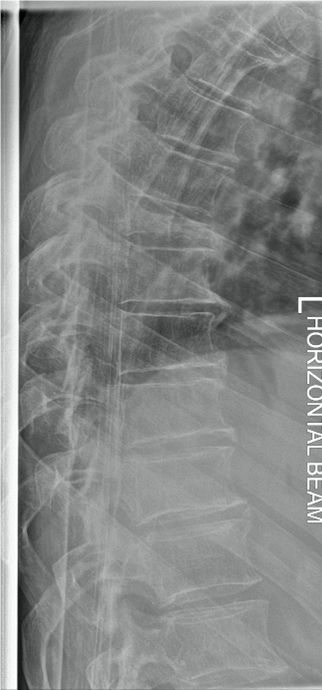
On examination, there was marked left leg weakness with gait incoordination and urinary retention. Radiological spinal imaging of the thoracic spine on admission showed a T6 vertebral body fracture with complete compression of the body of T6 (Figure 1). Computed tomography (CT) scan of the thoracic spine showed good vertebral alignment with soft tissue swelling around the fracture line, which was attributed to the acute inflammation following the fall. The T6 vertebral body had a distinct mottled appearance. This was thought to be due to either malignant infiltration or a haemangioma. No osteoblastic or osteolytic lesions were identified.
Figure 1: Sagittal x-ray of thoracic spine demonstrating T6 vertebral body fracture and compression.
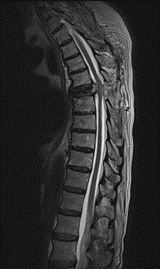
Initial magnetic resonance imaging (MRI) scan of the whole spine demonstrated multilevel spondylosis of the cervical spine, which was attributed to the patient’s older age. At the thoracic levels, there was a loss of 8mm of the anterior column height and T5/T6/T7 anterior cord compression (Figure 2). Scans also identified soft tissue oedema and bilateral foraminal narrowing of T5/T6 which was considered, at the time, to be suggestive of a haematoma secondary to the mechanical fall.
Figure 2: T2-weighted MRI of the thoracic spine, sagittal view demonstrating loss of anterior column height and T5/T6/T7 anterior cord.
Subsequently, the patient was transferred to the Neurosurgery Unit where he received 7 doses of 8mg dexamethasone to reduce oedema, awaiting spine stabilization surgery via T6 laminectomy and vertebroplasty. A biopsy of T6 vertebral body was also taken to investigate the possibility of malignancy. No post-operatively complications were reported, and the patient displayed improvement in his leg pain and gait coordination, despite still relying on a wheeled Zimmer frame + two supports to mobilize. A repeat MRI of the thoracic spine post-operatively showed no discrete haematoma, unlike the initial whole spine MRI, but did show evidence of osteomalacia (Figure 3).
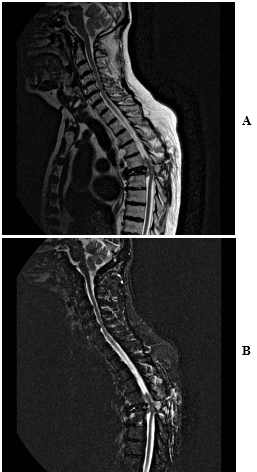
Figure 3: Post-operative T2-weighted MRI of the thoracic spine, demonstrating no oedema but moderate osteolytic bone lesions.
Figure 4: A) T2-weighted of the thoracic spine, demonstrating postoperative further collapse of T6 with new posterior cord compression at T6A. B) STIR MRI of the thoracic spine, demonstrating postoperative further collapse of T6 with new posterior cord compression at T6.
Histopathology report of the biopsies taken intraoperatively found no convincing evidence of malignancy. Microscopy found mostly bone and necrotic matter with very few viable cells. Further cytological analysis found no tumor cells and no known cancer markers, such as MNF116, were absent. The patient was referred to the general cancer Multidisciplinary Team (MDT) review, who found no evidence of malignancy, and he was subsequently transferred to the specialist rehabilitation unit at Pinderfields Hospital.
Approximately 6 weeks post-operatively, whilst as an in-patient in Pinderfields Hospital, the patient had a deterioration in power of left leg. New MRI scans showed there was further collapse of T6 with new posterior cord compression (Figure 4). A new lesion was also noted at T6. In light of this, the patient was transferred back to Neurosurgery at Hull Royal Infirmary for further management. On re-admission, the patient had reduced power in both lower limbs. Left lower limb had 3/5 MRC power grade at L2 and 4/5 at levels L3/S1. The right lower limb had a 4/5 MRC power grade at all levels.
Current differential diagnoses were spinal metastases and multiple myeloma. A repeat CT thorax, abdomen and pelvis scan was ordered to investigate these, but no evidence of malignancy was found. A repeat x-ray of the thoracic spine was unchanged from the previous scans done. Screening for multiple myeloma was completed; serum free light chain analysis found increased levels of both Kappa and Lambda chains, but with a normal ratio. There was also increased levels of alpha-2 globulin, but there were no Bence Jones protein or paraprotein found.
A second operation was arranged to decompress the posterior part of the cord, to aid diagnosis of the underlying cause and to help prevent further deterioration of neurological function. Access was via the old midline scar from the previous decompression with x-ray guidance to confirm the correct level. Intraoperatively, a suspicious soft-tissue mass was located attached to the dura at T5-T7, which was excised to achieve gross total resection and samples were sent to histopathology. Abnormal scar tissue causing compression of the dura at T5-T7 was also found.
Histological report from the suspicious mass sample showed paraspinal tissue with extensive pleomorphic nuclei, some of which had prominent nucleoli showing different stages of mitotic activity and apoptosis. This was now suggestive of high-grade B cell lymphoma. Immunological analysis of the samples showed CD45 and CD20 were expressed, but the samples were still negative for cytokeratin tumor markers (MNF116). At the date of write-up, the patient’s care had been transferred to Haematology, who currently plan on initiating the R-CHOP (rituximab, cyclophosphamide, doxorubicin hydrochloride, vincristine, prednisolone) chemotherapy regime with an adjunct of Methotrexate.
Discussion
Spinal NHLs have been reported in all ages but mainly affect the fifth to seventh decades of life [3, 9]. Common presenting symptoms include weakness, sensory loss, spasticity, pain and bowel or bladder dysfunction [4, 3]. ‘B’ symptoms of fever, night sweats and weight loss may also be present in a minority of patients [10].
In this patient, there was an initially low suspicion for malignancy due to the presence of non-specific neurological symptoms and the association of onset of symptoms with the recent fall. Furthermore, the patient did not complain of other symptoms, such as weight loss, loss of appetite or night sweats. Lastly, there was no background of immunocompromise, which is common in extranodal presentations of NHL. Nonetheless, further imaging raised the suspicion for malignant infiltration of the spine, which triggered the referral to our neurosurgical department.
As demonstrated by this case, NHL has a predilection for the thoracic spine thanks to its plasticity and length, which are capable of accommodating bulky disease, and the concentrated lymphatic drainage [11, 12]. Furthermore, males are predominantly affected compared to females [13, 3]. It is hypothesized that spinal lymphomas arise from the paravertebral ganglion or the epidural lymphoid tissue, then enter the epidural space via the vertebral foramen [14]. This is supported by evidence of tumor extension into the neural foramina and epidural space on MRI in previous studies as well as this report [2, 15, 16]. Spinal lymphomas are believed to uniquely possess this type of tumor growth, which achieves cord invasion without vertebral bone destruction. Nonetheless, lack of bone destruction or erosion is not a specific or sensitive finding for primary lymphomas. In fact, primary lesions may also be intraosseous, causing bone erosion following tumor growth Indeed, this has been described in the literature and is also supported by this case that demonstrated significant vertebral erosion at T6 [9, 16].
A number of protocols laying out a pathway to diagnosing spinal lymphomas are available in the literature. If suspecting a diagnosis of spinal lymphoma, it is imperative to exclude other localizations to differentiate between primary disease and secondary lesions due to metastatic spread of systemic lymphoma [2]. MRI of the brain and spine should be the preferred imaging modality and first-line mode of investigation in spinal lymphomas [4]. Solitary lesions are most commonly seen, as demonstrated by this case, but lesions throughout the spinal cord have also been reported [2, 17]. Isointense or hypointense homogenous lesions may be described in concomitance with contrast enhancement or foramina extension [15, 16]. Nonetheless, spinal lymphomas may often undergo the initial diagnostic journey for bone erosion or destruction on CT or X-ray. Furthermore, positron emission tomography/computed tomography (PET/CT) offers excellent imaging due to high avidity for 18F fluorodeoxyglucose of NHL, which appears well demarcated [4, 18].
Subsequent investigations may include cerebrospinal (CSF) cytology, blood evaluation for cell counts, glucose and protein levels, CSF and peripheral blood flow cytometry, and tissue biopsy. Previous research has demonstrated the potential for CFS flow cytometry in combination with CFS cytology to establish a quick diagnosis of primary or secondary lymphoma and to exclude inflammatory diseases [19, 20]. Nevertheless, CSF cytology may report as inconclusive, which is known not to exclude a diagnosis of CNS lymphoma [21]. The role of biopsy in itself is also greatly debated due to the questionable safety of a biopsy of the spinal cord, which may result in irreversible neurological damage. If the suspicion for lymphoma is high, efforts should be made to locate a primary focus of systemic lymphoma via peripheral blood flow cytometry and bone marrow biopsy prior to taking a spinal cord biopsy [4].
In particular, classical neurosurgical teaching is known to suggest that pre-operative corticosteroid administration reduces the diagnostic accuracy of tissue sampling [22]. This is believed to be due disruption of B-cell lymphoma cells which are not protected from steroid-induced apoptosis, causing lesions to appear with histologically destructive and demyelinating features: the so-called sentinel lesions. These are often difficult to distinguish from demyelinating disease [23].
In this case, an initial surgical approach was performed for spine stabilization and a tissue biopsy was obtained from the T6 vertebra, which did not demonstrate signs of malignancy. However, the patient had undergone pre-operative corticosteroid treatment prior to tissue sampling, which may be responsible for the inconclusive report. Nonetheless, no sentinel lesions were observed. In contrast, similarly to other published cases, our patient subsequently further deteriorated without regular corticosteroid administration [24]. A second lesion was visualized on imaging and histological examination during the second biopsy demonstrated high suspicion for high-grade B cell lymphoma.
Therefore, if imaging is suggestive of lymphoma, patients should undergo CFS cytology and flow cytometry prior to steroid administration to prevent CSF artefacts, and the scope of cord biopsies should be limited to cases with inconclusive imaging and haematological findings [4].
Due to the low incidence of spinal NHL, the evidence on management is inconsistent. High dose intravenous chemotherapy agents, such as methotrexate, alkylating agents or antimetabolites, achieved full remission in previous studies [4, 19, 21, 25, 26]. Furthermore, chemotherapy with adjuvant immunomodulator therapy may prove indispensable in treating spinal NHL. However, oral chemotherapy is not effective in treating these tumors [27]. Additionally, consideration for the risk of systemic toxicity and tolerance to the drug must be taken into account when prescribing the regimen, tailoring to individual patients [27].
Evidence on the application is highly variable. For example, it may be administered in palliative cases with low tolerance to high dose chemotherapy [4]. In contrast, radiotherapy has also been used as first-line therapy even in cases of neurological decline due to the radiosensitivity of lymphomas [28]. Nonetheless, radiation does not appear to provide significant advantage to the holistic treatment [4].
The role of surgical resection is greatly disputed and may not be as significant as intravenous chemotherapy, with the only agreed indication remaining for the management of spinal instability [4, 29]. For instance, there is evidence of primary surgical decompression improving neurological outcome [30]. In contrast, other research proved surgery with radiotherapy or surgery alone did not provide any additional benefit compared to sole radiotherapy or non-surgical management, respectively [31, 32]. Nonetheless, surgery is often provided in concomitance to other treatment modalities, to obtain tissue samples of definite diagnosis or to stabilize the spine [24, 30]. Of interest, only a recent study explored the outcomes following surgical intervention, reporting 77% of all mortality in the surgical group [21].
Numerous protocols for combined regimens of chemotherapy and radiotherapy have been proposed, demonstrated favourable outcomes and response to chemoradiation within days [10, 29, 30, 33-35]. In specific, our patient has been arranged to undergo R-CHOP regimen, which has been shown to provide positive outcomes [35, 29].
Extranodal NHL has intrinsically a poor prognosis [2]. Survival outcome in spinal NHL improved significantly with systemic chemotherapy. Nonetheless, remission rates and survival vary inconsistently across studies, from 10% at 1 year to 36% at 2 years [36, 9]. Immunosuppression, increasing age, high grade histopathology, significant neurological compromise and elevated LHD serum level and CSF protein concentration are predictors of grave prognosis [37].
Conclusion
NHL of the spine is a rare condition with a complex diagnosis. This case demonstrated the need to consider spinal lymphoma as a differential diagnosis at early stages of presentation and clinical diagnosis. Furthermore, this is a typical case in which symptomatic presentation has occurred at a late stage of the disease progression. Early differential recognition may improve the recognition of this disorder and prevention of further neurological deterioration. Aggressive treatment is crucial to survival.
Author Contributions
All authors: guarantors of integrity of entire study; all authors: study concepts/study design; SS and VC: data acquisition and data analysis/interpretation; all authors: manuscript drafting or manuscript revision for important intellectual content; all authors: agrees to ensure any questions related to the work are appropriately resolved; VC: literature search; all authors: manuscript editing.
Conflicts of Interest
None.
Consent
The patient described in this report has given full written consent to the inclusion of material relating to themselves and their medical history. They also understand that this report is fully anonymized and that they cannot be identified from this report.
Article Info
Article Type
Case Report and Review of the LiteraturePublication history
Received: Sat 26, Mar 2022Accepted: Mon 18, Apr 2022
Published: Sat 30, Apr 2022
Copyright
© 2023 Samantha Strickland. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited. Hosting by Science Repository.DOI: 10.31487/j.SCR.2022.04.01
Author Info
Samantha Strickland Vassili Crispi Efosa Ukponmwan Shuaibu Dambatta
Corresponding Author
Samantha StricklandDr. Gray’s Hospital, NHS Grampian, Elgin, UK
Figures & Tables

References
1. Mally R, Sharma M,
Khan S, Velho V (2011) Primary Lumbo-sacral Spinal Epidural Non-Hodgkin's
Lymphoma: A Case Report and Review of Literature. Asian Spine J 5:
192-195. [Crossref]
2. Moussaly E, Nazha
B, Zaarour M, Atallah JP (2015) Primary Non-Hodgkin's Lymphoma of the Spine: A
Case Report and Literature Review. World J Oncol 6: 459-463. [Crossref]
3. Hashi S, Goodwin
CR, Ahmed AK, Sciubba DM (2018) Management of extranodal lymphoma of the spine:
a study of 30 patients. CNS Oncol 7: CNS11. [Crossref]
4. D'cruz J, Adeeb N,
Von Burton G, Georgescu M-M, Larmeu L et al. (2020) Diagnosis and management of
intramedullary spinal cord lymphoma: A case illustration and review of
literature. Interdisciplinary Neurosurgery 19: 100552.
5. Batson OV (1940)
THE FUNCTION OF THE VERTEBRAL VEINS AND THEIR ROLE IN THE SPREAD OF METASTASES.
Ann Surg 112: 138-149. [Crossref]
6. Costigan DA,
Winkelman MD (1985) Intramedullary spinal cord metastasis. A
clinicopathological study of 13 cases. J Neurosurg 62: 227-233. [Crossref]
7. Roug IK, Mccartney
LB (2012) Metastatic non-Hodgkin lymphoma presenting as low back pain and
radiculopathy: a case report. J Chiropr Med 11: 202-206. [Crossref]
8. Metzger ML,
Mauz-Körholz C (2019) Epidemiology, outcome, targeted agents and immunotherapy
in adolescent and young adult non-Hodgkin and Hodgkin lymphoma. Br J
Haematol 185: 1142-1157. [Crossref]
9. Perry JR, Deodhare
SS, Bilbao JM, Murray D, Muller P (1993) The significance of spinal cord
compression as the initial manifestation of lymphoma. Neurosurgery 32:
157-162. [Crossref]
10. Tang Y, Yang X,
Xiao J, Liu K, Yan W et al. (2013) Clinical outcomes of treatment for spinal
cord compression due to primary non-Hodgkin lymphoma. Spine J 13:
641-650. [Crossref]
11. Epelbaum R, Haim N,
Ben-Shahar M, Ben-Arie Y, Feinsod M et al. (1986) Non-Hodgkin's lymphoma
presenting with spinal epidural involvement. Cancer 58: 2120-2124. [Crossref]
12. Mullins GM, Flynn
JP, El-Mahdi AM, Mcqueen JD, Jr Owens AH (1971) Malignant lymphoma of the
spinal epidural space. Ann Intern Med: 74: 416-423. [Crossref]
13. Haddad P, Thaell
JF, Kiely JM, Harrison EG, Miller RH (1976) Lymphoma of the spinal extradural
space. Cancer 38: 1862-1866. [Crossref]
14. Seo JY, Ha KY, Kim
MU, Kim YC, Kim YH (2014) Spinal cord compression by B-cell lymphoma,
unclassifiable, with features intermediate between diffuse large B-cell
lymphoma and Burkitt lymphoma in a patient seropositive for human
immunodeficiency virus: a case report. J Med Case Rep 8: 324. [Crossref]
15. Haque S, Law M,
Abrey LE, Young RJ (2008) Imaging of lymphoma of the central nervous system,
spine, and orbit. Radiol Clin North Am 46: 339-361. [Crossref]
16. Mascalchi M, Torselli P, Falaschi F, Pozzo GD (1995) MRI of spinal epidural
lymphoma. Neuroradiology 37: 303-307. [Crossref]
17. Jiménez De La PEÑA
MD, Vicente LG, Alonso RC, Cabero SF, Suárez AM (2017) The Multiple Faces of
Nervous System Lymphoma. Atypical Magnetic Resonance Imaging Features and
Contribution of the Advanced Imaging. Curr Probl Diagn Radiol 46:
136-145. [Crossref]
18. Mapelli P, Vanoli
EG, Picchio M, Gianolli L (2013) Spinal cord involvement secondary to
non-Hodgkin's lymphoma identified by ¹⁸F-FDG PET/CT. Rev Esp Med Nucl Imagen
Mol 32: 125. [Crossref]
19. Benz R, Viecelli A,
Taverna C, Schelosky L (2012) Paroxysmal non-kinesigenic dyskinesia due to
spinal cord infiltration of low-grade B cell non-Hodgkin's lymphoma. Ann
Hematol 91: 463-465. [Crossref]
20. Feng L, Chen D,
Zhou H, Shen C, Wang H et al. (2018) Spinal primary central nervous system
lymphoma: Case report and literature review. J Clin Neurosci 50: 16-19.
[Crossref]
21. Broen M, Draak T,
Riedl RG, Weber WE (2014) Diffuse large B-cell lymphoma of the cauda equina. BMJ
Case Rep. [Crossref]
22. Jiménez de la Peña MD, Vicente LG, Alonso RC, Cabero SF, Suárez AM et al. (2017) The Multiple
Faces of Nervous System Lymphoma. Atypical Magnetic Resonance Imaging Features
and Contribution of the Advanced Imaging. Curr Probl Diagn Radiol 46:
136-145. [Crossref]
23. Bashir R,
Chamberlain M, Ruby E, Hochberg FH (1996) T-cell infiltration of primary CNS
lymphoma. Neurology 46: 440-444. [Crossref]
24. Yamamoto J,
Shimajiri S, Nakano Y, Nishizawa S (2014) Primary central nervous system
lymphoma with preceding spontaneous pseudotumoral demyelination in an
immunocompetent adult patient: A case report and literature review. Oncol
Lett 7: 1835-1838. [Crossref]
25. Ezon IC, Barteselli
G, Rosenberg J, Freeman WR (2014) Concurrent primary vitreoretinal and spinal
cord lymphoma: a unique entity. JAMA Ophthalmol 132: 902-904. [Crossref]
26. Guzik G (2018)
Primary B-cell Spinal Cord Lymphoma of the Cervical Spine. Ortop Traumatol
Rehabil 20: 219-227. [Crossref]
27. Morita M, Osawa M,
Naruse H, Nakamura H (2009) Primary NK/T-cell lymphoma of the cauda equina: a
case report and literature review. Spine (Phila Pa 1976) 34: E882-E885.
[Crossref]
28. Kaloostian PE,
Yurter A, Zadnik PL, Sciubba DM, Gokaslan ZL (2014) Current paradigms for
metastatic spinal disease: an evidence-based review. Ann Surg Oncol 21:
248-262. [Crossref]
29. Laufer I, Rubin DG,
Lis E, Cox BW, Stubblefield MD et al. (2013) The NOMS framework: approach to
the treatment of spinal metastatic tumors. Oncologist 18: 744-751. [Crossref]
30. Chang CM, Chen HC,
Yang Y, Wang RC, Hwang WL et al. (2013) Surgical decompression improves
recovery from neurological deficit and may provide a survival benefit in
patients with diffuse large B-cell lymphoma-associated spinal cord compression:
a case-series study. World J Surg Oncol 11: 90. [Crossref]
31. Aabo K,
Walbom-Jørgensen S (1986) Central nervous system complications by malignant
lymphomas: radiation schedule and treatment results. Int J Radiat Oncol Biol
Phys 12: 197-202. [Crossref]
32. Peng X, Wan Y, Chen
Y, Chen L, He A et al. (2009) Primary non-Hodgkin's lymphoma of the spine with
neurologic compression treated by radiotherapy and chemotherapy alone or
combined with surgical decompression. Oncol Rep 21: 1269-1275. [Crossref]
33. Bekar A, Cordan T,
Evrensel T, Tolunay S (2001) A case of primary spinal intramedullary lymphoma. Surg
Neurol 55: 261-264. [Crossref]
34. Han S, Yang X,
Jiang D, Zhou W, Liu T et al. (2016) Surgical Outcomes and Prognostic Factors
in Patients With Diffuse Large B-cell Lymphoma-associated Metastatic Spinal
Cord Compression. Spine (Phila Pa 1976) 41: E943-E948. [Crossref]
35. Harris E, Butler
JS, Cassidy N (2014) Aggressive plasmablastic lymphoma of the thoracic spine
presenting as acute spinal cord compression in a case of asymptomatic
undiagnosed human immunodeficiency virus infection. Spine J 14: e1-e5. [Crossref]
36. Flanagan EP, O'neill BP, Porter AB, Lanzino G, Haberman TM et al. (2011) Primary intramedullary spinal cord lymphoma. Neurology 77: 784-791. [Crossref]
37. Ferreri AJM, Blay JY, Reni M, Pasini F, Spina M et al. (2003) Prognostic scoring system for primary CNS lymphomas: the International Extranodal Lymphoma Study Group experience. J Clin Oncol 21: 266-272. [Crossref]
