A Rare Case of De Garengeot Hernia: A Challenging Diagnosis and a New Approach
A B S T R A C T
De Garengeot’s hernia is a rare entity in which the appendix is located within a femoral hernia and is almost invariably encountered incarcerated in an emergency setting. The clinical presentation is usually that of an incarcerated femoral hernia and is indistinguishable from other incarcerated femoral hernias. Here, we report on a 48-year-old female patient, known for a post-operative chronic seroma in the right groin since childhood, with a rare clinical presentation of a De Garengeot hernia. An abdominal CT-scan was performed, revealing an appendicitis with a stercolith in a femoral hernia. Generally, an inguinal approach alone (McVay procedure) is chosen and provides access for both appendectomy and hernia repair. In the absence of concomitant acute appendicitis, trans-abdominal pro-peritoneal laparoscopy (TAPP) could also be used as a single approach. In case of a rare presentation of acute appendicitis with probable contamination of the groin, we propose the double approach of laparoscopic appendectomy and hernia repair either with (if hernia sac is not opened during surgery) or without mesh. This approach is not yet described in the literature, and we think it the best technique to perform the appendectomy and hernia repair with little contamination of the groin.
Keywords
De Garengeot hernia, appendicitis, laparoscopic approach
Case Presentation
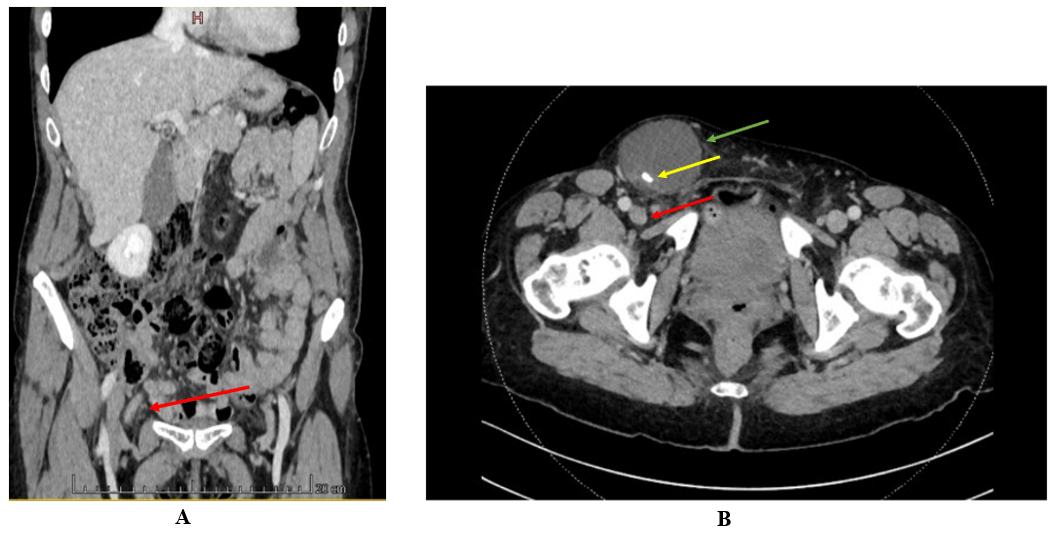
We report on a patient with a rare clinical presentation of a De Garengeot hernia. A 48-year-old female patient, known for a chronic seroma in the right groin since a right inguinal endovascular approach for the treatment of an atrial septal defect in her childhood, developed a progressive right iliac fossa pain over the last three days. She had no pain in the right groin. She also described an increase in the size of her seroma. Clinical examination reveals pain at the palpation of the right iliac fossa. There was an irreducible bulge in the right groin, but its palpation elicited no pain. There was no inflammatory syndrome. An abdominal CT scan was performed to complete diagnosis, revealing an appendicitis with a stercolith in a femoral hernia (Figure 1).
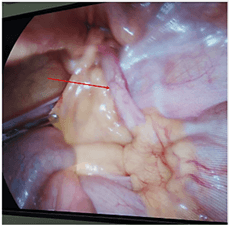
We went to surgery with a double approach. We started with an exploratory laparoscopy (Figure 2). We found that only the tip of the appendix was incarcerated. We managed to reduce the De Garengeot hernia via laparoscopic traction and external pressure and performed a laparoscopic appendectomy. We completed the surgery with a femoral approach. We opened the hernial sac, sampled the seroma content for microbial study. Because of the potentially infected seroma, we decided not to implant a mesh and performed a McVay procedure. The patient was discharged two days later; the seroma content was sterile. Follow-up at 6 weeks showed no complication.
De Garengeot’s hernia, described the first time in 1731, is a rare entity in which the appendix is located within a femoral hernia and is almost invariably encountered incarcerated in an emergency setting with concomitant appendicitis. It is important to not confuse it with Amyand’s hernia, which is defined as an inguinal hernia containing the appendix, described in 1735 [1].
De Garengeot’s hernia is rare, it accounts for 1% of hernias, and only 222 cases have been described in the literature since 1925 [2, 3]. Only 0.08%-0.13% of them present with a simultaneous acute appendicitis [4]. The clinical presentation is usually that of an incarcerated femoral hernia and is indistinguishable from other incarcerated femoral hernias on clinical examination. In the series of Linder et al., the most common clinical finding (87/90) was a mass in the inguinal region, of which pain was documented in 74.4% [5]. Pre-operative diagnosis is established in only 31.5% of the cases; the majority of patients are taken to surgery for simple femoral hernia incarceration. Generally, an inguinal approach alone is chosen, and provided access for both appendectomy and hernia repair [6]. The most common hernia repair is through suture technique, and with non-absorbable material. The most frequently specified methods are the McVay, Cooper ligament suture techniques, and the Rives [7].
Figure 1: Image of abdominal CT showing the appendix in the femoral hernia with a seroma. A) Coronal view of the appendix next to the femoral vessels (red arrow). B) Axial view of the appendix next to the femoral vessels (red arrow), the chronic seroma (green arrow) and the stercolith in the hernia (yellow arrow).
Figure 2: Laparoscopic image of the appendix in the femoral hernia.
Our described clinical presentation was uncommon for an incarcerated De Garengeot hernia as the patient had no inguinal/femoral pain but only a right iliac fossa pain. The history of a surgical vascular right inguinal access in her childhood, as well as the presence of a chronic seroma, challenged the diagnosis. Fortunately, CT-scan was readily available, allowing for an early diagnosis and treatment of this rare clinical presentation.
Conclusion
In conclusion, De Garengeot’s hernia is a rare entity, and its diagnosis can be challenging. Imaging is not always necessary but can be useful in planning a surgical approach, as an inguinal-only approach could be challenging in ligating the base of the appendix. In the absence of the concomitant acute appendicitis, trans-abdominal pro-peritoneal laparoscopy (TAPP) could be used as a single approach to perform both appendectomy and mesh repair. In case of a rare presentation of acute appendicitis with probable contamination of the groin region, we propose the double approach of laparoscopic appendectomy and hernia repair either with (if hernia sac is not opened during surgery) or without mesh. This approach is not yet described in the literature, and we think it the best technique to perform the appendectomy and hernia repair with little contamination of the groin.
Author Contributions
Dr. Sleiman Marwan-Julien: Date curation, writing original draft, writing & review; Dr. Litchinko Alexis: Writing and review; Professor Toso: Supervision and review; Professor Ris: Supervision and review; Dr. Delaune Vaihere: Writing and review.
Article Info
Article Type
Case ReportPublication history
Received: Tue 06, Apr 2021Accepted: Tue 20, Apr 2021
Published: Mon 03, May 2021
Copyright
© 2023 Sleiman Marwan Julien. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited. Hosting by Science Repository.DOI: 10.31487/j.SCR.2021.05.01
Author Info
Sleiman Marwan Julien Litchinko Alexis Toso Christian Ris Frédéric Delaune Vaihere
Corresponding Author
Sleiman Marwan JulienDivision of Digestive Surgery, Department of Surgery, University Hospital of Geneva, Geneva, Switzerland
Figures & Tables
References
1.
Patoulias D,
Kalogirou M, Patoulias I (2017) Amyand’s hernia: an up-to-date review of the
literature. Acta Medica 60: 131-134. [Crossref]
2.
Akbari K, Wood C,
Hammad A, Middleton S (2014) De Garengeot’s hernia: our experience of three
cases and literature review. BMJ Case Rep 2014: bcr2014205031. [Crossref]
3.
Guenther TM,
Theodorou CM, Grace NL, Rinderknecht TN, Wiedeman JE (2020) De Garengeot
hernia: a systematic review. Surg Endos 35: 503-513. [Crossref]
4.
Jin Z, Imtiaz MR,
Nnajiuba H, Samlalsingh S, Ojo A (2016) de Garengeot’s hernia: two case reports
with correct preoperative identification of the vermiform appendix in the
hernia. Case Rep Surg 2016: 2424657. [Crossref]
5.
Linder S, Linder
G, Mansson C (2019) Treatment of de Garengeot’s hernia:
a meta-analysis. Hernia 23: 131-141. [Crossref]
6.
Rossi SH, Coveney
E (2016) Type 4 appendiceal diverticulum within a de Garengeot hernia. Ann R Coll Surg
Engl
98: e141-e142. [Crossref]
7.
Sibona A, Gollapalli V, Parithivel V, Kannan U (2016)
Case report: de Garengeot’s hernia. Appendicitis within femoral hernia.
Diagnosis and surgical management. Int J Surg Case Rep 27: 162-164. [Crossref]
