A Case of Neurocysticercosis in Diyarbakir
A Case of Neurocysticercosis in Diyarbakir
A B S T R A C T
Neurocysticercosis is a major parasitic disease of the central nervous system, affecting endemic areas worldwide. It spreads through intermediary hosts, pigs and eventually men to his definitive host: humans. It causes lesions in the CNS which have different evolutive stages and can be asymptomatic or clinically evident. Imaging studies play an important role in the diagnosis of the disease and in its appropriate control.
Keywords
Neurocysticercosis, taenia solium, magnetic resonance imaging, paralysis
Introduction
Neurocysticercosis (NCC) is a chronic inflammatory infection of the central nervous system (CNS) caused by the larval form of the tapeworm Taenia solium. The larvae can cause cyst formation in any tissue, including the central nervous system (CNS) [1]. The disease is endemic in many low- and middle-income countries of the world. NCC is a very common disease in Central and South America, Asia, and Africa [2]. Although a few cases have been reported in Turkey. The clinical diagnosis of NCC has been based on the patient history, radiographical findings, and pathological confirmation. Magnetic Resonance (MR) imaging is also valuable for the diagnosis [3]. Here we present a case of NCC identified by MR imaging, which showed multiple lesions compatible with cysticercus.
Case Report
Our case is reported here, occurring in a previously healthy 26-year-old woman, born and residing in Diyarbakir. In November 2017, she was admitted to the Diyarbakir Gazi Yasargil Education and Research Hospital in Diyarbakir. Her complaint is numbness in the left arm for a two months. She had no history of intracranial infectious disease or autoimmune disease. Physical examination revealed no abnormality of her skin and body. Neurological examination revealed mild muscle strength loss of the left arm (4/5). Other muscle strength are 5/5. All blood chemistry findings, including the eosinophil cell count, c-reactive protein and various tests for autoimmune diseases, showed no abnormalities. Culture of her sputum showed no bacterium or tubercle bacillus. Her feces no contained parasite eggs.
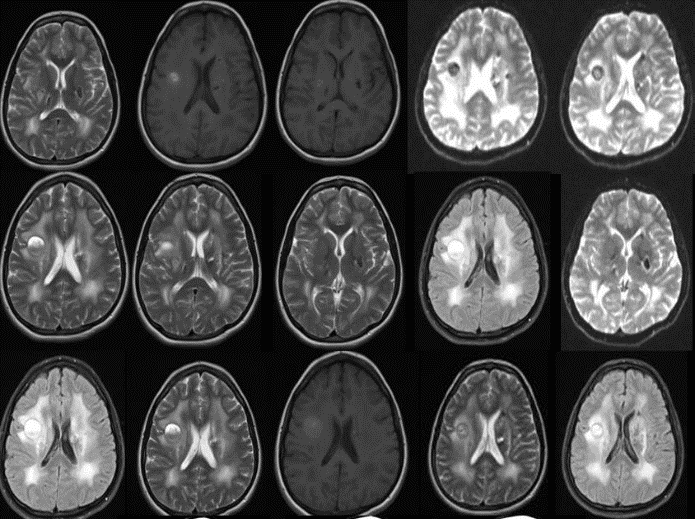
T1-weighted MR imaging revealed an approximately 16 mm diameter hyperintense lesion with circumferential calcification and gadolinium administration T2-weighted MR imaging showed a central focal milimetric contrast containing hyperintense lesion in the right corona radiata. Bilateral centrum semiovale white matter are heterogenic. After gadolinium administration, left centrum semiovale showed a focal contras containing area. Also there is a intense edema around bilateral centrum semiovale. This intense edema spread to the to corona radiata. The contrast magnetic resonance imaging (MRI) showed bilateral basal ganglion calcifications (Figure 1). An electroencephalogram (EEG) was normal. She was started on albendazol (800 mg/day).
Figure 1: MR imaging revealed an approximately 20 mm diameters lesion in the right frontoparietal area and 12 mm diameter lesion in adjacent to the left lateral ventricle.
Discussion
Human NCC is considered a rare disease in Turkey. The diagnosis and treatment of NCC are very difficult in nonendemic regions. Negative serology does not rule out the NSS infection. The imaging of brain lesions is very important for NCC diagnosis [3]. Our case illustrates the difficulty in the diagnosis of NCC in countries where the disease is very rare. Diagnosis requires a reliable medical history, physical examination, knowledgeable medical personnel, brain imaging technology, serological assays, as well as access to medication [4].
In our case, MR imaging with gadolinium showed a parenchymal solitary lesions were compatible with inflammatory disease such as NCC. NCC is a common cause of epilepsy and neurological focal abnormalities. Clinical presentation is related to the cyst localization. Accurate diagnosis is very important. MR imaging is the most accurate diagnostic method [3]. The mainstay for treatment of NCC is albendazole.
Conclusion
The clinical diagnosis of NCC has been based on the patient history, radiographical findings. Magnetic Resonance imaging is valuable for the diagnosis for NCC in non-endemic regions.
Article Info
Article Type
Case ReportPublication history
Received: Fri 09, Aug 2019Accepted: Mon 26, Aug 2019
Published: Thu 05, Sep 2019
Copyright
© 2023 Pinar AYDIN OZTURK. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited. Hosting by Science Repository.DOI: 10.31487/j.SCR.2019.04.09
Author Info
Onder Ozturk Pinar AYDIN OZTURK Unal Ozturk
Corresponding Author
Pinar AYDIN OZTURKDepartment of Neurosurgery, University of Health Sciences, Diyarbakır Gazi Yasargil Education and Research Hospital, Diyarbakir, Turkey
Figures & Tables
References
- Del Brutto OH, Nash TE, White AC Jr, Rajshekhar V, Wilkins PP et al. (2017) Revised diagnostic criteria for neurocysticercosis. J Neurol Sci 372: 202-210. [Crossref]
- Ishikawa E, Komatsu Y, Kikuchi K, Yamasaki H, Kimura H et al. (2007) Neurocysticercosis as solitary parenchymal lesion confirmed by mitochondrial deoxyribonucleic acid sequence analysis. Neurol Med Chir 47: 40-44. [Crossref]
- White AC Jr, Coyle CM, Rajshekhar V, Singh G, Hauser WA et al. (2018) Diagnosis and Treatment of Neurocysticercosis: 2017 Clinical Practice Guidelines by the Infectious Diseases Society of America (IDSA) and the American Society of Tropical Medicine and Hygiene (ASTMH). Am J Trop Med Hyg 98: 945-966. [Crossref]
- Bustos JA, García HH, Del Brutto OH (2007) Reliability of Diagnostic Criteria for Neurocysticercosis for Patients with Ventricular Cystic Lesions or Granulomas: A systematic review. Am J Trop Med Hyg 97: 653-657. [Crossref]
