Pure Embryonal Carcinoma of the Testis Presenting as an Acute Scrotal Swelling
Pure Embryonal Carcinoma of the Testis Presenting as an Acute Scrotal Swelling
A B S T R A C T
We present a case report of a 13-year-old male patient who presented with acute testicular pain and testicular swelling. An urgent ultrasound scan demonstrated a large, irregular, poorly circumscribed, hypervascular right testicular mass. A staging CT scan revealed no distant metastases and an orchidectomy demonstrated a pure embryonal carcinoma of the right testis with lymphovascular invasion.
Keywords
Pure embryonal carcinoma, testicular malignancy, ultrasound testis, doppler ultrasound
Introduction
Pure embryonal carcinoma of the testis is a form of non-seminomatous germ cell tumor. It is a component of 80% of mixed germ cells tumors but in pure form, it comprises only 2-10% of these tumors [1]. The normal age of presentation is between 25-35 years and most patients present with a unilateral enlarging testicular mass; two-thirds of cases have retroperitoneal or distal nodal metastases at the time of presentation [2].
Case Report
A 13-year-old male patient of Spanish origin presented to the emergency department with acute testicular pain and swelling. The patient stated that there had been progressive swelling over the past two weeks. There was no history of trauma and the patient had been afebrile. On examination, the patient had a markedly swollen tender right testicle. Initial blood tests revealed no leucophilia and a normal C Reactive Protein. The patient was reviewed by the surgical team and given the acute presentation, an urgent ultrasound was arranged to assess for a testicular torsion or underlying inflammatory process.
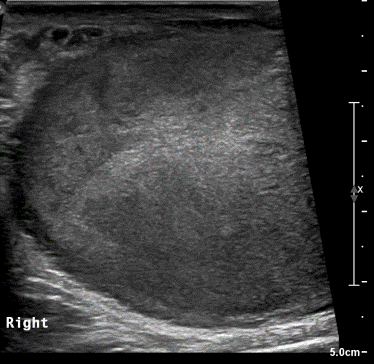
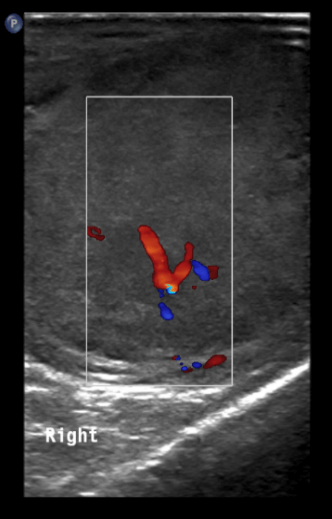
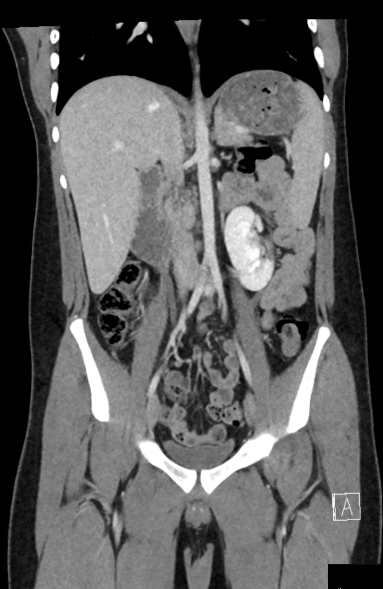
The ultrasound demonstrated a markedly enlarged right testis measuring 40ml in volume. It demonstrated a poorly circumscribed right testicular mass. There was loss of the normal echotexture of the testis, which instead appeared low in echogenicity compared to the normal left testis (Figures 1). There was no extension into paratesticular structures, such as the tunica albuginea or spermatic cord. Increased vascularity was seen within the right testis on colour Doppler imaging, and more visible in the areas of reduced echogenicity (Figures 2). There was no evidence of necrosis, calcification or haemorrhage. These ultrasound findings were strongly suggestive of an underlying malignancy. A staging CT scan of the chest, abdomen and pelvis confirmed no thoracic, abdominal or pelvic metastatic disease (Figure 3).
Figure 1: Gray scale ultrasound image demonstrating an enlarged hypoechoic right testis with loss of the normal echotexture.
Following the ultrasound and CT scan suggesting a local malignancy with no distant metastases, the patient underwent further blood tests, which revealed a raised alpha-fetoprotein of 30 (Normal <6), a raised beta-human chorionic gonadotrophin of 166 (Normal < 2) and a raised lactate dehydrogenase of 665 (Normal < 240). The patient subsequently underwent an orchidectomy which revealed a pure embryonal carcinoma of the right testis with lymphovascular invasion (pT2, N0, M0). The patient was referred for a cycle of post-operative chemotherapy and ongoing surveillance.
Figure 2: Doppler ultrasound image demonstrating increased internal vascularity within the areas of reduced echogenicity present in the right testis.
Figure 3: Coronal CT reformat of the abdomen and pelvis demonstrates no para-aortic lymphadenopathy and no distant metastatic disease. Incidental note is made of a malrotated left kidney.
Discussion
Ultrasound is a first line imaging technique in the evaluation of testicular masses in children. It has a sensitivity of 92% and a specificity of 95% in detecting testicular tumors, however, it cannot reliably be used to predict tumor histology [3]. Other testicular tumors have a different appearance on ultrasound. Testicular mixed germ cell tumors typically demonstrate a partly cystic and partially solid intratesticular mass with increased internal blood flow on ultrasound [3]. Testicular yolk sac tumors are more heterogeneous on ultrasound with significant increased hypervascularity [3]. Testicular teratomas are more complex on ultrasound with cystic components or calcifications and can contain echogenic intra-tumoral fat [4].
This case presented more acutely compared to what has been described in the literature. Ultrasound was useful for the assessment of the mass in the emergency setting. Ultrasound was useful to demonstrate inhomogeneity, reduced echogenicity and diffuse infiltration. These are sonographic features which have been described in the literature for pure embryonal cell carcinoma of the testis. On histology, these lesions commonly demonstrate haemorrhage and necrosis [5]. In cases where there is lymphovascular invasion (LVI), there is a 50% risk of recurrence for LVI-positive patients and 15% for LVI-negative patients. Given the high recurrence rate, patients are offered an orchidectomy followed by a cycle of BEP chemotherapy using bleomycin, etoposide and cisplatin (platinum); this reduces the risk of relapse from 50-2% [6]. The side effects of BEP chemotherapy include cardiovascular disease, infertility, lung disease and renal toxicity [7]. Alternatively, patients can choose to have active surveillance which has a higher relapse rate.
Conclusion
Pure embryonal cell carcinoma is a rare form of non-seminomatous germ cell tumor. Ultrasound is a key tool in the initial acute assessment of testicular pain and swelling, and is a sensitive and specific modality for identifying testicular malignancy, especially in the paediatric population.
Article Info
Article Type
Case ReportPublication history
Received: Wed 15, Jul 2020Accepted: Mon 27, Jul 2020
Published: Thu 06, Aug 2020
Copyright
© 2023 Saira Haque. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited. Hosting by Science Repository.DOI: 10.31487/j.JSCR.2020.04.08
Author Info
Roofia Tanvir Adeel Syed Saira Haque
Corresponding Author
Saira HaqueDepartment of Radiology, Kings College Hospital, Denmark Hill, London, UK
Figures & Tables
References
- Mostofi FK, Sesterhenn IA, Davis CJ Jr (1998) Developments in histopathology of testicular germ cell tumors. Semin Urol 6: 171-188.
- Bahrami A, Ro JY, Ayala AG (2007) An Overview of Testicular Germ Cell Tumors. Arch Pathol Lab Med 131: 1267-1280. [Crossref]
- Moreno CC, Small WC, Camacho JC, Master V, Kokabi N et al. (2015) Testicular tumors: what radiologists need to know–differential diagnosis, staging, and management. Radiographics 35: 400-415. [Crossref]
- Dogra VS, Gottlieb RH, Oka M, Rubens DJ (2003) Sonography of the scrotum. Radiology 227:18-36. [Crossref]
- Ro JY, Amin MB, Sahin AA, Ayala AG (2000) Tumors and tumorous conditions of the male genital tract. In: Fletcher CDM, ed. Diagnostic Histopathology of Tumors. 2nd ed. London, England: Churchill Livingstone 2000: 733-838.
- Chevreau C, Mazerolles C, Soulie M, Gaspard M, Mourey L et al. (2004) Long-term efficacy of two cycles of BEP regimen in high-risk stage I nonseminomatous testicular germ cell tumors with embryonal carcinoma and/or vascular invasion. Eur Urol 46: 209-214. [Crossref]
- Vidal AD, Thalmann GN, Karamitopoulou Diamantis E, Fey MF, Studer UE (2015) Long-term outcome of patients with clinical stage I high-risk nonseminomatous germ-cell tumors 15 years after one adjuvant cycle of bleomycin, etoposide, and cisplatin chemotherapy. Ann Oncol 26: 374-377. [Crossref]
