Omental Infarction: A Review of 3 Cases
A B S T R A C T
Omental infarction is an unusual cause of abdominal pain presenting in both adults and children; though it is rare in both [1, 2]. The difficulty is in the initial diagnosis where it can present in a number of different ways and may mask an underlying surgical condition [3, 4]. Most cases are managed without surgery, however; continuing or worsening pain may push a surgical approach. We present 3 cases of omental infarction, all with characteristic radiological findings. One had accompanying radiological features of acute appendicitis, another continued abdominal pain and the third with symptoms responding well to analgesia. The first and second patients required laparoscopic intervention, while the third was managed conservatively.
Keywords
Omental infarction, conservative management, radiological diagnosis
Background
The acute abdomen is a major presentation in Emergency departments (ED) around the world, with nearly 7-10% of all ED presentations [5]. This makes the awareness of rare causes of abdominal pain very relevant to emergency and surgical diagnosis. The most common presentations in the differential include non-specific abdominal pain, renal colic, biliary colic, appendicitis and diverticulitis [5]. However, a cursory glance at this differential encompasses all parts of the abdomen. Even though the numbers do not in all cases represent a life-threatening cause, it is evident that the frequency of presentation is sufficient for serious conditions to present commonly. The onus, therefore, lies on early and correct diagnosis. Surgeons should also bear in mind, that the co-existence of diagnoses though uncommon, should also be considered.
The mainstay of investigations are biomarkers and radiology. More often than not, the cause of the acute abdomen is clearly identified on radiological investigations, however the role of biomarkers as an adjunct has been dubiously established [6, 7]. But as radiology becomes more common and the safety profile of surgery rises, the demand for definitive management also increases. This also lowers the threshold for surgical intervention in keeping with current guidelines and patient wishes. However, it is clear that though present guidelines are very comprehensive, nearly all cases have a degree of personal tailoring. In cases where the diagnosis is either unclear or uncertain, clinical improvement or lack of; early intervention may be of benefit. In a randomized trial of conservative vs surgical management of acute appendicitis, it was found that 18% of CT labelled uncomplicated appendicitis patients had complicated appendicitis with peritonitis on laparoscopy [8].
There have been a little more than 400 reported cases of omental infarction [9]. The most common presentation has been with right sided abdominal pain which may mimic any right sided pathology including colonic, hepato-biliary or appendiceal pathologies. However, presentation again is not exclusive to the right side [9]. Characteristic CT findings often show a cake-like, high-attenuation fatty mass in keeping with the position of the omentum, near or involving the colon. The more important feature is the presence of an omental inflammatory response greater than the adjacent viscus, often well out of proportion [10]. The mainstay of treatment is conservative non-surgical management as the inflammatory response is sterile and self-limiting. However, surgical intervention may be necessary if the symptoms do not settle or there is concurrent surgical pathology sufficient to warrant it.
Case Presentation
Case 1
A 27-year-old male presented to our ED with complaints of a 1-day history of right sided abdominal pain. The pain had initially been severe, but seemed to have responded to taking paracetamol. There was no shift, migration or radiation. The pain was gradual in onset and involved the right flank and right lower quadrant. There was no association with food intake with no accompanying nausea, other GI symptoms or urinary complaints. There was no recent history of trauma or radiation exposure. He had no previous operations and no underlying medical conditions. He had a BMI of 27, smoked infrequently and drank moderately on weekends only. His father and 2 of his sisters had acute appendicitis requiring surgery at a similar age. On examination he was tender with mild guarding in the right lower quadrant. Rebound and percussive tenderness were also present over McBurney’s point. Murphy’s sign was absent.
Case 2
A 28-year-old female presented to the ED with complaints of pain in the lower abdomen for the past 4 days. Insidious onset but progressively getting worse. At the time of presentation was moderately-severe. Initial site was supra-pubic, but then shifted to the right iliac fossa. There were no accompanying significant GI symptoms, including anorexia and nausea and no history of urinary or gynaecological complaints. The pain responded to analgesia. She had a past history of Stage 1A1 cervical cancer and had received conization surgery in 2016. She had a history of depression. There was no history of radiation treatment or any abdominal surgery. She was nulliparous. She was an active smoker and took Prozac for her depression. She had no known allergies and noncontributory family history. Examination revealed tenderness across the lower abdomen, maximally over the right iliac fossa and the suprapubic region. She had rebound tenderness but no guarding in the right iliac fossa.
Case 3
A 53-year-old male presented to the ED with complaints of pain in the right upper quadrant for the past 3 days. Gradual in onset, it was moderately severe with exacerbation on movement. There were no accompanying gastrointestinal or urinary symptoms. He had no history of gall stones, trauma or exposure to radiation. He had no previous surgeries and his BMI was 29. He was an active smoker with a 25-pack year history. The pain responded well to analgesics. Examination revealed tenderness and guarding in the right upper quadrant with a positive Murphy’s sign. There was no palpable organomegaly.
Investigations
Case 1
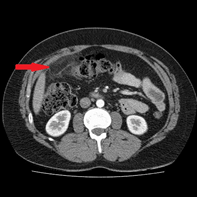
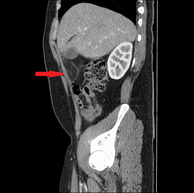
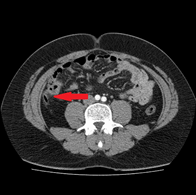
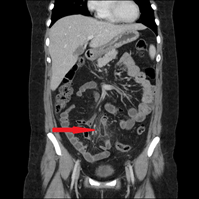
Laboratory results showed a white cell count (WCC) of 9.08 x 103/µl and a CRP of 16mg/L. Other labs results were within normal limits. A urine dipstick and MSU did not reveal any evidence of infection. He underwent an US abdomen which showed no evidence of gall bladder pathology or any free fluid in the abdomen. After his symptoms persisted, he underwent a CT scan which showed mesenteric inflammatory changes in the right upper quadrant. (Figures 1 & 2)There were minor inflammatory changes in the right iliac fossa and the base of the appendix (Figure 3). There was some mild colitic changes in the sigmoid and descending colon as well.
Figure 1: Omental and mesenteric inflammation in right upper quadrant 270 x 270mm (96 x 96 DPI).
Figure 2: Omental and mesenteric inflammation in right upper quadrant 338 x 338mm (96 x 96 DPI).
Figure 3: Inflammation at base of appendix 270 x 270mm (96 x 96 DPI).
Case 2
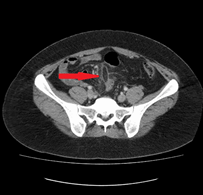
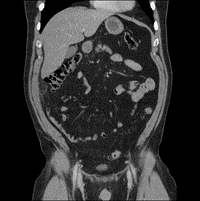
Laboratory results showed a white cell count (WCC) of 10 x 103/µl and a CRP of 10mg/L. Other labs results were within normal limits. A urine dipstick showed trace blood without any white cells. She underwent a CT scan which showed evidence of an omental infarct with inflammatory changes in the lower abdomen towards the center of the mesentery (Figures 4 & 5). There was minimal free fluid in the pelvis. The appendix was identified and was normal.
Figure 4: Omental/mesenteric inflammatory changes in proximity to the sigmoid colon 270 x 270mm (96 x 96 DPI).
Figure 5: Omental and mesenteric inflammatory changes in the lower abdomen 325 x 325mm (96 x 96 DPI).
Case 3
Laboratory results showed a white cell count (WCC) of 10.77 x 103/µl and a CRP of 12mg/L. Other labs results were within normal limits. A urine dipstick did not reveal any evidence of infection. There was no gas under the diaphragm on an erect chest x-ray. He underwent an CT abdomen which showed an omental infarct measuring 2 x 2 cm in the right upper quadrant with characteristic inflammatory changes and no other intra-abdominal pathology (Figures 6 &7).
Figure 6: Omental infarct right upper quadrant 135 x 135mm (96 x 96 DPI).
Figure 7: Omental infarct with minimal surrounding inflammation - coronal view 173 x 173mm (96 x 96 DPI).
Differential Diagnosis
Case 1
Based on the initial history and examination, the differential included acute appendicitis, ascending colitis, pyelonephritis and cholecystitis.
Case 2
Based on the initial history and examination a differential included acute appendiciis, ureteric stone, ovarian cyst or pelvic inflammatory disease.
Case 3
Based on the initial history and examination, the differential included acute cholecystitis, gastritis/duodenitis with possible perforation and atypical appendicitis.
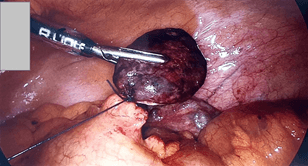
Figure 8: Omental infarction in the right upper quadrant 295 x 167mm (176 x 176 DPI).
Treatment
Case 1
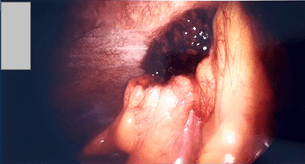
Initial management included analgesia and antibiotics. However, as the symptoms did not appear to settle and the CT findings were equivocal, the patient underwent laparoscopy and was found to have an omental infarct with the infarcted omentum adherent to the peritoneum in the right upper quadrant (Figure 8). This measured approximately 6 x 4cm. There was blood-stained fluid in the subhepatic space of Morrison’s and also in the right iliac fossa. The region of omentum was easily dissected off and resected between endo-loops (Figure 9). The base of the appendix looked injected and an appendicectomy was performed at the same time without complication.
Figure 9: Easily dissected off peritoneum 296 x 162mm (179 x 179 DPI).
Case 2
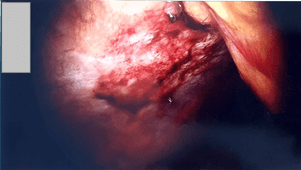
Initial management included analgesia and antibiotics. After the CT findings, she was managed conservatively for 24 hours with analgesia, during which she complained of persistent pain. Her localized examination did not show any change in abdominal signs. After a detailed discussion with the patient, we proceeded with laparoscopy. This revealed a well-defined 3 x 3cm lesion of omental infarct in close proximity to the sigmoid colon, causing minimal localized inflammation of the sigmoid colon. The appendix epiploicae on the bowel were distinctly separate in the same region. This was dissected off easily and resected under a single endo-loop (Figure 10).
Figure 10: Small area of mesenteric infarct in close proximity to sigmoid colon 297 x 162mm (194 x 194 DPI).
Case 3
Initial management included analgesia and anti-biotics to which he responded very well. The pain settled on conservative management.
Outcome and Follow-Up
Case 1
Post-operatively the patient made excellent recovery and was discharged the next day. Follow-up 6 weeks later revealed no issues. Histopathology confirmed infarcted adipose tissue with thrombosed vessels, along with a normal appendix without inflammation.
Case 2
Post-operatively the patient made excellent recovery and was discharged on the first post-op day. Follow-up in 6 weeks revealed no issues. Histopathology confirmed infarcted adipose tissue with thrombosed vessels.
Case 3
He was discharged in next day on continued conservative management. On follow up, his symptoms had subsided completely in a week.
Discussion
Omental infarction is sufficiently rare to not warrant a top-line differential in common ED presentations with acute abdomen, with a ratio of about 4 in 1000 appendicectomies [2, 9]. However, it is an important differential when the biochemical markers are not in keeping with the clinical picture. Tenderness is commonly out of proportion with clinical findings. Accurate CT diagnosis is essential to avoid undue surgery [10].
The greater omentum is a large apron of fat hanging from the greater curvature of the stomach, the transverse colon and other viscera. It is primarily composed of adipose and fibrous tissue, lymph and blood vessels. The understanding of the omentum has undergone a renaissance. In the past, carless omentectomies were carried out, but the unique properties of this ‘abdominal policeman’ are now being used in a variety of surgical techniques [11]. The first case of segmental omental infarction was described by Bush in 1896 [12]. Omental infarction takes place after a portion of the omentum, most commonly rotates along its long axis leading to the classic obstructive sequelae of venous stasis, thrombosis and infarction leading to extravasation of haemorrhagic fluid. Histological evidence is consistent with venous congestion, necrosis of adipose tissue and haemorrhage [13].
In 90% of cases, torsion is on the right-hand side; along the axis of the distal right epiploic artery. This is usually attributed to the fact, that the right side of the omentum is longer and has relatively less attachments as compared to the left side, making it prone to rotational forces [1]. In the 3 cases mentioned above, 2 were on the right-hand side and one was on the left. The exact etiology of omental torsion is not clear, but a number of factors have been considered as predispositions. These include anatomic variations of the omentum, redundant omental veins, obesity leading to excess omental fat, trauma and sudden changes in position, intense exercise and increase in intrabdominal pressures due to coughing and straining [1, 9, 13]. The link between childhood obesity and pediatric primary omental torsion has been well discussed.
Omental infarction can be classified as primary or secondary. Primary omental infarcts are considered to have idiopathic, spontaneous origins. Infarctions resulting from an underlying condition are termed secondary. These include adhesions, hernias, intra-abdominal inflammatory conditions and intra-abdominal neoplasms [9, 10, 13]. This classification was first used in a seminal paper by Anton and Jennings in 1945 [14]. A number of articles use the paper by Leitner et al. in 1952 as a reference, but Leitner et al. defer to the paper by Anton as being the first in the text [15]. It is clear that the etiology of primary omental infarction is relatively independent of secondary occurrences. The role of the descriptive risk factors mentioned here, are more directly related to primary omental infarctions. In all 3 of our cases, interestingly; none were obese, and all were idiopathic and thus primary. There was reported inflammation of the appendix in one case on the CT scan, but the histopathology did not show any inflammation. At the time of presentation, one of the patients had been coming after a relatively active day of cycling; but the rest could not pinpoint a direct attributable instance.
Modern availability of CT scanning and the increasing reliance on early investigations, means that the diagnosis of omental infarction is usually made pre-operatively. In the past, most omental infarcts were found on laparotomy or other open procedures like appendicectomy [2]. CT findings, as mentioned earlier; rely on the pathogenesis of the process, whereby the process takes place within the omentum not the abdominal viscus. Therefore, the inflammatory process which is readily picked up by CT; proportionately involves the omental fat more than any of the adjoining viscera. Often the need for contrast is not necessary, because of intrinsically high contrast from the adipose tissue of the inflamed omentum [10]. Characteristic CT findings like the classical ‘whirl’ sign are not as common, but are thought to arise as a result of CT representation of the rotational nature of omental torsion leading to infarction [2]. US abdomen can be useful as an adjunct to rule out accompanying pathology such as cholecystitis. As mentioned previously, the CT findings of our patients all showed characteristic changes in the omentum, intra-abdominal fat and viscera. One CT showed inflammation of the base of the appendix.
Modern management of omental infarction is now largely conservative [2, 9, 13, 16]. The result of an increase in the availability and improvement in imaging. However, the decision to operate is not infrequent. Vriesman et al. in a paper in 1999, gave their experience of the conservative management of a series of 40 cases of omental infarction, appendagitis epiploica and cases indistinguishable radiologically between the two [17]. They relied solely on radiological findings and in some cases, this lead to the cancellation of planned interventions. All patients were treated only with NSAIDs and analgesics and were followed up to 2 years. All cases had successful resolution of symptoms, most of which were confirmed on radiological findings. However, the in some patients the pain lasted upwards of 4 months. The weakness of this study lies in the fact that there is no burden of surgical or histopathological proof and relied totally on radiological findings. As mentioned before, radiological evidence is not conclusive for the underlying process.
The argument for conservative management lies in the inherently sterile nature of the inflammatory process. However, there have been multiple case reports of surgical intervention [2, 15, 16, 18]. The indication for surgery is usually clinically directed. Progression or persistence of symptoms or clinical deterioration plus the presence of concomitant surgical pathologies are usual indicators of a switch to a surgical approach. There is also a role for laparoscopy in cases of suspected secondary omental infarction [19]. In a series of 30 pediatric patients of omental infarction, McCusker reported an operative approach on 13 patients because of progression or evolution of symptoms and signs [20]. Of these, there was concurrent appendicectomies in 6 patients. None of the specimens was histologically proven to acute appendicitis. However, the physical appearances of these specimens all suggested macroscopic congestion and inflammation. All 30 patients were overweight, and the pre-operative diagnosis of acute appendicitis was substantiated on macroscopic appearance in 60% of cases. The lower pick-up rate was attributed to the fact that signs of acute appendicitis can be nearly indistinguishable from omental infarction in the same region. Other case reports have had similar approaches in adults [21].
Laparoscopy offers a number of advantages including more robust diagnostic data on visualization, quicker diagnosis and pain relief and early discharge from the hospital. This is also reflected in lower hospital costs. However, surgery has its own drawbacks and include an increased risk to life. Nubi et al. in 2009 presented a series of 10 pediatric cases of omental infarction with an attempt at conservative management working in 4. There were 3 first-instance and 3 late-instance laparoscopies [22]. Based on our own experience of the 3 cases mentioned above, the broad recommendation of an initial trial of conservative approach for 24-48 hours seems suitable. If there is progression or persistence of symptoms or the presence of a confounding factor like suspected appendicitis, a laparoscopic approach will provide excellent vision and interventional options for definitive management of omental infarction both primary and secondary.
Learning Points
i. Omental infarction is a rare but confusing diagnosis.
ii. Diagnosis with CT scan is the recommended radiological investigation.
iii. Initial management with analgesia and anti-biotics with in-hospital admission is recommended.
iv. Surgical approach via laparoscopy provides excellent diagnostic and therapeutic possibilities
Intellectual Property Rights Assignment or Licence Statement
I, Naveed Abbas, the Author has the right to grant and does grant on behalf of all authors, an exclusive licence and/or a non-exclusive licence for contributions from authors to permit this work if accepted, to be published.
Funding
None.
Competing Interests
None.
Ethics and Consent
All patients in the study gave signed explicit consent. No ethics approval was required for this study.
Availability of Data and Materials
There is no study related data relevant for declaration.
Patient and Public Involvement Statement
There was no direct involvement of patients or public in the research or reporting of this article.
Article Info
Article Type
Review ArticlePublication history
Received: Mon 05, Oct 2020Accepted: Fri 16, Oct 2020
Published: Mon 26, Oct 2020
Copyright
© 2023 Naveed Abbas. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited. Hosting by Science Repository.DOI: 10.31487/j.AJSCR.2020.04.03
Author Info
Naveed Abbas Salman Ahmed Shahid Kaimkhani
Corresponding Author
Naveed AbbasDepartment of Surgery, Midland Regional Hospital Portlaoise, Surgery
Figures & Tables

References
- Theriot JA, Sayat J, Franco S, Buchino JJ (2003) Childhood obesity: a risk factor for omental torsion. Pediatrics 112: e460. [Crossref]
- Itenberg E, Mariadason J, Khersonsky J, Wallack M (2010) Modern management of omental torsion and omental infarction: a surgeon's perspective. J Surg Educ 67: 44-47. [Crossref]
- Catania VD, di Giacomo V, Bonomo R, Guarino N (2015) Omental infarction in children misdiagnosed as acute appendicitis. Ann Pediatr Surg 11: 200-202.
- Smolilo D, Lewis BC, Yeow M, Watson DI (2015) Omental infarction mimicking cholecystitis. Case Rep Surg 2015: 687584. [Crossref]
- Cervellin G, Mora R, Ticinesi A, Meschi T, Comelli I et al. (2016) Epidemiology and outcomes of acute abdominal pain in a large urban Emergency Department: retrospective analysis of 5,340 cases. Ann Transl Med 4: 362. [Crossref]
- Dias BH, Rozario AP, Olakkengil SA (2015) Role of inflammatory markers as predictors of laparotomy in patients presenting with acute abdomen. ANZ J Surg 85: 755-759. [Crossref]
- Salem TA, Molloy RG, O'Dwyer PJ (2007) Prospective study on the role of C-reactive protein (CRP) in patients with an acute abdomen. Ann R Coll Surg Engl 89: 233-237. [Crossref]
- Vons C, Barry C, Maitre S, Pautrat K, Leconte M et al. (2011) Amoxicillin plus clavulanic acid versus appendicectomy for treatment of acute uncomplicated appendicitis: an open-label, non-inferiority, randomised controlled trial. Lancet 377: 1573-1579. [Crossref]
- Park TU, Oh JH, Chang IT, Lee SJ, Kim SE et al. (2012) Omental infarction: case series and review of the literature. J Emerg Med 42: 149-154. [Crossref]
- Tonerini M, Calcagni F, Lorenzi S, Scalise P, Grigolini A et al. (2015) Omental infarction and its mimics: imaging features of acute abdominal conditions presenting with fat stranding greater than the degree of bowel wall thickening. Emerg Radiol 22: 431-436. [Crossref]
- Liebermann Meffert D (2000) The greater omentum. Anatomy, embryology, and surgical applications. Surg Clin North Am 80: 275-293. [Crossref]
- Bush P (1896) A Case Of HÆMorrhage Into The Great Omentum. Lancet 147: 286.
- McMillen B, Hekman DP, Nguyen MTT, Grewal D (2019) Idiopathic omental infarction: managed conservatively. BMJ Case Rep 12: e226978. [Crossref]
- Anton JI, Jennings JE, Spiegel MB (1945) Primmary omental torsion. Am J Surg 68: 303-317.
- Leitner MJ, Jordan CG, Spinner MH, Reese EC (1952) Torsion, infarction and hemorrhage of the omentum as a cause of acute abdominal distress. Ann Surg 135: 103-110. [Crossref]
- Zaleta Cruz JL, Rojas Mendez J, Garza Serna U, Gonzalez Ruvalcaba R, Ortiz de Elguea Lizarraga J (2017) Omental torsion. Case Report. Cir Cir 85: 49-53. [Crossref]
- van Breda Vriesman AC, Lohle PN, Coerkamp EG, Puylaert JB (1999) Infarction of omentum and epiploic appendage: diagnosis, epidemiology and natural history. Eur Radiol 9: 1886-1892. [Crossref]
- Cianci R, Filippone A, Basilico R, Storto ML (2008) Idiopathic segmental infarction of the greater omentum diagnosed by unenhanced multidetector-row CT and treated successfully by laparoscopy. Emerg Radiol 15: 51-56. [Crossref]
- Abdulaziz A, El Zalabany T, Al Sayed AR, Al Ansari A (2013) Idiopathic omental infarction, diagnosed and managed laparoscopically: a case report. Case Rep Surg 2013: 193546. [Crossref]
- McCusker R, Gent R, Goh DW (2018) Diagnosis and management of omental infarction in children: Our 10 year experience with ultrasound. J Pediatr Surg 53: 1360-1364. [Crossref]
- Danikas D, Theodorou S, Espinel J, Schneider C (2001) Laparoscopic treatment of two patients with omental infarction mimicking acute appendicitis. JSLS 5: 73-75. [Crossref]
- Nubi A, McBride W, Stringel G (2009) Primary omental infarct: conservative vs operative management in the era of ultrasound, computerized tomography, and laparoscopy. J Pediatr Surg 44: 953-956. [Crossref]
