Effect of Remineralizing Agents on Initial Caries Lesions - Clinical Pilot Study on School-Children
A B S T R A C T
Purpose: Enamel remineralization can be improved by increasing salivary calcium and phosphate ion concentration. Dentiplus® lozenges and Remin Pro® -mousse include these components and may have a positive effect on remineralization process. The study investigated if using these additional agents for a month improves dental remineralization compared to tooth brushing using fluoride tooth paste alone.
Methods: Twenty-two patients were included in the final study and all participants had initial caries lesions. They were randomly divided into two test groups (A and B) and a control group. All groups brushed their teeth twice a day with a toothpaste (1500 ppm fluoride). In addition, patients in group A used Dentiplus® -lozenges three times a day and patients in group B used Remin Pro®-mousse once a week. The patients in the control group only brushed their teeth. Lesions were diagnosed by using ICDAS classification, Nyvad’s modified criteria and DIAGNOdent-Pen® scanning.
Results: One third of the lesions in incisors/canines became inactive in both intervention groups, whereas in the control group the respective figure was 15.6%. There was a decrease in LF values in the Dentiplus® group whereas in Remin Pro® group the change was controversial in other except the 1st molar teeth. Both decrease and increase of the LF values was seen in the control group. There were only minor changes as for ICDAS values in this study.
Conclusion: Remineralization of initial lesions by tooth brushing alone can be improved by remineralizing agents especially lozenges rich in calcium and phosphate used regularly. Laser fluorescence is excellent in monitoring change n remineralization with short monitoring periods.
Keywords
Initial lesion, laser fluorescence, DIAGNOdent pen, remineralization, remineralization agent
Introduction
Plaque, dental biofilm containing caries bacteria can cause visible demineralization of the enamel even in couple weeks [1, 2]. Biofilm forms when microbes and their metabolites adhere to dental surface, especially on sites of stagnation such as interproximal and gingival tooth surfaces [3]. In addition to inadequate tooth brushing, fixed and removable orthodontic appliances may cause plaque accumulation; thus, increasing the risk of dental caries [1]. Oral bacteria ferment carbohydrates in their metabolism reducing oral pH and causing mineral loss of the enamel and dentin [3]. The easiest way of disabling the bacteria in oral biofilm from acid formation is by removing it mechanically.
Saliva’s natural buffering capacity (P-ions and H2CO3 –systems) enables remineralization to take place and dental minerals precipitate back on the tooth surfaces. Optimally there is a balance between de- and remineralization on tooth surface. Remineralization or a natural chemical repair process in which biological processes are not involved, occurs when salivary calcium and phosphate recrystallize on the surfaces of existing crystal remnants in enamel and dentin [4]. Remineralization can be improved by increasing salivary calcium and phosphate ion concentration [5]. In recent decades remineralization mousses rich in calcium and phosphate have been introduced (CPP-ACP) and found beneficial on remineralization [1]. Remineralizing lozenges (Dentiplus®; Suomen bioteekki Oy, Raisio, Finland according to patent by Neocare Oy, Finland) contain calcium carbonate, disodium hydrogen phosphate as well as xylitol and and sodium fluoride (0.04 mg/lozenge). Its ingredients help to minimize the period of low pH after meal and improve the remineralization process. Fluoride ions also support the remineralization process as well as reduce demineralization. A new remineralization mousse (Remin Pro® (Voco GmbH, Cuxhaven, Germany) contains hydroxyapatite and fluoride (1500 ppm).
Early diagnosis of dental caries lesions is a corner stone for caries control but is also challenging. Laser fluorescence of dental tissues measured by DIAGNOdent®-pen (KaVo, Biberbach, Germany) can be used to follow the progress of initial caries lesions [6]. Distinct decrease (improvement) in LF values have been demonstrated in patients with initial lesions after regular tooth brushing for only two weeks using fluoride toothpaste (1450 ppm, 5000 ppm) [7]. LF values also correlate with clinical caries status when monitored for a period of one year [8]. According to the literature LF is useful in adjunct with visual detection of caries lesions [8, 9]. The aim of this study was to investigate if using additional remineralization agents, lozenges used many times daily and a mousse used once a week, for one month improves dental remineralization compared to tooth brushing using fluoride tooth paste alone. Our hypothesis was that tooth brushing alone is effective for remineralization of incipient caries lesions presuming that individuals have been taught thorough brushing. Our second hypothesis was that regardless the treatment type remineralization occurs within a month.
Table 1: Distribution of participants into the study and control groups and length of the follow-up period in different groups.
|
Group |
N |
Follow up period (days) |
|
|
Mean |
Sd |
||
|
Dentiplus® |
9 |
38.5 |
12.3 |
|
Remin Pro® |
7 |
30.6 |
15.8 |
|
Control |
6 |
37.2 |
9.8 |
|
Total |
22 |
|
|
Materials and Methods
I Subjects
Research group comprised patients from the Oulu municipal health center (initially n=30; in the end n=22; mean age 13.1 ± 2.2 [SD] years). All participants had initial caries lesions. Many of them (n=13) had either had fixed orthodontic appliances removed recently or were already in retention phase. Patients were randomly divided into two test groups (A, B) and one control group (C) (Table 1) by using a computed randomization. In all groups participants brushed their teeth twice a day with toothpaste (1500 ppm fluoride). Additionally, patients in group A used Dentiplus®-lozenges three times a day (after morning and bedtime tooth brushing and after lunch). Patients in group B used Remin Pro® -mousse once a week and the patients in control group (C) only brushed their teeth. All subjects were personally educated with tooth brushing technique at the first visit and given toothbrushes and toothpastes. Group A was given also Dentiplus®-lozenges and group B Remin Pro®-mousse.
Table 2: Original Nyvad (NY) scores and the corresponding modified scores used in the study.
|
Original NY score |
Modified score |
|
|
0 |
0 |
Sound |
|
1 |
1 |
Active enamel caries, intact surface |
|
4 |
2 |
Inactive enamel caries, intact surface |
|
2 |
3 |
Active enamel caries, surface discontinuity |
|
5 |
4 |
Inactive enamel caries, surface discontinuity |
|
3 |
5 |
Active enamel or dentin caries, cavity |
|
6 |
6 |
Inactive enamel or dentin caries, cavity |
II Clinical Examination
Detection and registering of lesions were carried out by two third-year dental students (K-MP and JN) and an oral hygienist (AT). Lesions were diagnosed visually from the buccal surface of every tooth in oral cavity. To measure lesion depth ICDAS classification was used [1, 5, 6, 8-10]. Nyvad’s modified criteria (Table 2) were used to estimate lesion activity [11]. By DIAGNOdent-Pen® scanning demineralization of the lesions was quantified. The same procedures were carried out by the same person (JN, K-MP, AT) both at baseline and after the follow-up.
The light of the unit and a ball pointed probe were used for the visual-tactile examination. The teeth were professionally cleaned before detection always, when visible plaque was present. The surfaces were air-dried with a three-in-one syringe. The DIAGNOdent-Pen®- device was calibrated every day and individually for each subject on a clean, sound smooth tooth surface according to the manufacturer’s instructions. The ICDAS and Nyvad scores representing the most severe and most active site on the surface as well as the highest DIAGNOdent®-pen scores of each buccal surface were recorded manually on a formulated collection sheet.
The examiners (JN, K-MP, AT) were educated on clinical criteria of ICDAS and the modified Nyvad method by a specialist in cariology and paedodontics experienced in diagnostics (VA). In teaching a Power-Point presentation was used two weeks prior to the first examinations. At the same session they were also educated on the use of the DIAGNOdent Pen® device according to the manufacturer’s instructions. Training of the protocol was practiced in vitro and clinically on three occasions. In calibration sessions findings of extracted teeth on screen were discussed and compared with the findings of the same teeth sectioned. As for laser fluorescence scanning, the training dentist (VA) acted as a golden standard and re-examined some of the patients of each examiner during survey. Kappa values (κ) were calculated to analyze the inter-examiner agreement during the calibration session for ICDAS and Nyvad’s methods and in vivo between the golden standard (VA) and the examiners as for laser fluorescence scanning.
III Statistical Analyses
A change parameter (the value at follow-up minus the baseline value) was calculated for ICDAS and laser fluorescence values. The statistical differences in the mean change parameter within and among groups (Dentiplus®, Remin Pro® and control) were analyzed using a two-level hierarchical ANOVA model with SAS PROC MIXED. The model has two error terms, one measuring the variation between different children and the second representing variation within the same child. Change in activity by Nyvad’s method among groups was analyzed with Fisher’s exact test using SPSS (version 20.0, SPSS, Inc., Chicago, IL, United States).
IV Ethics of the Research
Northern Ostro Bothnia Hospital District’s, Finland Ethical Committee gave a favorable statement for performing this study (§239) 08.12.2011. All analyses were performed without identification of the participants.
Results
Of the original study group (n=30), 22 children participated both examinations (Table 1). In all groups the period between the first and the second visit was at least a month; in the Dentiplus® (A) and control (C) groups the period was even a week longer than in the Remin Pro® group (Table 1). Forty eight permanent 1st molars, 79 premolars and 135 incisors / canines were monitored. The inter-examiner agreement for both ICDAS and Nyvad’s methods was κ = 0.87 in the in vitro calibration session and the in vivo situation for laser fluorescence κ = 0.56.
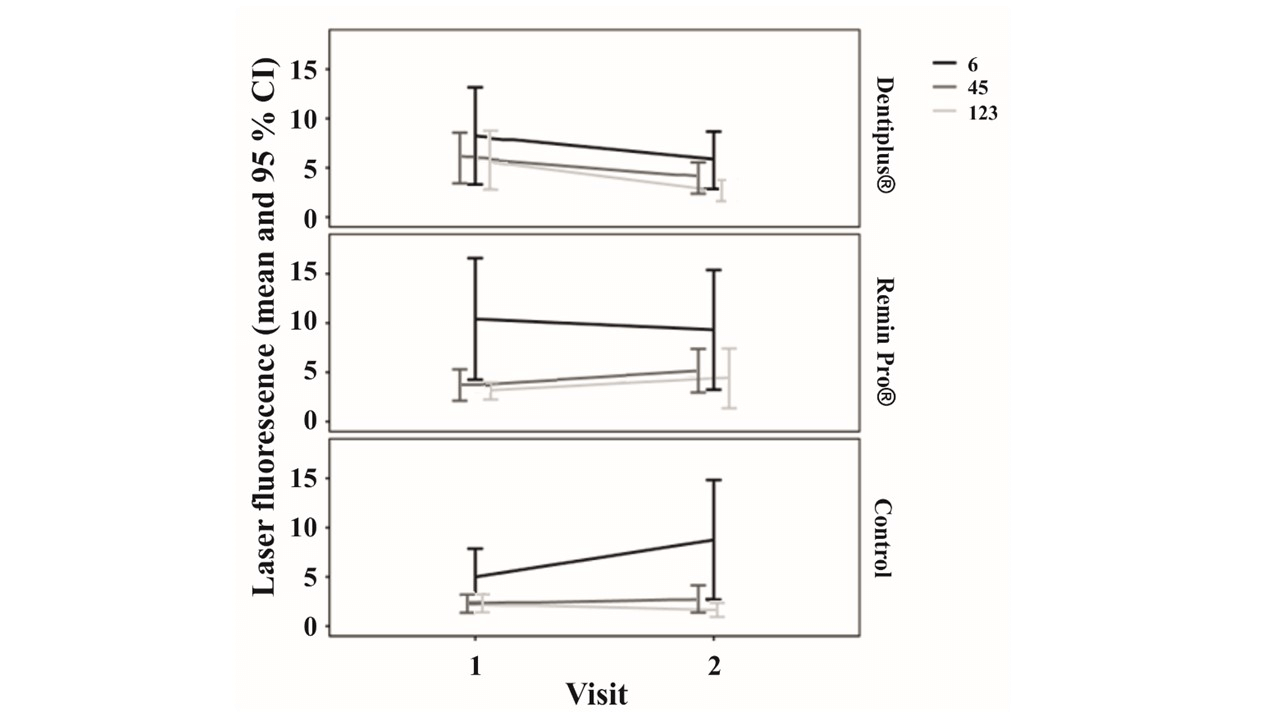
Figure 1: Changes in DIAGNOdent values of incisors/canines (123), premolars (45) and first molars (6) in different groups during the follow-up period.
At baseline the highest mean LF values were measured from the 1st molars. Also, the biggest numerical differences between baseline and end values were measured in them (Table 3). In the Dentiplus® group mean LF values decreased the most; the decrease was -3.88 for the 1st molars, -2.00 for premolars and -3.15 for incisor/canines. In the Remin Pro® group there was also a decrease measured in the 1st molars (-1.25) but premolar (+1.60) and incisor/canine values (+1.52) increased from the baseline. In the control group there was an increase in LF values measured in the 1st molars (+3.62) and premolars (+0.85) but incisor/canine values (-1.45) were reduced from baseline (Table 3). The change in LF values was not statistically significant concerning any teeth in any group (Table 3). The changes in LF values in different groups are illustrated in (Figure 1).
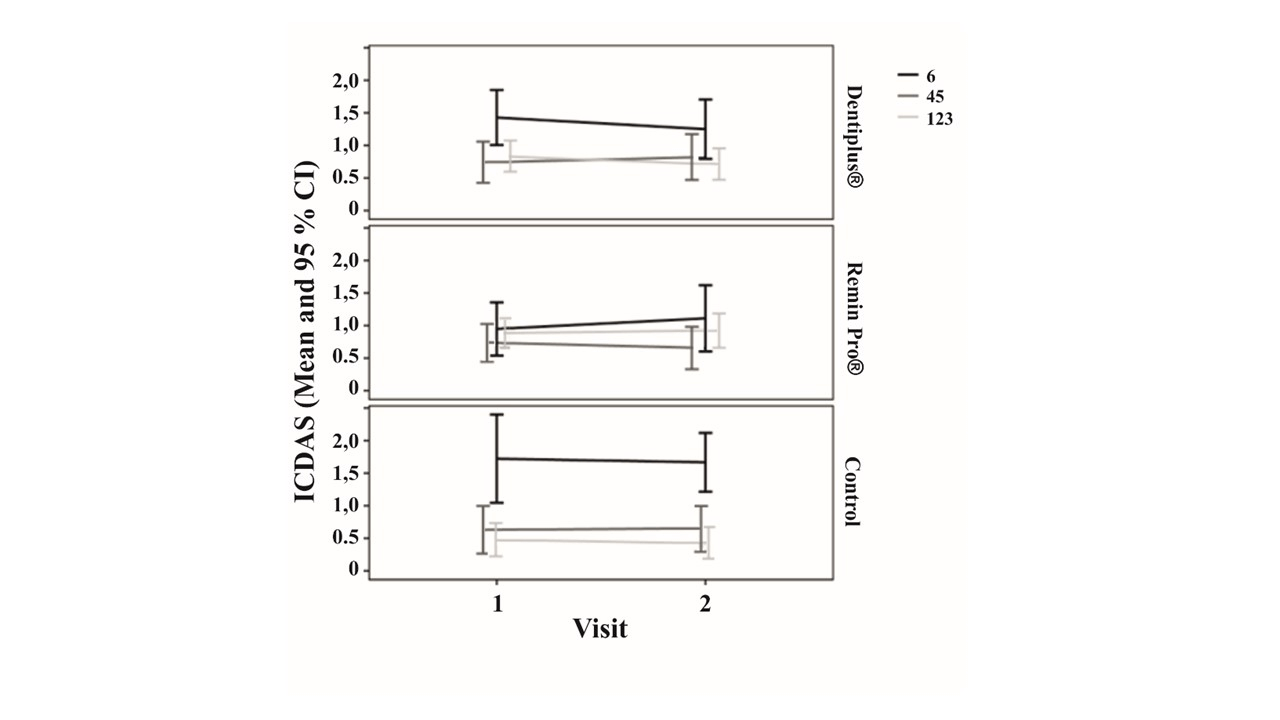
In more than half of the lesions there was no change in activity observed according to the modified Nyvad’s method; in the control group even 4/5 remained unchanged (Table 4). One third of the lesions became inactive in both intervention groups concerning incisors/canines, whereas in the control group the respective figure was 15.6% (Table 4). None of the lesions in the Dentiplus® group turned active, whereas 11.5% of the lesions in Remin Pro® group turned active. Difference between the groups was statistically significant concerning incisors and canines (p=0.011) (Table 4). There were only minor and non-significant changes in ICDAS values. At baseline mean ICDAS values varied between 0.97 and 0.79 including all teeth in all groups. The changes in ICDAS values varied between 0.07-0.09 (Figure 2).
Table 3: Mean DIAGNODent -values at baseline and in the end.
|
Tooth number & group |
n |
LF (SD)
|
p |
p |
|
|
At baseline |
In the end |
||||
|
1st Molars Dentiplus® |
16 |
9.75 (11.95) |
5.87 (5.26) |
0.229 |
0.135 |
|
1st Molars Remin Pro® |
16 |
10.56 (12.36) |
9.31 (11.39) |
0.676 |
|
|
1st Molars Control |
16 |
5.13 (6.10) |
8.75 (11.38) |
0.225 |
|
|
Premolars Dentiplus® |
29 |
5.97 (7.83) |
3.97 (4.16) |
0.253 |
0.108 |
|
Premolars Remin Pro® |
30 |
3.57 (4.36) |
5.17 (5.92) |
0.289 |
|
|
Premolars Control |
20 |
1.95 (2.21) |
2.80 (3.10) |
0.586 |
|
|
Incisors / Canines Dentiplus® |
49 |
5.88 (12.87) |
2.73 (3.88) |
0.341 |
0.364 |
|
Incisors / Canines Remin Pro® |
46 |
2.87 (2.80) |
4.39 (10.21) |
0.329 |
|
|
Incisors / Canines Control |
40 |
2.30 (3.29) |
1.65 (2.21) |
0.559 |
|
Figure 2: Changes in mean ICDAS values of incisors/canines (123), premolars (45) and first molars (6) in different groups during the follow-up period.
Table 4: Change in lesion activity (modified Nyvad’s criteria) concerning incisors and canines.
|
Change in activity |
Intervention group |
Control (%) |
|
|
Dentiplus (%) |
Remin Pro (%) |
||
|
No change |
69.4 |
53.8 |
80 |
|
Active |
0 |
11.5 |
4.4 |
|
Inactive |
30.6 |
34.6 |
15.6 |
|
p |
|
p=0.011 |
|
Discussion
Remineralization occurs in initial lesions regardless of the intervention used – by tooth brushing with or without remineralizing agents which also was our hypothesis. However, there are significant differences in remineralization between tooth types – change of activity is the greatest in incisor-canine regions. This finding is contradictory to what was expected. The best way to measure remineralization is visual-tactile estimation of lesion activity as well as LF scanning.
Lesion activity measured by Nyvad’s criteria indicated significant remineralization of incipient lesions even in weeks in incisors/canines when the participants use daily remineralizing lozenges [2]. Same trend is seen also when weekly remineralizing mousse was used, but less change of activity is seen by tooth brushing only. Additionally, laser fluorescence shows remineralization of the first molars in the groups using extra remineralizing agents, especially daily lozenges, compared to those who only brushed. ICDAS, shows only minor changes during such a short monitoring period and consequently no significant differences between the intervention groups are discovered. Both Nyvad’s method and laser fluorescence scanning seem valid methods for monitoring changes of activity in incipient caries lesions.
The study group here is limited, which is the true short coming in the study. Results can therefore be considered preliminary. RCTs are challenging to conduct and similar size (limited) study groups and follow-up periods have been used in other similar studies [1, 12]. Schirrmeister et al. found significant remineralization of initial lesions in only two weeks [7]. The drop-out rate also caused some bias in the distribution of the participants into different groups. Also, the periods between the baseline and follow-up dental examinations varied. All participants were, however, given similar instructions on homecare. According to our overall positive results, most likely patients followed the instructions even if this was not monitored. To have reliable and generalizable results, studies with larger study populations would be beneficial.
Our findings are partly in concordance with those of Bröchner et al., who used a similar setting in their study [1]. The controls brushed their teeth with fluoride tooth paste but the remineralizing agent used daily by their study group was CPP-ACP. In both groups remineralization of lesions was discovered, but there was no statistally significant difference between the groups. Sitthisettapong et al. also compared effect of tooth brushing with fluoride tooth paste and additional CPP-ACP used topically daily in a year’s follow-up among pre-school children [13]. They found no benefit of the use of CPP-ACP. The remineralizing agents used here (Dentiplus®, Remin Pro®) as well as CPP-ACP all have calcium and phosphate as their main component inducing remineralization.
Both Dentiplus® (0.04 mg/lozenge) and Remin Pro® (1450 ppm) have fluoride; CPP-ACP is also provided with fluoride. Fluoride is most effective when used locally. In the mechanism hydroxyapatite is replaced with fluoroapatite which is formed simultaneously when HA dissolves. The outcome is a decrease in enamel dissolution [5]. Excessive fluoride is stored as CaF2 as reservoir. Dentiplus® has calcium carbonate and xylitol which improve to neutralize the acidic pH in saliva. Even if generalization must be avoided, calcium carbonate and xylitol in Dentiplus® may be the components causing better outcome by its use compared to other methods. CPP-ACP also contains casein which promotes adherence of the active substances on the tooth surface. A recent article on biomimetic hydroxyapatite toothpaste proved to be effective against dental caries in primary teeth (Bossu) [10].
At baseline LF values were the highest in the first molars, which may be explained by their position making cleaning challenging and consequently causing a higher risk for demineralization. Our results support the idea that brushing front teeth is easier than brushing molars. In education tactile sensation of effective brushing should be emphasized but can be out of reach/understanding for children. The impact of remineralization agents was most positive for the molars. It might be helpful to use remineralizing agents at risk ages and times – tooth eruption and orthodontic treatment and times when the roots become exposed. This would need further studies.
Remin Pro® is a topical mousse, which maybe more difficult to use for children. It was also used only once a week, which may not be enough to promote remineralization. It may be easier for children to use a product daily – the use becomes a routine, whereas a product used seldom is easily forgotten. This was not questioned here. This too, may have influenced the outcome in favor of Dentiplus® lozenges used daily. In some cases, the participant’s whole family ended up using Dentiplus® lozenges, which may have motivated the children.
Examiners didn't have much clinical experience of caries diagnostics which could have been a threat for reliable results despite a thorough training, calibration and supervision during the field phase. However, Gimenez et al. have reported that the examiner’s experience does not affect their diagnostic skills [14]. Estimating activity of initial lesions is challenging. Here Nyvad’s descriptive method was used when using ICDAS LAA (ICDAS criteria with quantified lesion activity estimation) could have been easier for third year dental students, but also could have been more time consuming [14] . In vitro the inter-examiner agreement was good. In vivo agreement was quantified for laser fluorescence scanning and it was fair; it must be borne in mind that scanning did not occur in the same situation which might have influenced the outcome.
Orthodontic appliances are considered stagnation sites for biofilm causing risk for dental caries [15]. Therefore, careful oral hygiene instructions should always be given to orthodontic patients. Orthodontic treatment with fixed appliances on patients with high caries risk should also be avoided. Periods of tooth eruption are also considered a times of elevated risk for dental caries due to lazy tooth brushing and dietary habits favoring snacking in addition to erupting teeth being difficult to clean. Fluoride solvents (0.02%) are often used for daily mouth rinsing among orthodontic patients in Finland. Remineralizing lozenges could be another, as effective and practical alternative. Also mousses and even composites containing amorphous calcium phosphate have been used to induce remineralization around brackets [16].
Conclusions
According to our results remineralization of initial lesions by tooth brushing alone can be improved by using remineralizing agents, especially those used daily. This is true for children during and after orthodontic treatment and with active initial lesions on their smooth tooth surfaces. Our second hypothesis was that despite the group, remineralization occurs within a month which was true, yet the process can be strengthened by remineralizing agents. This finding is not in accord with our null hypothesis. However, these agents can be used when lesions are active or the risk for dental caries to develop is obvious. More studies are needed with bigger study groups for investigating the use of remineralizing agents for instance on different types of lesions and on patients with low salivary secretion rate. Laser fluorescence is a good instrument for monitoring short-term changes in mineralization stage.
Author Contributions
VA and LT designed the intervention. VA made the practical arrangements together with AP from the City of Oulu. VA also educated and calibrated the examiners. K-P, JN and AT carried out the examinations. The data were analysed by JN and K-MP supervised by PP and VA. Reporting was done by JN and K-MP supervised by VA and LT.
Acknowledgements
We want to express our gratitude to oral hygienist Anna Turku, who contributed remarkably on the success of this intervention. Also, we want to thank Voco, Finland for contributing the Remin pro® mousse, and Suomen bioteekki, Finland and especially DDS Martti Neva for donating Dentiplus® lozenges free of charge for this intervention.
Conflicts of Interest
None.
Article Info
Article Type
Research ArticlePublication history
Received: Thu 20, Feb 2020Accepted: Wed 04, Mar 2020
Published: Wed 18, Mar 2020
Copyright
© 2023 Vuokko Anttonen. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited. Hosting by Science Repository.DOI: 10.31487/j.CEI.2020.01.09
Author Info
A. Poikela J. Nikkinen K-M. Pasanen L. Tjäderhane M. Neva P. Pesonen Vuokko Anttonen
Corresponding Author
Vuokko AnttonenInstitute of Dentistry, Department of Cariology, Endodontology and Pedodontics, University of Oulu, Oulu, Finland
Figures & Tables
Table 1: Distribution of participants into the study and control groups and length of the follow-up period in different groups.
|
Group |
N |
Follow up period (days) |
|
|
Mean |
Sd |
||
|
Dentiplus® |
9 |
38.5 |
12.3 |
|
Remin Pro® |
7 |
30.6 |
15.8 |
|
Control |
6 |
37.2 |
9.8 |
|
Total |
22 |
|
|
Table 2: Original Nyvad (NY) scores and the corresponding modified scores used in the study.
|
Original NY score |
Modified score |
|
|
0 |
0 |
Sound |
|
1 |
1 |
Active enamel caries, intact surface |
|
4 |
2 |
Inactive enamel caries, intact surface |
|
2 |
3 |
Active enamel caries, surface discontinuity |
|
5 |
4 |
Inactive enamel caries, surface discontinuity |
|
3 |
5 |
Active enamel or dentin caries, cavity |
|
6 |
6 |
Inactive enamel or dentin caries, cavity |
Table 3: Mean DIAGNODent -values at baseline and in the end.
|
Tooth number & group |
n |
LF (SD)
|
p |
p |
|
|
At baseline |
In the end |
||||
|
1st Molars Dentiplus® |
16 |
9.75 (11.95) |
5.87 (5.26) |
0.229 |
0.135 |
|
1st Molars Remin Pro® |
16 |
10.56 (12.36) |
9.31 (11.39) |
0.676 |
|
|
1st Molars Control |
16 |
5.13 (6.10) |
8.75 (11.38) |
0.225 |
|
|
Premolars Dentiplus® |
29 |
5.97 (7.83) |
3.97 (4.16) |
0.253 |
0.108 |
|
Premolars Remin Pro® |
30 |
3.57 (4.36) |
5.17 (5.92) |
0.289 |
|
|
Premolars Control |
20 |
1.95 (2.21) |
2.80 (3.10) |
0.586 |
|
|
Incisors / Canines Dentiplus® |
49 |
5.88 (12.87) |
2.73 (3.88) |
0.341 |
0.364 |
|
Incisors / Canines Remin Pro® |
46 |
2.87 (2.80) |
4.39 (10.21) |
0.329 |
|
|
Incisors / Canines Control |
40 |
2.30 (3.29) |
1.65 (2.21) |
0.559 |
|
Table 4: Change in lesion activity (modified Nyvad’s criteria) concerning incisors and canines.
|
Change in activity |
Intervention group |
Control (%) |
|
|
Dentiplus (%) |
Remin Pro (%) |
||
|
No change |
69.4 |
53.8 |
80 |
|
Active |
0 |
11.5 |
4.4 |
|
Inactive |
30.6 |
34.6 |
15.6 |
|
p |
|
p=0.011 |
|
References
- Bröchner A, Christensen C, Kristensen B, Tranæus S, Karlsson L et al. (2011) Treatment of post-orthodontic white spot lesions with casein phosphopeptide-stabilised amorphous calcium phosphate. Clin Oral Investig 15: 369-373. [Crossref]
- Marsh P D, Nyvad B (2008) The oral microflora and biofilms on teeth. Fejerskov O, Kidd E (eds). Dental Caries, The Disease and Its Clinical Management, 2nd Edition. UK: Wiley-Blackwell 93-95 & 164-85.
- Takahashi N, Nyvad B (2008) Caries ecology revisited: microbial dynamics and the caries process. Caries Res 42: 409-418. [Crossref]
- Featherstone JD (2009) Remineralization, the natural repair process the need for new approaches. Adv Dent Res 21: 4-7. [Crossref]
- Cury JA, Tenuta LM (2009) Enamel remineralization: controlling the caries disease or treating early caries lesions. Braz Oral Res 1: 23-30. [Crossref]
- Aljehani A, Bamzahim M, Yousif MA, Shi XQ (2006) In vivo reliability of an infrared fluorescence method for quantification of carious lesions in orthodontic patients. Oral Health Prev Dent 4: 145-150. [Crossref]
- Schirrmeister J, GebrandeJ, Altenburger M, Mönting J & Hellwig E (2007) Effect of dentifrice containing 5000 ppm fluoride on non-cavitated fissure carious lesions in vivo after two weeks. Am J Dent 20: 212-216. [Crossref]
- Anttonen V, Seppä L, Hausen H (2004) A follow-up study of the use of DIAGNOdent for monitoring fissure caries in children. Community Dent Oral Epidemiol 32: 312-318. [Crossref]
- Angnes V, Angnes G, Batisttella M, Grande RH, Loguercio AD et al. (2005) Clinical effectiveness of laser fluorescence, visual inspection and radiography in the detection of occlusal caries. Caries Res 39: 490-495. [Crossref]
- Bossù M, Saccucci M, Salucci A, Di Giorgio G, Bruni E et al. (2019) Enamel remineralization and repair results of Biomimetic Hydroxyapatite toothpaste on deciduous teeth: an effective option to fluoride toothpaste. J Nanobiotechnol 17: 17. [Crossref]
- Nyvad B, Machiulskiene V, Baelum V (1999) Reliability of a new caries diagnostic system differentiating between active and inactive caries lesions. Caries Res 33: 252-260. [Crossref]
- Ferrazzano GF, Amato I, Cantile T, Sangianantoni G, Ingenito A (2011) In vivo remineralising effect of GC tooth mousse on early dental enamel lesions: SEM analysis. Int Dent J 61: 210-216. [Crossref]
- Sitthisettapong T, Phantumvanit P, Huebner C, Derouen T (2012) Effect of CPP-ACP paste on dental caries in primary teeth: a randomized trial. J Dent Res 91: 847-852. [Crossref]
- Gimenez T, Bittar DG, Piovesan C, Guglielmi CA, Fujimoto KY (2013) Influence of examiner experience on clinical performance of visual inspection in detecting and assessing the activity status of caries lesions. Oper Dent 38: 583-590. [Crossref]
- Opsahl Vital S, Haignere-Rubinsteinc C, Lasfarguesc JJ Chaussainc C (2010) Caries risk and orthodontic treatment. Int Orthod 8: 28-45. [Crossref]
- Uysal T, Amasyali M, Koyuturk AE, Ozcan S (2010) Effects of different topical agents on enamel demineralization around orthodontic brackets: an in vivo and in vitro study. Aust Dent J 55: 268-274. [Crossref]
