A Prospective Study on Odontogenic Tumors Among Patients Attending Muhimbili National Hospital, Dar Es Salaam, Tanzania
A B S T R A C T
Introduction: Odontogenic tumors which may be benign or malignant, constitute a group of heterogeneous lesions that are derived from the tooth-producing tissues or their remnants that are entrapped either within the jawbones or into the adjacent soft tissues. Aim of the study was to determine the pattern of occurrence and clinicopathological presentation of odontogenic tumors among patients attending the oral and maxillofacial unit at Muhimbili National Hospital (MNH), Dar es Salaam, Tanzania using 2005 WHO classification.
Material and Methods: This was a cross-sectional hospital-based study that included patients with oral and maxillofacial tumors. Patients’ information was gathered using a structured questionnaire. Clinical and histological examination was done, and the findings were recorded in a specially designed form. Data was processed and analyzed using Statistical Package for Social Sciences (SPSS) version 19.
Results: A total of 102 patients with histological diagnosis of odontogenic tumors comprising 52 (51%) males and 50 (49%) females, were included in this study. The mean age of the patients was 34.07 ± 14.8 SD years and the most affected age group was 20-29 years. Majority 76 (74.5%) of the patients had odontogenic tumors comprised of odontogenic epithelium with mature fibrous stroma without odontogenic ectomesenchyme. Ameloblastoma was the most (65.7%) common odontogenic tumor followed by odontogenic myxoma/myxofibroma (5.9%) and Keratocystic Odontogenic Tumor (5.9%).
Conclusion: Generally, the sociodemographic distribution and frequency of occurrence, of odontogenic tumors seen in this study is similar to that reported in other African and Asian studies but differed with American and European studies. Ameloblastoma was the most common odontogenic tumor with a high propensity for the mandible compared to the maxilla.
Keywords
Odontogenic tumors, occurrence, Tanzania
Introduction
Odontogenic tumors and tumor-like lesions constitute a group of heterogeneous diseases that range from hamartomatous (tumor-like malformations) or non-neoplastic tissue proliferation to benign and malignant tumors [1]. They are derived from epithelial, ectomesenchymal and/or mesenchymal elements of the tooth-forming apparatus. The occurrence of the odontogenic tumors and tumor-like lesions vary from one country to the other. In Tanzania, they were reported to comprise about 12% of all tumors of the orofacial region [2] and elsewhere in Africa, they accounted for 10% to 14% of all orofacial tumors [3, 4]. Their prevalence was less than 5% in Brazil, China and Pakistan [5-7]. In Iran however, a prevalence of about 26% was reported [8]. In Tanzania, ameloblastoma was documented to be the most (73.7%) common odontogenic tumor followed by odontogenic myxoma (10.3%) [2]. Similarly, in Kenya, ameloblastoma was the most (45.9%) common followed by the keratocystic odontogenic tumor (KOT) with 11.2% [3]. While in India odontoma was reported as the most (56%) common odontogenic tumor followed by ameloblastoma (14%), in China KOT was the most (38.73%) frequent benign tumor followed by ameloblastoma (36.52%) [6, 9].
Although odontogenic tumors are derived from tooth-producing tissues or their remnants that are entrapped either within the jawbones or into the adjacent soft tissues, their etiology is unknown [10]. Majority, however, seem to arise de novo, without an apparent causative factor and histologically, tend to resemble the tissue of origin [1, 7]. Clinically, benign odontogenic tumors have an insidious onset and grow slowly [7]. These tumors are usually painless, do not metastasize and are not life-threatening unless they interfere with vital organs by direct extension. Benign tumors are usually detected clinically by expansion of the jaws or are found incidentally during a radiographic examination. On the contrary, malignant tumors represent an uncontrolled growth of tissue and unlike benign neoplasms, they are more locally invasive, have a greater degree of anaplasia, and can metastasize [1].
Previous studies on odontogenic tumors and tumor like lesions in Tanzania used the older WHO classifications of odontogenic tumors (either the 1971 or 1992) [2, 11]. In the classification of odontogenic tumors that was developed by WHO in 2005, there was a re-categorization of some of these tumors and therefore there was a need to make another audit based on this new classification.
The aim of this study was to determine the pattern of occurrence and clinicopathological presentation of odontogenic tumors among patients attending the oral and maxillofacial unit at MNH, Dar es Salaam, Tanzania using 2005 WHO classification.
Material and Methods
This was a descriptive prospective hospital-based study conducted at the oral and maxillofacial surgery unit of Muhimbili National Hospital, Dar es salaam, Tanzania for one year in 2014/2015. MNH is the biggest referral hospital in Tanzania with the only fully functioning oral and maxillofacial unit and therefore receives patients from all over the country. All patients who presented for treatment in the oral and maxillofacial unit of MNH with a histological diagnosis of odontogenic tumors were included in the study after consenting. Patients who were diagnosed with odontogenic tumors but did not give consent were excluded. Refusal to enroll or withdrawal from the study did not in any way affect the patient’s right to receive treatment as per the existing Muhimbili National Hospital protocol.
A structured questionnaire was used to gather patients’ information. The information included demographics, chief complaint, duration of the lesion, presenting symptoms and previous treatments. Clinical and histopathological presentation of the lesions were recorded in predesigned clinical forms. The 2005 WHO classification of odontogenic tumors was used for histological categorization of the tumors. The data obtained was entered in the computer and was processed and analyzed using version 19 of Statistical Package for Social Sciences (SPSS). Frequency distribution to describe the sociodemographic characteristics, occurrence and clinicopathological characteristics of the study population was generated. Ethical clearance was granted by the Research and Publications Committee of the Muhimbili University of Health and Allied Sciences (MUHAS). The information was kept confidential by giving numbers of identification instead of using the names of participants in both the questionnaires and clinical forms.
Results
A total of 102 patients with a histological diagnosis of odontogenic tumors were included in this study. The study group consisted of 52 (51%) males and 50 (49%) females, with a male to female ratio of almost 1:1. The age range was 8 to 68 years with a mean age of 34.07 and SD ± 14.8 years. The age group 20-29 years was the commonest (35.3%) affected and in general patients aged 40 years and below accounted for 68.6% (Table 1). Out of the 102 patients, 76 (74.5%) had odontogenic tumors comprised of odontogenic epithelium with mature fibrous stroma without odontogenic ectomesenchyme. Ten (9.8%) patients had odontogenic tumors of mesenchyme and/or odontogenic ectomesenchyme with or without odontogenic epithelium. Nine patients (8.8%) had odontogenic carcinomas while 7 (6.9%) patients had tumors of odontogenic epithelium origin with odontogenic ectomesenchyme with or without hard tissue formation.
Table 1: Distribution of patients by age group and gender.
|
Age group |
Gender of the patient |
Total |
|
|||
|
Male |
Female |
|
||||
|
|
0-9 |
1 |
0 |
1 |
||
|
10-19 |
9 |
6 |
15 |
|||
|
20-29 |
14 |
22 |
36 |
|||
|
30-39 |
12 |
6 |
18 |
|||
|
40-49 |
4 |
4 |
8 |
|||
|
50-59 |
8 |
11 |
19 |
|||
|
60-69 |
4 |
1 |
5 |
|||
|
Total |
52 |
50 |
102 |
|
||
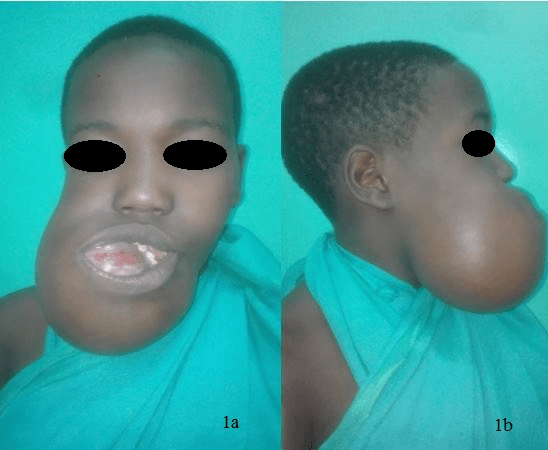
Figure 1: Mandibular ameloblastoma in a rather young healthy person. a) frontal view and b) lateral view.
Ameloblastoma was the most frequent diagnosis accounting for 67 (65.7%) cases, followed by odontogenic myxoma/myxofibroma and KOT each accounting for 6 (5.9%) cases. Others included odontogenic fibroma, ameloblastic fibrodentinoma, metastasizing (malignant) ameloblastoma and ameloblastic carcinoma (Table 2). Of the 67 cases of ameloblastoma, there were 36 (53.7%) males and 31 (46.3%) females making an almost equal sexual distribution (male to female ratio of 1.2:1). The peak age group for ameloblastomas was 20-29 years and females outnumbered males in this peak age group. All except one (1.5%) intrabony ameloblastomas were located in the mandible (Figure 1) and there were 5 (7.5%) extraosseous/peripheral (soft tissue) ameloblastoma. Of the mandibular ameloblastomas, 37.5% were extending from the right ramus to the midline, followed by those which were located on the symphyseal area (23.2%) (Figure 2).
Table 2: Different odontogenic tumors encountered.
|
TUMOR |
FREQUENCY |
PERCENTAGE |
|
Ameloblastoma New cases Recurrences |
67 57 10 |
65.6 |
|
Odontogenic myxoma/myxofibroma |
6 |
5.9 |
|
Keratocystic odontogenic tumor (KOT) |
6 |
5.9 |
|
Odontogenic fibroma |
4 |
3.9 |
|
Ameloblastic fibrodentinoma |
3 |
2.9 |
|
Metastasizing (malignant) ameloblastoma |
3 |
2.9 |
|
Ameloblastic carcinoma |
3 |
2.9 |
|
Primary intraosseous sq cell ca |
2 |
2.0 |
|
Ameloblastic fibroma |
2 |
2.0 |
|
Clear cell tumor |
1 |
1.0 |
|
Sq odontogenic tumor |
1 |
1.0 |
|
CEOT |
1 |
1.0 |
|
Adenomatoid odontogenic tumor |
1 |
1.0 |
|
Odontoma-complex type |
1 |
1.0 |
|
Calcifying cystic odontogenic tumor |
1 |
1.0 |
|
TOTAL |
102 |
100 |
Table 3: Combined age and gender with frequency of occurrence of ameloblastomas.
|
Type of Ameloblastoma |
Age group |
|||||||||||||||
|
0-9 |
10-19 |
20-29 |
30-39 |
40-49 |
50-59 |
60-69 |
Total |
|||||||||
|
M |
F |
M |
F |
M |
F |
M |
F |
M |
F |
M |
F |
M |
F |
|||
|
|
Solid/multicystic |
- |
- |
4 |
2 |
8 |
10 |
4 |
2 |
2 |
1 |
4 |
3 |
2 |
- |
42 |
|
Unicystic |
1 |
- |
1 |
- |
1 |
7 |
3 |
- |
- |
1 |
0 |
1 |
1 |
- |
16 |
|
|
Extraosseous/peripheral |
- |
- |
- |
- |
2 |
- |
1 |
1 |
- |
- |
- |
1 |
- |
- |
5 |
|
|
Desmoplastic |
- |
- |
- |
1 |
- |
- |
1 |
- |
- |
- |
1 |
1 |
- |
- |
4 |
|
Figure 2: Locations of the 61 mandibular ameloblastomas. A) Tumor extending from right condyle to left condyle (3.6%); B) Tumor extending from the right ramus to the midline (37.5%); C) Tumor localized in the right ramus (8.9%); D) Tumor extending from the right ramus crossing the midline to involve the body on the left side (1.8%); E) Tumor occupying the symphysial region only (23.2%); F) Tumor extending from left ramus to the midline (19.6%); G) Tumor localized in the left ramus (5.4%).
Forty-two ameloblastomas (62.7%) were of solid/multicystic type, 16 (23.9%) of unicystic type, 5 (7.5%) were extraosseous/peripheral type, and 4 (6%) desmoplastic type (Table 3). The various histological subtypes/pattern of solid/multicystic ameloblastomas are shown in (Figure 3). Recurrent ameloblastomas were found in 10 (14.9%) patients who had been surgically treated previously. Their previous histological diagnoses were reviewed and compared to the recurrent tumor histology. Both the previous and current tumor histologies were similar (Figure 4).
Regarding odontogenic myxoma, there were 4 male and 2 female patients. Two patients were in the age group 30-39 years; the other two patients were in the age group 20-29 years, and the remaining two belonged to the age groups of 10-19 and 40-49 years respectively. Odontogenic myxomas were equally distributed in the maxilla and mandible (i.e. three each). Also, 6 patients were diagnosed with KOT, of which four (66%) were females. Three (50%) patients were in the age group of 10-19 years and 5 of these lesions were located in the mandible.
Figure 3: Distribution of the histological pattern of solid ameloblastoma.
Figure 4: Histopathological images (H& E) of granular cell ameloblastoma showing hypercellularity with scanty stroma with central areas of granular cells with large, eosinophilic cytoplasmic granules. (magnification x40).
Discussion
This study assessed the situation of odontogenic tumors in the Tanzanian population using the WHO (2005) classification. The last published report on odontogenic tumors in Tanzania fifteen years ago used the 1992 WHO classification of odontogenic tumors [11]. One of the drawbacks inherent in this study was that some few patients who initially reported to hospital with clinically suspected odontogenic tumors could not report back on appointed days for biopsy and further clinical evaluation. hence were dropped from the study. The outcome, however, should be as close to the true situation as possible given the fact that all patients with oral and maxillofacial tumors in the whole country are referred to our unit which is the only oral and maxillofacial center in the country.
Most (76%) of the patients were below 50 years of age and nearly half (48%) were between 10 and 29 years with a mean age of 34 years, which is in concurrence with several other studies elsewhere [7, 12-17]. The findings of this study, however, contradict what was reported in Nigeria and India where the mean age was found to be 29.9 years and 25 years respectively [4, 18]. Unlike in some studies which reported a slight male preponderance and others which reported a female predilection, in this study, there was an equal sex predilection in the occurrence of odontogenic tumors which is in agreement with several other studies [4, 7, 12-18].
The fact that our study found out that 94.1% of patients had intraosseous odontogenic tumors and 5.9% of patients had peripheral/extraosseous odontogenic tumors correlate with the findings from Nigeria [4]. The high distribution of odontogenic tumors in the intraosseous location can be explained by the fact that odontogenic tumors are derived from epithelial, ectomesenchymal and/or mesenchymal elements of the tooth-forming apparatus which are located in the jawbones and tend to histologically resemble the tissue of origin [1, 7]. Of the intraosseous odontogenic tumors, 90.6% were located in the mandible and 9.4% were located in the maxilla, a ratio of 9.7:1. This was similar to many other studies which also reported the odontogenic tumors to be more frequently located in the mandible [4, 7, 12]. Slightly over 93% of the tumors were benign while only 6.9% were malignant. These findings are comparable to reports in the literature [4, 6, 8, 12]. A rather higher frequency of malignant odontogenic tumors was reported in a study from Pakistan which showed that benign odontogenic tumors constituted 78.8% while 21.3% were malignant [7].
In this study while ameloblastoma comprised majority (65.6%) of the odontogenic tumors it was slightly below the findings by Simon et al. (2005) in which ameloblastoma constituted 80.1% of all odontogenic tumors [11]. Ameloblastoma has also been reported to be the most common odontogenic tumor in several other studies from other countries [2-4, 8].
In the previous study by Simon et al. (2005) which used the WHO (1992) classification the KOT was not reported because it was not yet classified as a tumor but rather a cyst and hence it was omitted [11]. In the present study, the KOT together with odontogenic myxoma, were the second commonest occurring tumors. Two other studies have reported KOT as the second most common odontogenic tumor [3, 12]. Our findings differ from other studies that reported KOTs or the odontomas as the commonest odontogenic tumors [6, 7, 9, 12]. In the developed world, odontomas are the commonest occurring lesions because most patients attend routine checkups which allows these tumors which are usually symptomless to be incidentally diagnosed. This is not the case in developing countries where patients commonly stay with lesions until they develop a certain degree of incapacitation before they consider seeking medical help.
In this study, the solid/multicystic type of ameloblastoma was the commonest type of ameloblastoma. This was in agreement with several other studies [14, 19, 20]. Follicular ameloblastoma was the most (55.2%) common histological type, followed by the mixed (14.9%) and the plexiform (13.4%) subtypes. This is in agreement with several other previous studies from Tanzania and elsewhere [2, 15, 16, 19, 21]. In Brazil, however, the plexiform type was reported to be the most common histological subtype and an equal number of follicular and plexiform histological patterns was reported in the Netherlands [14, 20]. Only one (1.5%) ameloblastoma was located in the maxilla and 5 (7.5%) were extraosseous/peripheral ameloblastomas in the soft tissues. This is in concurrence with several other studies [2, 14, 17, 19]. So far it remains an enigma why ameloblastomas have an extremely high affinity for the mandible compared to the maxilla.
Of the mandibular ameloblastomas, 37.5% were extending from the right ramus to the midline, followed by those which were located on the symphyseal area (23.2%). Two studies reported that the left ramus to the midline was the most common mandibular site of ameloblastomas followed by the symphyseal area [2, 14]. Many other studies reported the posterior mandible as the most common site for ameloblastoma [14-17,19-21]. Location and extension of ameloblastoma lesions have implications on the treatment plan of the patient and on the postsurgical morbidity and quality of life of the patient. In situations where the symphysis is involved and segmental resection has to be done, detachment of the central muscles is inevitable, which greatly affects function and aesthetics unless reconstruction is done.
Although the odontogenic myxoma was the second most common odontogenic tumor in our study, there were only six encountered cases. This concurs with the previous studies which also showed that this lesion has a low frequency in Tanzania [11, 22]. Contrary to a previous report from Tanzania in which there was a female predominance and odontogenic myxomas were mainly located in the mandible, in this study males were predominant and there was an equal distribution of these tumors in both jawbones [22]. Nevertheless, the findings of this study showed similarity with the previous studies in the age groups of patients with odontogenic myxoma.
Conclusion
Generally, the sociodemographic distribution and frequency of occurrence, of odontogenic tumors seen in this study was similar to other African and Asian studies but differed with American and European studies. Ameloblastoma was the most common odontogenic tumor with a high propensity for the mandible compared to the maxilla.
Recommendations
i. There is a great need for raising awareness of the society for early reporting and health personnel at primary health facilities for making early detection and appropriate referrals.
ii. Strengthening the regional hospitals and referral centers to enable them to make accurate diagnosis would alleviate the problems of patients who have to travel long distances to get the required medical help.
Ethics Approval and Consent to Participate
The study was conducted in compliance with Good Clinical Practices and in accordance with the “Declaration of Helsinki.” Ethical clearance to conduct this study was granted by the Research and Publications Ethical Committee of the Muhimbili University of Health and Allied Sciences (MUHAS). Written informed consents for participation in the clinical study were obtained for all participants. For the child patients, written informed consents for participation was obtained from their parents/guardians.
Acknowledgment
We are most grateful to the patients for availing all the necessary information that was required for the study.
Availability of Data and Materials
The complete data and materials described in this study are freely available from the corresponding author on reasonable request.
Author Contributions
The authors have contributed equally to this work by making substantial contributions to the conception and design, acquisition of data, and analysis and interpretation of data as well as being involved in drafting of the manuscript or revising it critically for important intellectual content. All authors read and approved the final manuscript.
Funding
None.
Competing Interests
None.
Article Info
Article Type
Research ArticlePublication history
Received: Sat 25, Apr 2020Accepted: Wed 27, May 2020
Published: Wed 10, Jun 2020
Copyright
© 2023 Karpal Singh Sohal. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited. Hosting by Science Repository.DOI: 10.31487/j.ORD.2020.01.02
Author Info
Elison NM Simon Karpal Singh Sohal Samwel Mwalutambi Sira Stanslaus Owibingire
Corresponding Author
Karpal Singh SohalDepartment of Oral and Maxillofacial Surgery, Muhimbili University of Health and Allied Sciences, Dar es Salaam, Tanzania
Figures & Tables
Table 1: Distribution of patients by age group and gender.
|
Age group |
Gender of the patient |
Total |
|
|||
|
Male |
Female |
|
||||
|
|
0-9 |
1 |
0 |
1 |
||
|
10-19 |
9 |
6 |
15 |
|||
|
20-29 |
14 |
22 |
36 |
|||
|
30-39 |
12 |
6 |
18 |
|||
|
40-49 |
4 |
4 |
8 |
|||
|
50-59 |
8 |
11 |
19 |
|||
|
60-69 |
4 |
1 |
5 |
|||
|
Total |
52 |
50 |
102 |
|
||
Table 2: Different odontogenic tumors encountered.
|
TUMOR |
FREQUENCY |
PERCENTAGE |
|
Ameloblastoma New cases Recurrences |
67 57 10 |
65.6 |
|
Odontogenic myxoma/myxofibroma |
6 |
5.9 |
|
Keratocystic odontogenic tumor (KOT) |
6 |
5.9 |
|
Odontogenic fibroma |
4 |
3.9 |
|
Ameloblastic fibrodentinoma |
3 |
2.9 |
|
Metastasizing (malignant) ameloblastoma |
3 |
2.9 |
|
Ameloblastic carcinoma |
3 |
2.9 |
|
Primary intraosseous sq cell ca |
2 |
2.0 |
|
Ameloblastic fibroma |
2 |
2.0 |
|
Clear cell tumor |
1 |
1.0 |
|
Sq odontogenic tumor |
1 |
1.0 |
|
CEOT |
1 |
1.0 |
|
Adenomatoid odontogenic tumor |
1 |
1.0 |
|
Odontoma-complex type |
1 |
1.0 |
|
Calcifying cystic odontogenic tumor |
1 |
1.0 |
|
TOTAL |
102 |
100 |
Table 3: Combined age and gender with frequency of occurrence of ameloblastomas.
|
Type of Ameloblastoma |
Age group |
|||||||||||||||
|
0-9 |
10-19 |
20-29 |
30-39 |
40-49 |
50-59 |
60-69 |
Total |
|||||||||
|
M |
F |
M |
F |
M |
F |
M |
F |
M |
F |
M |
F |
M |
F |
|||
|
|
Solid/multicystic |
- |
- |
4 |
2 |
8 |
10 |
4 |
2 |
2 |
1 |
4 |
3 |
2 |
- |
42 |
|
Unicystic |
1 |
- |
1 |
- |
1 |
7 |
3 |
- |
- |
1 |
0 |
1 |
1 |
- |
16 |
|
|
Extraosseous/peripheral |
- |
- |
- |
- |
2 |
- |
1 |
1 |
- |
- |
- |
1 |
- |
- |
5 |
|
|
Desmoplastic |
- |
- |
- |
1 |
- |
- |
1 |
- |
- |
- |
1 |
1 |
- |
- |
4 |
|



References
- Philipsen HP, Reichart PA (2006) Classification of Odontogenic Tumours. A Historical Review. J Oral Pathol Med 35: 525-529. [Crossref]
- Simon ENM, Stoelinga PJW, Vuhahula E, Ngassapa D (2002) Odontogenic Tumours and Tumour-Like Lesions in Tanzania. East Afr Med J 79: 3-7. [Crossref]
- Butt FMA, Ogeng’O J, Bahra J, Chindia ML (2011) Pattern of Odontogenic and Nonodontogenic Cysts. J Craniofac Surg 22: 2160-2162. [Crossref]
- Ladeinde AL, Ajayi OF, Ogunlewe MO, Adeyemo WL, Arotiba GT et al. (2005) Odontogenic Tumors: A Review of 319 Cases in a Nigerian Teaching Hospital. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 99: 191-195. [Crossref]
- Avelar RL, Antunes AA, de Santana Santos T, de Souza Andrade ES, Dourado E (2008) Odontogenic Tumors: Clinical and Pathology Study of 238 Cases. Braz J Otorhinolaryngol 74: 668-673. [Crossref]
- Luo HY, Li TJ (2009) Odontogenic Tumors: A Study of 1309 Cases in a Chinese Population. Oral Oncol 45: 706-711. [Crossref]
- Akram S, Ali MA, Shakir MM (2013) Prevalence of Odontogenic Cysts and Tumors in Karachi, Pakistan. J Dow Uni Heal Sci 7: 20-24.
- Taghavi N, Rajabi M, Mehrdad L, Sajjadi S (2013) A 10-year Retrospective Study on Odontogenic Tumors in Iran. Indian J Dent Res 24: 220-224. [Crossref]
- Ebenezer V, Ramalingam B (2010) A Cross-Sectional Survey of Prevalence of Odontogenic Tumors. J Maxillofac Oral Surg 9: 369-374. [Crossref]
- Taylor AM (2008) New Findings and Controversies in Odontogenic Tumors. Med Oral Patol Oral Cir Bucal 13: E555-E558. [Crossref]
- Simon ENM, Merkx MAW, Vuhahula E, Ngassapa D, Stoelinga PJW (2005) A 4-year Prospective Study on Epidemiology and Clinicopathological Presentation of Odontogenic Tumors in Tanzania. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 99: 598-602. [Crossref]
- Çizmeci Şenel F, Dayisoylu EH, Ersöz Ş, Yilmaz Altintaş N, Tosun E et al. (2012) The relative frequency of odontogenic tumors in the Black Sea region of Turkey: An analysis of 86 cases. Turkish J Med Sci 42: 1463-1470.
- Saghravanian N, Jafarzadeh H, Bashardoost N, Pahlavan N, Shirinbak I (2010) Odontogenic Tumors in an Iranian Population: A 30-year Evaluation. J Oral Sci 52: 391-396. [Crossref]
- Fregnani ER, da Cruz Perez DE, de Almeida OP, Kowalski LP, Soares FA et al. (2010) Clinicopathological Study and Treatment Outcomes of 121 Cases of Ameloblastomas. Int J Oral Maxillofac Surg 39: 145-149. [Crossref]
- Ladeinde AL, Ogunlewe MO, Bamgbose BO, Adeyemo WL, Ajayi OF et al. (2006) Ameloblastoma: Analysis of 207 Cases in a Nigerian Teaching Hospital. Quintessence Int 37: 69-74. [Crossref]
- Butt FMA, Guthua SW, Awange DA, Dimba EAO, Macigo FG (2012) The Pattern and Occurrence of Ameloblastoma in Adolescents Treated at a University Teaching Hospital, in Kenya: A 13-year Study. J Cranio-Maxillofacial Surg 40: e39-e45. [Crossref]
- Varkhede A, Tupkari JV, Mandale MS, Sardar M (2010) Odontogenic tumors: A review of 60 cases. J Clin Exp Dent 2: 2-6.
- Mullapudi SV, Putcha UK, Boindala S (2011) Odontogenic Tumors and Giant Cell Lesions of Jaws--A Nine Year Study. World J Surg Oncol 9: 68. [Crossref]
- Zhang J, Gu Z, Jiang L, Zhao J, Tian M et al. (2010) Ameloblastoma in Children and Adolescents. Br J Oral Maxillofac Surg 48: 549-554. [Crossref]
- Hertog D, Bloemena E, Aartman IHA, van der Waal I (2012) Histopathology of Ameloblastoma of the Jaws; Some Critical Observations Based on a 40 Years Single Institution Experience. Med Oral Patol Oral Cir Bucal 17: e76-e82. [Crossref]
- Adebayo ET, Ajike SO, Adekeye EO (2005) A Review of 318 Odontogenic Tumors in Kaduna, Nigeria. J Oral Maxillofac Surg 63: 811-819. [Crossref]
- Simon ENM, Merkx MAW, Vuhahula E, Ngassapa D, Stoelinga PJW (2004) Odontogenic Myxoma: A Clinicopathological Study of 33 Cases. Int J Oral Maxillofac Surg 33: 333-337. [Crossref]
