Complex Spinal Dorso-Ventral Stabilization in the Elderly – Is Age a Limiting Factor? Retrospective Case Series of 53 patients
A B S T R A C T
Objective: Medical progress is increasingly confronting us with the question of whether complex surgical spinal care can be performed safely, even in older patients. This study is intended to contribute to the clarification of this question.
Methods: 53 patients with a minimum age of 70 years at time of surgery were retrospectively enrolled in a single center setting. All patients were treated with complex dorsoventral instrumentation and corpectomy due to different pathologies. Because of neurological deficits and untreatable pain, no control group of patients could be defined in advanced age by withholding necessary surgery. The ethical committee would not accept this.
Results: Most patients benefited from the procedure with regard to pain (97%), sensori-motor deficit (89%), and finally, immobility (82%). The duration of surgery, the amount of transfused red blood cell concentrates, and the length of hospital stay were not predictors of a poor overall outcome. It was shown that the risk of postoperative complications increased due to the number of preoperative secondary diagnoses.
Conclusion: Therefore, not the patients’ age alone is of prime importance for individual surgical treatment decisions, but the number of secondary diagnoses plays a more important role. Especially in that older population, patients benefit from surgical therapy; regardless, it could be complex.
Keywords
Corpectomy, elderly patient, surgery, multimorbidity, secondary diagnoses
Introduction
Demographic change in developed countries is progressing steadily. The proportion of the population more than 65 years of age is growing by the achievements of medical care and resulting in increased life expectancy. In Germany, the part of this age population increased from 14.9% in 1990 to 21% in 2014 with a supposed part of 30% in 2030 [1]. This inevitably leads more frequently to the question of whether complex surgical spinal care is appropriate for advanced age as the risks of complications could rise [2]. Unfortunately, current literature offers limited answers to this question. Some studies report on small patient series with a significant younger average of age who were treated more frequently in a unilateral way and in fewer cases by dorso-ventral stabilization [3-6].
The population of ageing patients poses a particular challenge from a surgical point of view, as patho-physiological changes progress with increasing age and the number of secondary diagnoses rise. Pronounced osteoporosis with or without trauma, progressive degeneration of the spinal anatomy, tumor including spinal metastasis, and infection like spondylodiscitis may negatively influence the stability of the spinal column. Permanent anticoagulation also represents an intraoperative risk that should not only be underestimated because of actual blood loss but also because of decreased cardiovascular function and consecutive reduced cardiac reserve capacity. During the postoperative course, the cerebral and cardiopulmonary disease might determine the duration of ventilation and the beginning of the patient’s mobilization, leading to further complications if delayed. But all in all, the functional reserve of the human system is lower in elderly patients than in younger ones [7, 8]. In elective surgery, elderly patients might reach similar postoperative results than younger patients [9]. Extreme stress during emergency surgery leads to worse postoperative results, but which is often better than the conservative way of treatment in the presence of instability and/or neurological deficit [10].
In relation to the before-mentioned conditions, we would like to contribute with this study to the decision making on complex surgical spinal care in patients of advanced age. Because of neurological deficits and/or untreatable pain, no control group of patients could be defined in advanced age by withholding necessary surgery. The ethical committee of our hospital would not accept this.
Methods
Inclusion criteria for this retrospective case series were complex dorso-ventral instrumentation with corpectomy and a minimum patient age of 70 years at the time of surgery, ensuring only patients of advanced age were enrolled. Surgical spinal care was defined as complex when dorso-ventral instrumentation with corpectomy was performed. Indications for complex spinal stabilization were instability so far due to traumatic and pathological fractures (e.g., advanced osteoporosis or extensive metastases) and advanced degenerative pathologies with clinically relevant spondylolisthesis. Destructive infections, such as spondylodiscitis and spinal metastasis, were also the indicators for complex instrumentation.
The first surgical step was a dorsal fixation by massae laterales (cervical spine) or pedicle screws (thoracolumbar spine) above and below the intended corpectomy. Cement augmentation was performed with pronounced osteoporosis and low intraoperative bony resistance when screws were placed. In a second step, corpectomy was performed depending on the spinal section by retropharyngeal/ventral (cervical spine), transthoracic (thoracic spine), or retroperitoneal (lumbar spine) approach. The surgical level of the spinal column (cervical, thoracic or lumbar spine), the pure surgical time (incision/suture time), the surgical mode (single-stage vs. two-stage dorso-ventral instrumentation), the postoperative length of in-hospital stay, and the amount of transfused red blood cell concentrates (RBCs) during in-patient postoperative course were recorded.
In addition, preoperative secondary diagnoses of patients, as well as postoperative change of prior existing clinical deficits, were recorded. Focused on the development of the clinical course in relation to preoperative status, we established a simple score system consisting of 0: worse, 1: equal, and 2: improved. Furthermore, postoperative general and surgical complications and development of Nurick score up to a follow-up period of one year were evaluated. Nurick score classifies the severity of myelopathy on the basis of walking ability on a scale of 0 to 5 points. The higher the point value, the more pronounced the myelopathy, i.e., 5 points: immobility with bed rest or wheelchair requirement, 0 points no impairment of gait pattern – even if symptoms can be present [11].
Statistical analysis was performed using IBM SPSS Statistics [12]. Chi-square testing, according to Pearson, was applied to check the significant correlation between corpectomy level and mortality rate. Spearman-Rho calculation was used to control a significant correlation between the number of existing preoperative secondary diagnoses and the number of postoperative non-surgical complications. Significance was defined as a p-value < 0,05.
Results
In accordance with inclusion criteria, a total of 53 patients in this case series with complex dorso-ventral spinal stabilization could retrospectively be included from 2010 to 2016. A complete overview of relevant patient data is presented in (Table 1).
Table 1: Demographic overview of the entire study cohort, including patients’ main parameters, indication of surgery, level of corpectomy, and type of complications.
|
Items |
Parameters |
Values |
|
|
|
|
|
patients |
inclusion period (years) |
6,5 (01.01.2010-30.06.2016) |
|
|
|
|
|
|
total collective |
n = 53 |
|
|
|
|
|
|
sex (♀ : ♂) |
31 : 22 |
|
|
|
|
|
|
age at surgery* (years) |
75 (70-89) |
|
|
|
|
|
|
type of secondary diagnosis† |
cardiovascular (CHD, hypertension, arrhythmia) metabolic (DM Type 2) neurological (c. a. ischaemia / hemorrhage) neoplastic (malign) medicamentous (anticoagulation) nephrological (renal insufficiency) haematological (anaemia, factor diseases) endocrinological (thyroid dysfunction) pulmonary (COPD, bronchial asthma, OSA) rheumatoid (arthritis, M. Bechterew, arteritis) |
n = 38 n = 9 n = 10 n = 21 n = 21 n = 7 n = 7 n = 8 n = 7 n = 5 |
number of secondary diagnoses per patient‡ |
0 1 2 3 4 5 6 |
n = 0 n = 6 n = 13 n = 19 n = 7 n = 2 n = 1 |
|
operation |
indication† |
fractures traumatic pathologically (osteoporosis) pathologically (metastasis) infections (spondylodiscitis) degeneration (spondylolisthesis) |
n = 3 n = 15 n = 14 n = 8 n = 13 |
|
|
|
|
|
level of corpectomy§
|
cervical spine thoracic spine lumbar spine |
n = 18 n = 23 n = 14 |
|
|
|
|
|
mode |
single-stage two-stage |
n = 33 n = 20 |
|
|
|
|
|
duration (minutes)* |
475 (241-1057) |
|
|
|
|
|
perioperative |
transfusions (RBC)* |
2 (0-17) |
|
|
|
|
|
|
In-patient stay (days)*, II |
18 (7-98) |
|
|
|
|
|
postoperative |
type of complications (general) |
wound healing disorder nosocomial urinary tract infection pneumonia sepsis organ failure (kidney, liver) myocardial infarction resuscitation pleural effusion pulmonary embolism respiratory insufficiency tracheotomy (long-term ventilation) delirium cerebral (hydrocephalus, meningitis, SH) |
n = 11 n = 5 n = 11 n = 5 n = 9 n = 1 n = 5 n = 27 n = 3 n = 5 n = 7 n = 8 n = 2 |
number of complications per patient‡ |
0 1 2 3 4 5 6 |
n = 13 n = 13 n = 7 n = 7 n = 9 n = 3 n = 1 |
|
|
complications (implant-referred) ¶
|
none screw dislocation in need of revision conservative cage dislocation in need of revision conservative |
n = 37 n = 6 n = 8 n = 2 n = 1 |
|
|
|
|
|
deaths |
n = 4 |
|
|
|
|
*corresponds to: median (range), †preoperative situation, ‡median values bold marked, §two patients each operated at 2 spinal levels, IIno statement about destination after discharge/transfer, ¶one patient with screw and cage dislocation in need of revision. c. a.: condition after, CHD: coronary heart disease, COPD: chronic obstructive pulmonary disease, DM: Diabetes mellitus, M: Morbus, OSA: obstructive sleep apnea, RBC: red blood cell concentrate, SH: subdural hematoma.
Advanced age at time of operation was noticeable which showed a median age of 75 years (range 70 - 89). 38 patients had a cardiovascular secondary diagnosis like chronic heart disease, hypertension or arrhythmia. 19 patients revealed up to 3 secondary diagnoses per patient, e.g. neoplastic, need of anticoagulation, diabetes type 2 or cardiovascular (Table 1). Fractures of different causes like traumatic (n=3), pathological because of osteoporosis (n=15) or metastasis (n=14) or rather instability of spinal vertebra as a result of infections (spondylodiscitis) and degeneration (spondylolisthesis) were a main indication for stabilization surgery.
The most frequent surgically involved area was the thoracic spine in 43% of cases (n=23). In median, two complications per patient occurred (Table 1). Most common general complication was pleural effusion (51%, n=27), followed by wound healing disorders (21%, n=11) and pneumonia (21%, n=11). Postoperative complication referred to implants and 15% (n=8) patients were needed to be revised for the better positioning due to screw or cage dislocation.
Spearman-Rho calculation showed a significant correlation between the number of preoperative secondary diagnoses and the number of postoperative non-surgical complications (p=0.001). The positive correlation coefficient (0.447) showed a positive relation to these two characteristics. Thus, postoperative complications were more frequent, the more preoperative secondary diagnoses were present.
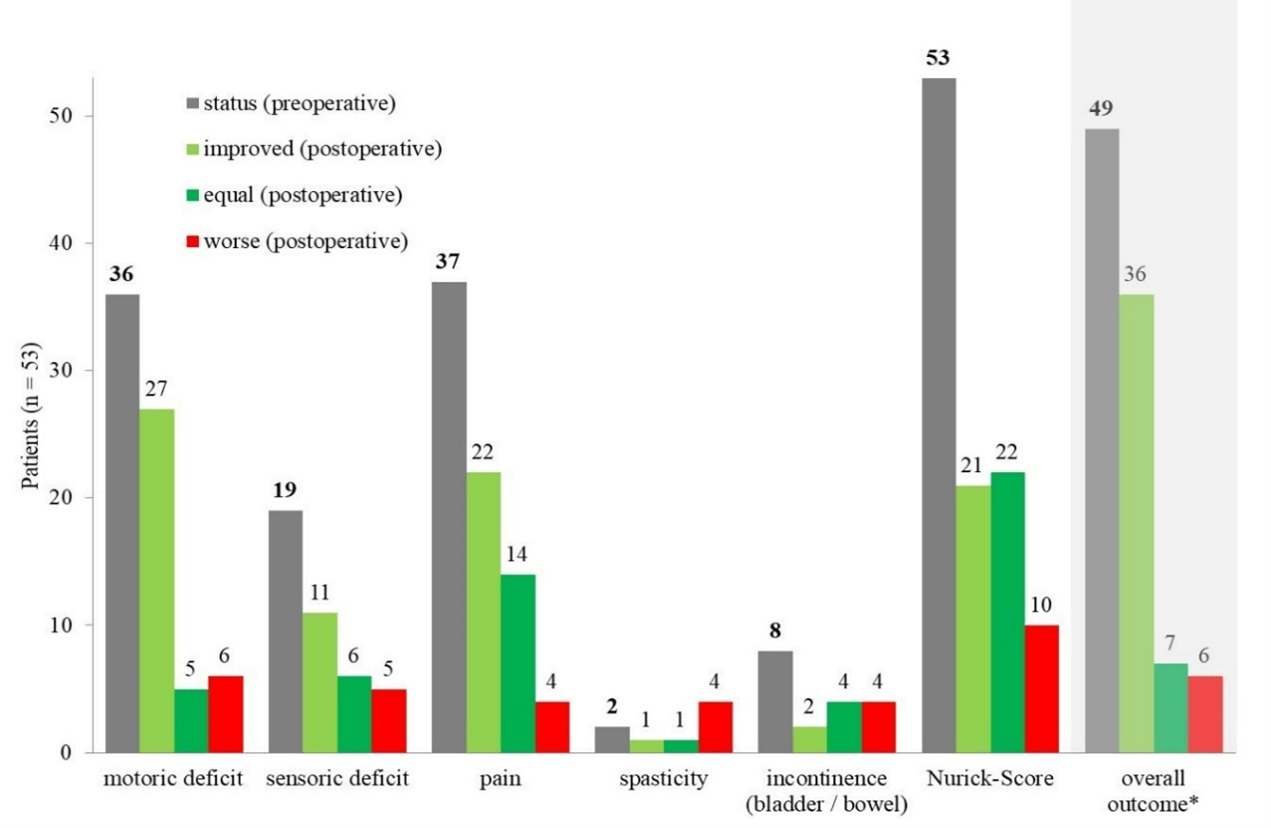
A total of four patients (8%) died during the in-patient stay because of multiorgan failure (n=2), respiratory insufficiency, and after the end of life-support treatment in persistent coma. Chi-square test, according to Pearson showed no significant correlation between corpectomy level and mortality rate (p=0.284). Figure 1 shows that preoperative pain and sensoric and motoric deficits were the most common symptoms. Postoperatively, the majority of patients (n=43) improved or at least, the progression of symptoms could be stopped. Exceptions to this were spasticity and incontinence, which showed no relevant improvement postoperatively (Figures 1 & 2).
Figure 1: Pre- and postoperative clinical status of patients included. *4 deceased patients excluded, total follow-up time up to one year (correlated to clinical status & Nurick score per patient).
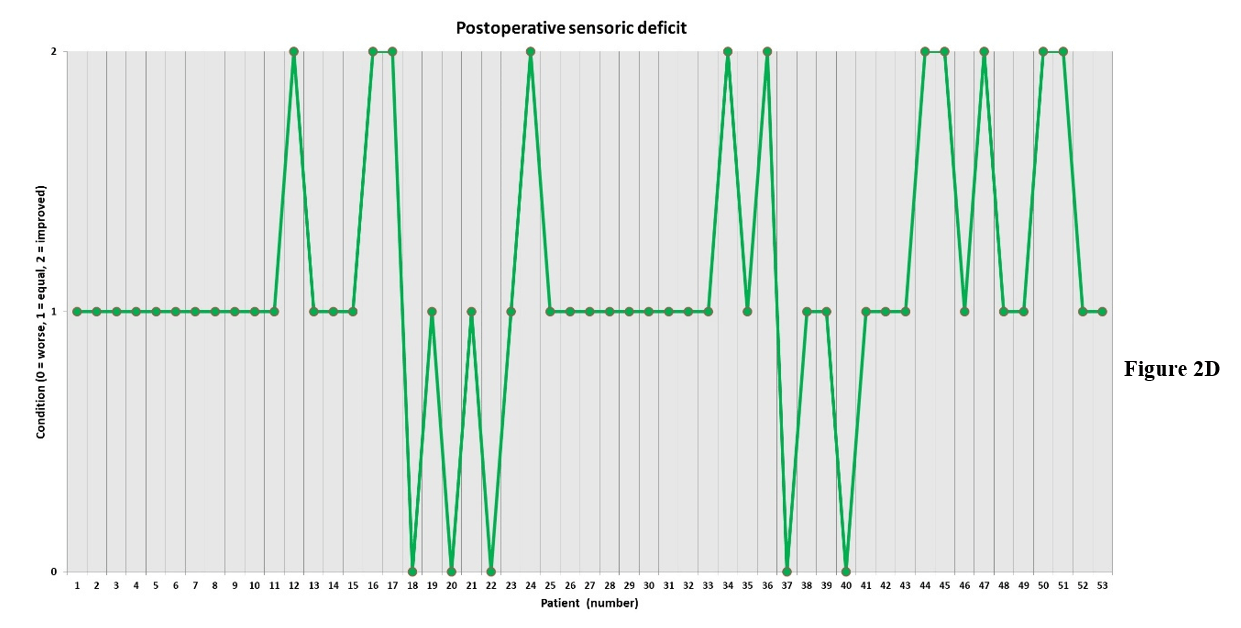
Figure 2: A-D) Postoperative patients’ neurological status; 0: worse, 1: equal, 2: improved.
Nurick score illustrates that 40% (n=21) of patients benefited from surgical therapy concerning mobility. Stabilization and no further deterioration of clinical symptoms was achieved in 42% (n=22). Apart from the four deceased patients, only 11% (n=6) showed a worse outcome. The overall outcome in correlation to Nurick score revealed a clear postoperative increase in mobility and a reduction of symptoms in 73% of patients (n=36). In 14% of all cases (n=7), stabilization of the symptoms could be provided (Figure 1).
The most frequent surgical mode was the single-stage procedure (62%, n=33). Median surgery time per patient was 475 minutes (range 241-1057), in median two RBCs (range 0-17) were transfused perioperatively. In median, after 18 days (range 7-98), an in-patient transfer or discharge from the hospital was performed (Table 1). Concerning the categories, the extent of the range was striking, which could be explained by extreme and torn values of only five patients. Nevertheless, stabilization or improvement in overall outcome could be achieved in all of these patients.
The most remarkable patient had an operation time of 870 minutes, 14 RBCs were admitted because of anticoagulant medication and hospital stay lasted 98 days – this patient improved in overall outcome. Two patients showed different operation length of 1057 and 987 minutes; the patient with longer surgery time also received the maximum of 17 RBCs. This patient showed an unchanged overall outcome – the second patient clinically improved. The last two patients had an in-patient transfer or discharge after 80 and 97 days, respectively. The patient with shorter in-patient stay improved in overall outcome – the other patient remained unchanged.
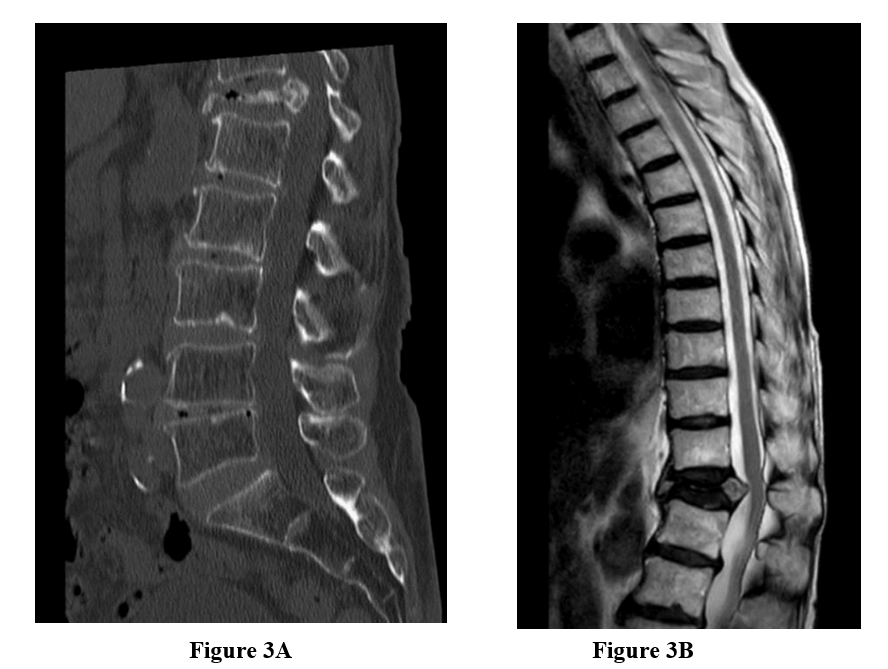
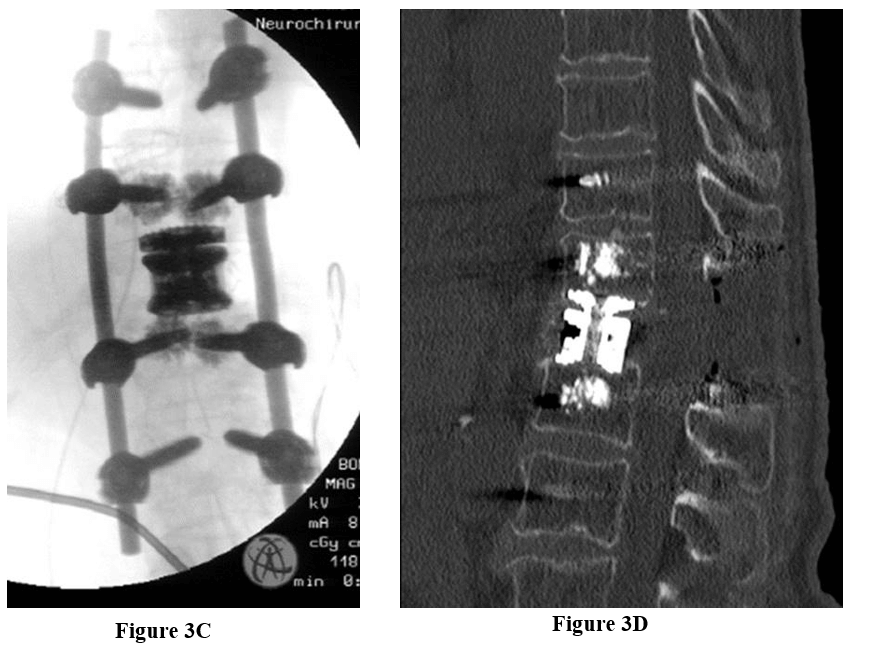
Figure 3: A) & B) Female patient suffering from immobilizing pain and pathological fracture because of osteoporosis in vertebra T12. MRI and CT scan showed an unstable fracture with the participation of dorsal vertebra wall and compression of the spinal cord. C & D) Dorso-ventral stabilization with corpectomy of T12, including cage insertion and screw placement from level T10-L2.
Discussion
Various factors depend on the autonomy of the elderly population, e.g., participation in life or comorbidity in case of immobility [13, 14]. Furthermore, reduction of the need for long-term care or its delay to a later point in time might make sense from an economic point of view and, depending on the health system of the respective country, might play a differently crucial role.
Complex spinal dorso-ventral stabilization aims to restore stability of the spinal column and to improve associated symptoms or to prevent deterioration, at least (Figure 3). According to the overall outcome, the before-mentioned results were achieved in 87% of patients (n=43) (Figure 1). It is remarkable that these patients with advanced age (75 years median at time of surgery) showed a benefit in comparison to their supposed alternative course without surgery (Table 1).
There is no consensus in literature as to when a person may be regarded as "old". The range of data reaches from 60 to 75 years of age [15, 16]. The median age in our study was 75 years - and in 26% of patients even more than 80 years – therefore, patients of our study are considered to be old. Furthermore, literature does not provide a common indication for the term multimorbidity to be used; depending on the individual working group, this condition is often supposed to start from two to three secondary diagnoses [17-19]. Our case series showed in 79% of patients (n=42), two secondary diagnoses and in 55% of patients (n=29), even three secondary diagnoses per individual person, so in consequence, the majority of these elderly patients can be regarded as multimorbid.
In addition, the risk of developing general postoperative complications, such as urinary tract infection or delirium, appears to be increased up to 1.96-fold from the age of 60 [2]. Statistically, this study showed that the more preoperative secondary diagnoses were present, the higher the postoperative general complication rate was. After surgery, general complications of varying severity occurred, ranging from mild nosocomial urinary tract infection to severe pulmonary embolism, resuscitation, or sepsis. The most common complication, pleural effusion, occurred in 51% (n=27) of patients because 42% (n=22) of patients were treated by transthoracic approach. However, this clinical “sign” was to be expected due to surgical approach and did not represent a strict part of postoperative complication. Even though there was an increased risk of general postoperative complication, 25% (n=13) of patients were without any complication after complex spinal surgery. Another 25% (n=13) of patients had only one complication – mostly the expected pleural effusion due to the transthoracic approach. Therefore, almost half of patients did not experience an unexpected general complication during postoperative course, whereas 75% (n=40) of patients generally had one general postoperative complication, at least (Table 1).
Since postoperative complications have not been standardized in literature in relation to complex spinal surgery, no consensus has been described, and comparisons remain difficult. Literature references on complication rates range from 14.8 to 43.6%, whereby only complications which were directly related to surgery were mentioned, e.g., wound healing disorders and pleural effusion [2, 5]. As this case series covered all new postoperative diagnoses and the patient cohort was old and multimorbid, the complication rate could be misjudged in our population according to recently published data [2-4, 6].
In total, 15% of patients (n=8) were revised due to screw or cage dislocation. Literature references on screw dislocation vary within a range from 1.3 to 41% [5, 20-22]. Specifically, low re-operation rate of 1.3% after screw dislocation referred to a significantly younger patient population with an average age of 39 years and initial traumatic fractures – with otherwise healthy bone structure in these young patients [5]. The old multimorbid population of our study showed in 79% (n=42) of cases a degenerative alteration and additionally an osteoporotic or metastatic deterioration of spinal bone structures. Considering these facts, the postoperative revision rate of 15% does not appear to be clinically relevant because it was not increased and remained within the range given in literature.
Four patients (8%) died in this study during the postoperative in-patient stay. Publications on mortality in this context vary between 0.33 and 15% depending on age and size of patient population [2, 4, 5, 23]. These four patients were old and multimorbid, with reduced pre-surgical clinical situation, e.g., spondylodiscitis, and an increased risk of developing post-surgical complication which subsequently evolved into sepsis followed by multiorgan dysfunction and finally leading to death. Comparing to literature and considering the before-mentioned aspects, the mortality rate within this population does not appear to be significantly increased. Furthermore, we could not demonstrate a statistically significant correlation between operated spinal level and death.
Five patients with statistical non-standardized values in the field of operation time, number of transfused RBCs and postoperative hospital stay showed stabilization or an improvement of their overall condition, so these values are no predictors for a negative outcome in these old and multimorbid patients.
In general, patients in our study benefited by improvement or arrest of their complaints, especially in cases with predominant pain (97%, n=36), motoric (n=32), or sensoric deficits (n=17) at 89% each (Figure 1). Based on Nurick score, it could be stated that 40% (n=21) of patients experienced an increase in mobility and gait; deterioration could be prevented in 42% (n=22). Excluding the four deceased patients, only 11% of patients (n=6) revealed a worsening in mobility. Few deteriorations across all these categories could be explained by the fact that initial trauma of the myelon (e.g., with subsequent myelopathy or myelon edema) progressed even after decompression in context of complex spinal surgery. Prolonged existing symptoms, such as spasticity or bladder and rectum dysfunction according to incontinence, improved rarely and were therefore not to be expected a priori. In literature, the success rate for postoperative pain reduction is given at 53% [4], an improvement of the paraplegic motor symptoms is given at a range of 69 - 100% [4, 24]. Good postoperative success in pain control, improvement of sensoric and motoric deficits, and finally in overall outcome within our follow-up period (Figure 1) could be confirmed in our population after complex dorso-ventral stabilization and decompression. Regarding Nurick score and perioperative clinical status (Figure 1, ‘overall outcome’), we could demonstrate an improvement in 88% of patients (n=36) or no further progress in worsening of their condition (n=7) and maintaining mobility.
Because of future demographic changes in our population pillar, the burden of the health care system will be continuing and will stress the institutions. Costs of health care correlate directly to age of more than 65 years in Germany. In 2008, these expenses increased to more than two times higher than those of average citizens [25]. From the age of 85 years and more, health care costs even explode to a five-time higher value than the average (14.840€ vs. 3.100€ on average) [25]. One big part of these costs was not only related to in-patient stays but also to ambulant and out-patient care. Therefore, our results in that case series contribute to providing independence from the need of care for the elderly population concerning mobility, chronic pain conditions, and basic care. In the end, quality of life by taking part on daily and productive activities and by reducing signs of aging plays an important role in these people.
The monocentric non-randomized retrospective design and the compact patient cohort of this study were a general limitation for the reliability of the presented results. Likewise, there is no standardized long-term follow-up period with acquisition of pain and spasticity scales or of the pre- and postoperative quality of life using a standardized questionnaire in this elderly population after complex spinal surgery [26-29]. Besides, the destination after patients’ hospital discharge, should be recorded – whether they are discharged into their home environment or transferred to another institution for further treatment – and that may provide additional information about early treatment success.
Conclusion
High chronological age of patient alone seems to be not an absolute contraindication for complex surgical spinal care, including dorsal instrumentation and vertebral body replacement. Delaying an adequate surgical treatment due to high chronological age may even limit the results for these patients, especially if the treatment has to be carried out later in an emergency situation instead of earlier elective intervention [30].
The decision for conservative care with orthosis treatment, in turn, leads to restriction of autonomy and mobility. This may not only result in more comorbidities, e.g., in case of predominantly bedridden patients, but also in an increasing dependency on nursing support. Thus, the conservative treatment approach – if it was chosen solely because of high chronological age – does not represent an adequate alternative to surgery, neither socio-economically nor from the point of view for primary treatment [24, 31]. When deciding on appropriate treatment modality, the assessment of individual patient risk on the basis of comorbidities should be more weighted, since the risk for development of relevant postoperative complications increases with the number of existing secondary diagnoses. As mentioned before, because of neurological deficits and/or untreatable pain, no control group of patients could be defined in advanced age by withholding necessary surgery. The ethical committee of our hospital would not accept this.
Highlights
i. Elderly patients benefit from spine surgery concerning pain, sensori-motor deficits.
ii. Risk of complications increased due to number of preoperative secondary diagnoses.
iii. Patients’ age alone is not suitable for individual surgical treatment decision.
Conflicts of Interest
None.
Funding
None.
Consent
Informed consent was obtained from all individual participants included in the study and data was prepared for further scientific analysis according to Ethics Commission of the University Hospital Muenster and the Westphalian Medical Association for Human Research (approval codes: 2011-016-f-S; 2019-026-f-S).
Article Info
Article Type
Research ArticlePublication history
Received: Sat 21, Nov 2020Accepted: Mon 07, Dec 2020
Published: Thu 24, Dec 2020
Copyright
© 2023 Christian Ewelt. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited. Hosting by Science Repository.DOI: 10.31487/j.SCR.2020.12.13
Author Info
Murat Yavuz Nils Warneke Michael Schwake Juliane Schröteler Samer Zawy Alsofy Walter Stummer Mark Klingenhöfer Christian Ewelt
Corresponding Author
Christian EweltDepartment of Neurosurgery, University Hospital Münster, Germany
Figures & Tables
Table 1: Demographic overview of the entire study cohort, including patients’ main parameters, indication of surgery, level of corpectomy, and type of complications.
|
Items |
Parameters |
Values |
|
|
|
|
|
patients |
inclusion period (years) |
6,5 (01.01.2010-30.06.2016) |
|
|
|
|
|
|
total collective |
n = 53 |
|
|
|
|
|
|
sex (♀ : ♂) |
31 : 22 |
|
|
|
|
|
|
age at surgery* (years) |
75 (70-89) |
|
|
|
|
|
|
type of secondary diagnosis† |
cardiovascular (CHD, hypertension, arrhythmia) metabolic (DM Type 2) neurological (c. a. ischaemia / hemorrhage) neoplastic (malign) medicamentous (anticoagulation) nephrological (renal insufficiency) haematological (anaemia, factor diseases) endocrinological (thyroid dysfunction) pulmonary (COPD, bronchial asthma, OSA) rheumatoid (arthritis, M. Bechterew, arteritis) |
n = 38 n = 9 n = 10 n = 21 n = 21 n = 7 n = 7 n = 8 n = 7 n = 5 |
number of secondary diagnoses per patient‡ |
0 1 2 3 4 5 6 |
n = 0 n = 6 n = 13 n = 19 n = 7 n = 2 n = 1 |
|
operation |
indication† |
fractures traumatic pathologically (osteoporosis) pathologically (metastasis) infections (spondylodiscitis) degeneration (spondylolisthesis) |
n = 3 n = 15 n = 14 n = 8 n = 13 |
|
|
|
|
|
level of corpectomy§
|
cervical spine thoracic spine lumbar spine |
n = 18 n = 23 n = 14 |
|
|
|
|
|
mode |
single-stage two-stage |
n = 33 n = 20 |
|
|
|
|
|
duration (minutes)* |
475 (241-1057) |
|
|
|
|
|
perioperative |
transfusions (RBC)* |
2 (0-17) |
|
|
|
|
|
|
In-patient stay (days)*, II |
18 (7-98) |
|
|
|
|
|
postoperative |
type of complications (general) |
wound healing disorder nosocomial urinary tract infection pneumonia sepsis organ failure (kidney, liver) myocardial infarction resuscitation pleural effusion pulmonary embolism respiratory insufficiency tracheotomy (long-term ventilation) delirium cerebral (hydrocephalus, meningitis, SH) |
n = 11 n = 5 n = 11 n = 5 n = 9 n = 1 n = 5 n = 27 n = 3 n = 5 n = 7 n = 8 n = 2 |
number of complications per patient‡ |
0 1 2 3 4 5 6 |
n = 13 n = 13 n = 7 n = 7 n = 9 n = 3 n = 1 |
|
|
complications (implant-referred) ¶
|
none screw dislocation in need of revision conservative cage dislocation in need of revision conservative |
n = 37 n = 6 n = 8 n = 2 n = 1 |
|
|
|
|
|
deaths |
n = 4 |
|
|
|
|
*corresponds to: median (range), †preoperative situation, ‡median values bold marked, §two patients each operated at 2 spinal levels, IIno statement about destination after discharge/transfer, ¶one patient with screw and cage dislocation in need of revision. c. a.: condition after, CHD: coronary heart disease, COPD: chronic obstructive pulmonary disease, DM: Diabetes mellitus, M: Morbus, OSA: obstructive sleep apnea, RBC: red blood cell concentrate, SH: subdural hematoma.



References
- F.S. Office (2016) Older people in Germany and the EU, Federal Statistical Office, Wiesbaden.
- Faciszewski T, Winter RB, Lonstein JE, Denis F, Johnson L (1995) The surgical and medical perioperative complications of anterior spinal fusion surgery in the thoracic and lumbar spine in adults. A review of 1223 procedures. Spine 20: 1592-1599. [Crossref]
- Liu Y, Hou Y, Yang L, Chen H, Wang X et al. (2012) Comparison of 3 reconstructive techniques in the surgical management of multilevel cervical spondylotic myelopathy. Spine 37: E1450- E1458. [Crossref]
- Ulmar B, Cakir B, Huch K, Puhl W, Richter M (2004) Vertebral body replacement with expandable titanium cages. Z Orthop Ihre Grenzgeb 142: 449-455. [Crossref]
- Knop C, Blauth M, Bühren V, Hax PM, Kinzl L et al. (1999) Surgical treatment of injuries of the thoracolumbar transition. 1: Epidemiology. Unfallchirurg 102: 924-935. [Crossref]
- Daentzer D, Bianchi N, Böker DK, Deinsberger W (2014) Multilevel segmental interbody fusion versus vertebral body replacement: comparison of two operative methods. Orthopade 43: 156-164. [Crossref]
- Angrés A, Osswald P (1997) Alte Patienten Komplikationen in der Anästhesie. Springer 521-535.
- Jandziol AK, Ridley SA (2000) Validation of outcome prediction in elderly patients. Anaesthesia 55: 107-112. [Crossref]
- Stewart I, Millac P, Shephard R (1975) Neurosurgery in the older patient. Postgrad Med J 51: 453-456. [Crossref]
- Katlic MR (2011) Principles of geriatric surgery, Cardiothoracic Surgery in the Elderly. Springer 25-42.
- Nurick S (1972) The pathogenesis of the spinal cord disorder associated with cervical spondylosis. Brain 95: 87-100. [Crossref]
- V.A. IBM Corp (2016) IBM SPSS Statistics for Windows, NY: IBM Corp.
- W.H. Organization, The world health report 2002: reducing risks, promoting healthy life, World Health Organization.
- Larson EB (1997) Successful aging. An overview. West J Med 167: 204-205. [Crossref]
- United Nations, World Population Ageing (2013) United Nations Publications.
- O'neill A, Rabbitts A, Himel H, Yurt R (2000) Burns in the Elderly: Our Burn Center's Experience with Patients≥ 75 Years Old: 97. J Burn Care Rehabil 21: S183-S183.
- Fortin M, Hudon C, Haggerty J, Akker MVD, Almirall J (2010) Prevalence estimates of multimorbidity: a comparative study of two sources. BMC Health Serv Res 10: 111. [Crossref]
- Akker MVD, Buntinx F, Roos S, Knottnerus JA (2001) Problems in determining occurrence rates of multimorbidity. J Clin Epidemiol 54: 675-679. [Crossref]
- Bussche HVD, Koller D, Kolonko T, Hansen H, Wegscheider K et al. (2011) Which chronic diseases and disease combinations are specific to multimorbidity in the elderly? Results of a claims data based cross-sectional study in Germany. BMC Public Health 11: 101. [Crossref]
- Gertzbein SD, Robbins SE (1990) Accuracy of pedicular screw placement in vivo. Spine 15: 11-14. [Crossref]
- Camille RR, Saillant G, Mazel C (1986) Internal fixation of the lumbar spine with pedicle screw plating. Clin Orthop Relat Res 203: 7-17. [Crossref]
- Vaccaro AR, Rizzolo SJ, Balderston RA, Allardyce TJ, Garfin SR et al. (1995) Placement of pedicle screws in the thoracic spine. Part II: An anatomical and radiographic assessment. J Bone Joint Surg Am 77: 1200-1206. [Crossref]
- Graßhoff H, Franke J, Mahlfeld K (2000) Ventraler Wirbelkörperersatz bei Spondylitis der Lendenwirbelsäule. Oper Orthop Traumatol 12: 197-208.
- Knop C, Blauth M, Bühren V, Arand M, Egbers HJ et al. (2001) Operative Behandlung von Verletzungen des thorako-lumbalen Übergangs–Teil 3: Nachuntersuchung Ergebnisse einer prospektiven multizentrischen Studie der Arbeitsgemeinschaft “Wirbelsäule” der Deutschen Gesellschaft für Unfallchirurgie. Der Unfallchirurg 104: 583-600.
- F.S. Office (2011) High costs of health care: a question of age? Federal Statistical Office, Wiesbaden.
- Ansari NN, Naghdi S, Arab TK, Jalaie S (2008) The interrater and intrarater reliability of the Modified Ashworth Scale in the assessment of muscle spasticity: limb and muscle group effect. NeuroRehabilitation 23: 231-237. [Crossref]
- Bendinger T, Plunkett N (2016) Measurement in pain medicine. BJA Education 16: 310-315.
- Jenkinson C, Layte R, Jenkinson D, Lawrence K, Petersen S et al. (1997) A shorter form health survey: can the SF-12 replicate results from the SF-36 in longitudinal studies? J Public Health Med 19: 179-186. [Crossref]
- Jr JEW, Sherbourne CD (1992) The MOS 36-item short-form health survey (SF-36): I. Conceptual framework and item selection. Med Care 30: 473-483. [Crossref]
- Nusbaum NJ (1996) How do geriatric patients recover from surgery? South Med J 89: 950-957. [Crossref]
- Vahldiek M, Gossè F, Panjabi M (2002) Stabilität ventraler, dorsaler und kombinierter Spondylodesen beim Wirbelkörperersatz. Der Orthopäde 31: 508-513.
